Journalists and providers share stories of Native American health during COVID-19
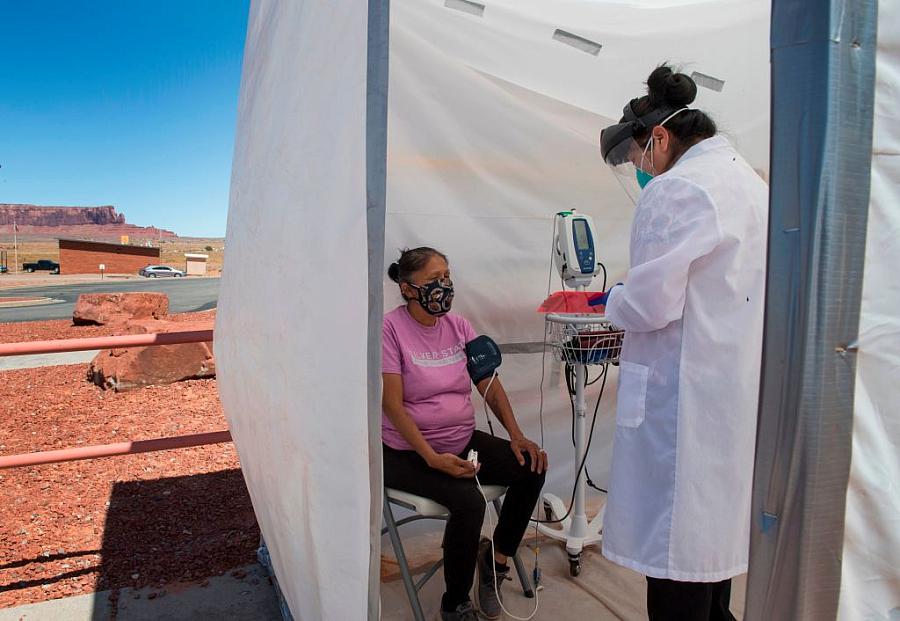
A nurse checks vitals on a Navajo woman complaining of virus symptoms at a COVID-19 testing center in Monument Valley, Arizona in May 2020.
(Photo by Mark Ralston/AFP via Getty Images)
“Take us back to a year ago,” Center for Health Journalism director Michelle Levander asked Dr. Michelle Tom, a Navajo family medicine physician.
“I feel like that would be PTSD. I don’t know if I want to do that.”
Tom paused, “I’m joking!”
She said she’s sleeping better and has a lot less stress and fewer depressed moods. “And the health of our population’s so much better compared to last year it doesn’t even compare. And, thankfully, our vaccination rates are amazing,” Tom said.
Levander was joined by Tom and others for a panel on Native American health and the pandemic for fellows attending the 2021 National Fellowship via Zoom last week.
A year ago Tom was battling to save lives at the Winslow Indian Health Care Center in Arizona near the Navajo reservation, where she said there are about 30 ICU beds for an area the size of West Virginia.
Back then, she and other providers were struggling to get patients into the care of cardiologists, pulmonologists and specialty nursing staff. They spent hours seeking open ICU beds in Las Vegas, Phoenix and Albuquerque. Transfers could take hours. With such delays, Tom said, “your mortality, morbidity goes up tremendously in an acute situation.”
She said people living in remote areas of the Navajo reservation, already isolated, were afraid to come to town. Volunteers and workers were leery of interaction. People living on unmarked dirt roads and lacking electricity, telephone and Internet service, and transportation were vulnerable.
“So it was difficult to get water – even water – out to them,” Tom said. “So, unfortunately, yes, there are people who became very sick or didn't have enough food or firewood or water or protective equipment to protect themselves.” Some died as a result, she added.
Investigative reporter Sunnie Clahchischiligi said the care for Navajo elders was at odds with the message from tribal leaders who kept saying “we've got to protect our elders, we've got to, they're keepers of things.’”
Their message was also at odds with what she uncovered in her reporting. Clahchischiligi, a contributor to Searchlight New Mexico, described the hunger and neglect she found while checking in on Navajo elders last summer, conditions she detailed in her article “Navajo elders: Alone, without food, in despair.” “You saw how heartbreaking that was and how difficult it was,” she said.
