At a hospital battered by COVID-19, some workers say no to the vaccine. Why?
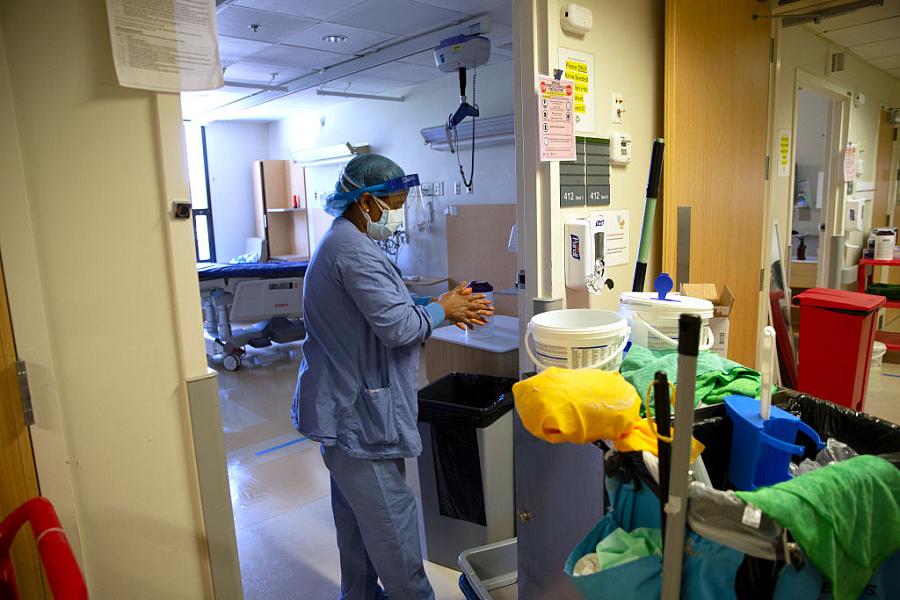
A member of housecleaning services disinfects her hands after cleaning a room in a COVID-19 unit at a Seattle hospital last year.
(Photo by Karen Ducey/Getty Images)
What is the opposite of vaccine-hesitant? Vaccine-delighted? Vaccine-obsessed? Whatever we call it, that was me in mid-December, when the rollout began. As a front-line medical worker in New York City, I had been working in labor and delivery, in a high-risk inpatient unit, and in prenatal clinics for eight pandemic months that seemed like forever. When I was given a vaccine appointment, one of the first available in our hospital — I moved child care and work obligations and mountains to get to it, without question.
At the appointment, I said a traditional Jewish blessing; my nurse said, “Thank you, Jesus,” and injected me in the arm. I wept. It was the week of my birthday.
I was preparing for a heavy week of work over Christmas and New Year’s when I received the vaccine. Supplies were limited, so only the very front-line workers were eligible and we had to be discreet, because so many deserving folks had to wait. Yet the medical system was continuing to notice who our “front lines” really were — not just doctors and nurses, but also the housekeeping staff who scrubbed COVID rooms in the ICU, and the food service workers who kept all of us nourished, and many, many others.
A week or so later, more of the hospital staff was eligible. A few weeks after that, a vaccine was available to essentially any hospital worker who would take it. Soon, vaccine appointments were going begging: availability had outpaced demand.
Some of this was because our hospitals were getting better at vaccine administration: at staffing our sites and lining up eligible recipients, and at matching our supplies to our appointments. But it turns out that we were also zipping through the hospital because a lot of people were saying no.
You have to remember that this was back in January and early February, before the vaccine was available to the general population. The only people being offered the vaccines were workers at hospitals, mostly health care workers, whose livelihood depends on science. And perhaps even more shocking to me, the people declining the vaccine had been on the front line in the health care system most directly impacted by COVID-19 deaths. Reports last summer showed that the overwhelming majority of COVID-related deaths among health care workers happened in New York: 368 fatalities as of mid-September.
The people being offered the vaccine had been watching people in COVID units get sick and die, day after day, for just as long as I had. And they still said “No.” I couldn’t believe it.
To be honest, I still can’t.
Some who declined had already gotten COVID-19 and had laboratory evidence of antibodies. They didn’t feel there was evidence showing that the vaccine had any advantage over their native immune response. This made some sense to me, though the idea is strongly contradicted by CDC guidance, which is very clear that getting a vaccine is advantageous to people who have recovered from the disease.
But many people who never contracted the virus and had no immunity also turned down the vaccine, and I wanted to understand. I’m a chatty person — I make small talk with people pretty much everywhere. So I started to ask. When I bought lunch at the cafeteria, I slid my credit card into the slot with a “Thank you so much! Hey, did you get your vaccine?”
“No,” said the cashier worker. She looked at me, surprised. “You did?”
“Yep, I did. I’m one of the doctors here and I feel so much better since I got it.”
“Hmm,” she said. “No side effects? Huh. I just felt really pushed into it. I wanted to think about it.”
