This Indiana needle exchange program was a big success — before officials killed it
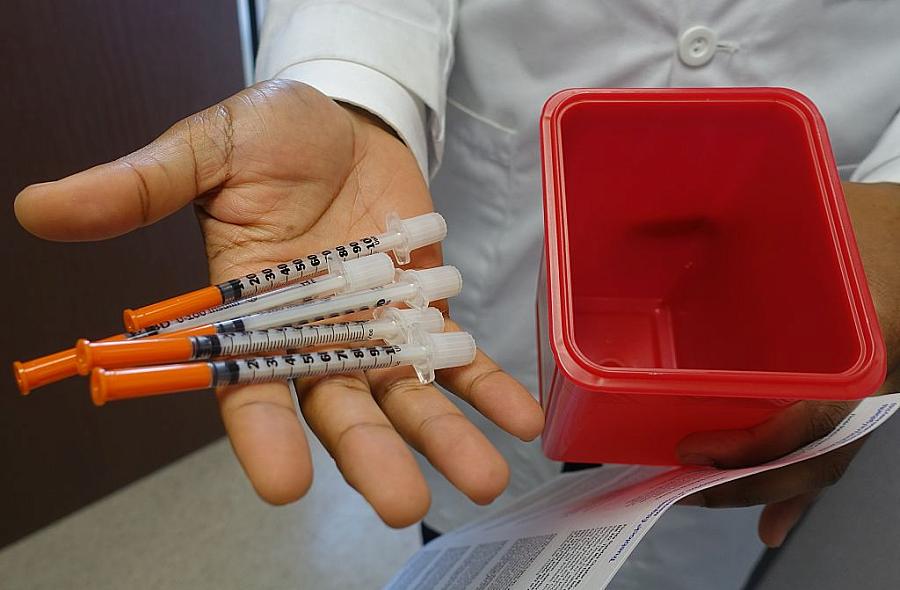
(Photo by Kerry Sheridan/AFP via Getty Images)
The first time I wrote about syringe exchanges was in 2015, a few days after I visited the site of the largest HIV outbreak caused by drugs in American history.
In Scott County, Indiana, a rural county of about 24,000 people near the Kentucky border, dozens of people addicted to opioids had been found to have contracted the disease from sharing dirty needles. The number of cases would eventually swell to more than 200.
In response, then-Indiana Gov. Mike Pence, long opposed to needle exchanges on the grounds they promoted drug use, signed an executive order allowing the county to operate one. Public health experts widely credited the program — where people could pick up free, clean syringes and safely dispose of used ones — with curtailing the outbreak (and found that having one sooner could have averted the crisis).
It seemed like a sea change for harm reduction, a movement that advocates for making drug use safer. Indiana, a red state, eventually legalized syringe exchanges statewide. The number of programs in the U.S. roughly doubled.
Six years later, though, the issue hasn’t gotten any less controversial. Last month, Scott County commissioners voted 2-1 to shut down their syringe exchange.
“I know people who are alcoholics, and I don’t buy them a bottle of whiskey. And I know people who want to kill themselves, and I don't buy them a bullet for their gun,” commissioner Mike Jones said, according to the Louisville Courier-Journal.
The vote happened in the wake of efforts by other government officials to limit needle exchanges. Earlier this year, West Virginia passed a law restricting their operations — a federal judge has halted it for the time being — while legislators in North Carolina attempted to do the same.
This backlash goes in the face of decades of research that has found syringe exchanges not only reduce the transmission of HIV and other diseases, but they also help get people off drugs. These programs often act as a gateway to recovery, referring treatment to people who may not have otherwise gone looking for it.
Last year, I wrote a story for Kaiser Health News about Indiana’s syringe-exchange experiment. As I reported then, even with the documented benefits of the programs, steadfast opposition remained. The exchanges existed in only nine of the state’s 92 counties. Two other counties in the state had closed their programs (one of which eventually reopened).
“Really, the needle exchange was the reason why I even started to think about getting clean,” Cody Gabbard, a former heroin user from Connersville, Indiana, told me.
He said the two women who operated the program were the first people in some time who had treated him like a human being. He said they planted the idea in his head that he could live a better life.
In one study of a Seattle syringe exchange, participants were found to be five times more likely to enter treatment than drug users who didn’t utilize the program.
Arguments against needle exchanges tend to be moral and anecdotal in nature. But that doesn’t make them any less powerful. And they don’t always come from politicians.
San Francisco has been enduring an overdose crisis lately that has people questioning its lax approach to substance use. Last year in that city, drug overdoses killed 713 people, nearly triple the number who died of COVID-19, The New York Times reported.
“What I’m pushing for is an urgency for the city to expand and promote drug treatment for people,” Thomas Wolf, a San Francisco man who is in recovery from drug addiction, told Times reporter Thomas Fuller. “It’s not enough to just hand out clean needles. We need to take it a step further and get you off the street.”
In other words, you can refer someone to drug treatment all you want, but if there’s no treatment for them to go to, it’s a pointless exercise. In 2019, about a fifth of Americans who didn’t get needed help for substance abuse blamed affordability or lack of health coverage, the National Survey on Drug Use and Health found.
The pandemic made it even harder to get treatment. As I reported for Kaiser Health News last July, COVID-19 forced many drug rehab facilities to close or limit their operations. Many syringe exchanges also had to curtail their availability because of the virus.
Meanwhile, 2020 will likely set the record as the deadliest year for drug overdoses in American history. More than 90,000 people died from overdoses during the 12-month period ending November 2020, according to preliminary Centers for Disease Control and Prevention data. The surge in drug deaths in recent years has been largely driven by fentanyl, a powerful synthetic opioid that is often mixed into heroin and other illicit substances.
Many syringe exchanges distribute testing strips that allow people to determine whether their drugs contain fentanyl. They also give out naloxone, a drug that reverses opioid overdoses. Harm-reduction treatment options include prescribing medications like buprenorphine that lessen cravings for more deadly opioids like heroin.
While local and state resistance against needle exchanges continues, the Biden administration included $30 million in its American Recovery Plan for harm reduction programs.
“It’s an enormous signal, recognizing that not everybody who uses drugs is ready for treatment,” Daliah Heller, director of drug use initiatives at Vital Strategies, a global public health organization, told The Times. “Harm reduction programs say, ‘OK, you’re using drugs. How can we help you stay safe and healthy and alive first and foremost?’”
Some countries take their support for harm reduction even further. Nations such as New Zealand and the Netherlands allow people to have street drugs tested to see if they’re laced with dangerous chemicals. Safe-injection sites, where IV drug users are monitored to make sure they don’t overdose, exist in places like Canada, Europe and Australia.
Don Des Jarlais, a New York University professor who has studied syringe exchanges extensively, told me he believes the reversal in Scott County is part of a larger anti-science movement in America, but that the pandemic has led to an increased acceptance of the need for a robust public health infrastructure.
“It’s definitely a substantial setback, but I don’t think it is going to stop forward progress in the country as a whole,” he said. “There's just too much evidence with the benefit of syringe service programs in controlling HIV and reducing HCV (hepatitis C) and getting people into treatment and distributing naloxone for things to come to a complete stop, or even for progress to to stop.”
In an ideal world, no one would feel the need to take life-threatening substances. But harm reduction advocates believe more lives will be unnecessarily lost if we don’t acknowledge the realities of addiction. Whether this approach continues to grow, or is stymied by people morally opposed to drug use in any form, is a story that health reporters will be telling for years to come.