She said, “It was a tough one to write because I had to tell people — I had to tell the world — that we were falling short while also trying to tell them that, you know, ‘We're trying to do the best we can to keep people alive.’ So it was a tough one.”
Tom said the problems ultimately stem from colonialism. Promises of health care and education in exchange for land and resources were not kept, Tom said. And the pandemic came after decades of underfunding of infrastructure.
Clahchischiligi said her story prompted her to think deeply about what she was doing for her community. She plans in the coming months to announce the creation of a fund to collect money for elders in need.
In Montana, Dr. Jennifer Show, Assiniboine, puts her Ph.D. in nursing practices to work as a family nurse practitioner for Fort Belknap Indian Community Tribal Health.
She said early in the pandemic, the tribe sent people to work from home, and promoted masks and social distancing. However, multi-generational households are not uncommon among the Assiniboine (Nakoda) and Gros Ventre (Aaniiih) tribes of Fort Belknap, with up to eight families in one household.
“That made it impossible for individuals to quarantine,” Show said.
She credited Fort Belknap’s nine public health registered nurses with many of their pandemic successes.
“They're all from this community or have grown up in this community. So they know their community members very well. The nurses know the families.” When a positive test result showed up they were able to get in touch with extended family right away, Show said.
And their messages about masks and social distancing carried weight. “So, really that was kind of our saving grace, that we had these nurses who were so in tune with the community that you just listen to what they're telling you.”
Close ties also put a face on the pandemic. “Everybody knew someone who had either died from COVID or was in the ICU or now was needing oxygen. And so word of mouth, everyone knows everyone, everyone's a relative to everyone, it was personal,” Show said.
“And so that when it came to the point people were getting vaccinated, they were lining up, they were just kind of just exhausted. So we're thankful for that, that everyone was stepping up and getting vaccinated,” Show said.
Indigenous Communities Reporter Nora Mabie, with the Great Falls Tribune, said tribes in Montana achieved a 70% vaccination rate, compared to a 48% rate among the state’s overall population.
She credits the Indian Health Service’s centralized health care system. “They had records. And they had contacts. They had people's names and numbers, and they knew people's comorbidities.” As soon as the vaccine became available, the Indian Health service was making one-on-one calls to elders to schedule vaccinations, said Mabie.
Meanwhile, “where I live in central Montana, we were doing sort of an online thing, where you had to know when you were eligible, and you had to sign up at 9 a.m. on a specific day online. And it was sort of like an internet roulette situation because all the slots would be filled. It was particularly hard for elderly people here.”
Mabie said tribes also offered incentives. The Crow Fair, which includes a rodeo, powwow and parade, was canceled last year. She said the Crow tribal chairman earlier this year told tribal citizens, “‘If you want to have Crow Fair, we need to get to a certain percent fully vaccinated.’” The fair starts August 19.
“They had records. And they had contacts. They had people's names and numbers, and they knew people's comorbidities,” said Nora Mabie of the Great Falls Tribune. As soon as the vaccine became available, the Indian Health service was making one-on-one calls to elders to schedule vaccinations.
The Blackfeet Nation made the reopening of a gate to Glacier National Park contingent on high vaccination rates. The closed gate had impacted dozens of reservation businesses dependent on visitor traffic. The Blackfeet tribe is 100% vaccinated, she said.
Mabie said community-specific messaging also seemed to help. The Blackfeet ran a public service announcement featuring a reservation dog puppet that spoke in Blackfeet and told inside jokes.
Still, Mabie said, a study of COVID-19 last year showed that “Native Americans accounted for 19% of the COVID cases in Montana and 32% of COVID deaths in Montana, even though they only represent 6.7% of the population, so it's just a huge disparity.”
Mabie said as a non-Native journalist covering Native communities, she’s worked at building relationships by showing up, being consistent, and showing she’s interested.
Clahchischiligi said, “I think the best advice I can give for working in a community that is not your own is one that's not even that magical. It's just being human, and knowing that you know people are going through things, being conscious of what people are going through, and what they want.”