“I actually didn’t have any side effects, though you know, you can, though generally not serious. And I understand,” I said. “But you know this disease is just waiting to get us, especially where we work. Every day wait feels like a scary day, at least to me.”
“Yeah, maybe,” she said. “I’m thinking about it. “
I talked to the guy who works in house cleaning on Labor and Delivery. I have a nice conversation with him most Thursdays when I’m on call. Usually we talk about how his kid is doing in school or where he’s planning to go on vacation. I know he also works next door, at the converted COVID ICU, which has seen many deaths.
The first time, I asked him if he got his vaccine, and his answer was minimalist: “Yeah, I know. I gotta look into that.” I just said, “Yeah, I know. I just feel so much less guilty about bringing this virus home since I got vaccinated, you know? It’s not just us living under this cloud — it’s our families too.”
The second time, he started the conversation. He had done some research and found out that Dr. Fauci had gotten the Moderna vaccine. Our institution was offering the Pfizer version. “I’m going to wait for the Moderna,” he said “That Fauci guy knows what’s what.” I told him that Fauci would tell him to grab a vaccine, any vaccine, as soon as he could, but he shook his head at me.
The most recent time, he just waved at me, and I didn’t feel I should mention the vaccine at all. In the end, I’m a doctor at this institution, and he’s a member of the housekeeping staff. That is a power differential that no amount of small talk can eliminate. And if he didn’t want to talk about the vaccine, pushing him on that felt like using that power, even if I meant to protect him. So I waved back as I left, and I haven’t mentioned it with him since.
There are many opinions about vaccine hesitancy. A lot has been written about people of color, and the legitimate mistrust that medical trials have earned since the notorious Tuskegee experiments on Black people with untreated syphilis, in the 1930s. But talking about an almost century-old unethical experiment assumes that COVID-19 vaccine distrust is rooted in inequitable treatment of the past, and that’s not true. Unfortunately, that inequitable treatment is very much present. COVID-19 pandemic data about complications and deaths continues to demonstrate how much worse the pandemic has been for communities of color: not long ago but today. That well-deserved mistrust of medical treatments is real, and needs to be explored and addressed at length.
But the vaccine hesitancy I see isn’t unique to people of color. It spans ethnic, racial, and socioeconomic backgrounds. Some people come from a place of long-standing vaccine mistrust. Some are in the midst of a general crisis of faith about elections and media. Many others are likely responding to the steady erosion of trust in the government over decades, and then I would argue, an abrupt fall in the last year of a mishandled pandemic.
And I can see how it is hard to trust a government that responded to COVID-19 so badly it led to over 500,000 deaths, many of them preventable, and then offers you a new shot of miracle protection. I can see how that might seem too good to be true. I just am not entirely sure what to do about that.
But the diversity of vaccine hesitancy means that there’s no one story here. Everybody has their own reasons for saying no — legitimate or not, or a bit of each — and their own velocity of change toward vaccine acceptance. Some holdouts will be persuaded soon; some will not. Some will get their shot after more effective public health messaging, or when they see how the vaccine has real, immediate benefits — being able to hug their grandchildren again or travel without quarantine. And some will get their shots when work requires it, or when there are things they aren’t allowed to do if they aren’t vaccinated.
And some people won’t budge. We as society will have to decide how much to make that cost.
I started out as a proselytizer of vaccines. But I saw how my conversations hinged on my power as a white woman, as a doctor, as an employer. I saw how careful I had to be about that if I wanted to make ethical change on this issue; if I wanted people to have an unforced choice.
I still talk about vaccines, but more gently, more carefully. That doesn’t seem right, either; this feels urgent and lifesaving. But it’s so easy to cross the line into an overbearing bully, and I am trying to stay on the right side of that line.
And it turns out, change does happen.
A few weeks ago, I was in the COVID ICU, rounding on a pregnant patient with pneumonia who was finally recovering. I heard my name called by a woman around my height. I couldn’t place her identity under the scrub cap and mask, so it took me a good two minutes to realize that she was one of the clerks from our labor and delivery unit, finishing nursing school, and doing rotations in the ICU.
“I had no idea you were in school!” I said. “Good for you!” And maybe because I had just come from the bedside of a sick COVID patient, and because she and I had worked together for a while, I impulsively said, “You got your vaccine, though, right? Before starting this rotation?”
She shook his head and looked down. “Come on,” I said, a panicky note entering my voice. “No, really. COME ON. I’m worried about you. You are a Black woman, you CANNOT get sick. Look where you work. Look how many we’ve lost.”
She sighed: “I know you’re right, Dr. K. I’ll get there. I’m just not there yet. I need some time.”
I wanted to push it; I wanted to convince her. Instead, I bumped elbows, wished her luck, and told her we missed her upstairs.
I recently saw her again in the ICU, across the room. She waved, flashed me her ID, and pointed to the bright, fresh “I got the shot” sticker on the front. I have no idea what got her there, or when or why. But I smiled so big she could see it behind my mask. And she smiled right back.

