The Health Divide: Black Americans’ deaths of despair overshadowed by whites
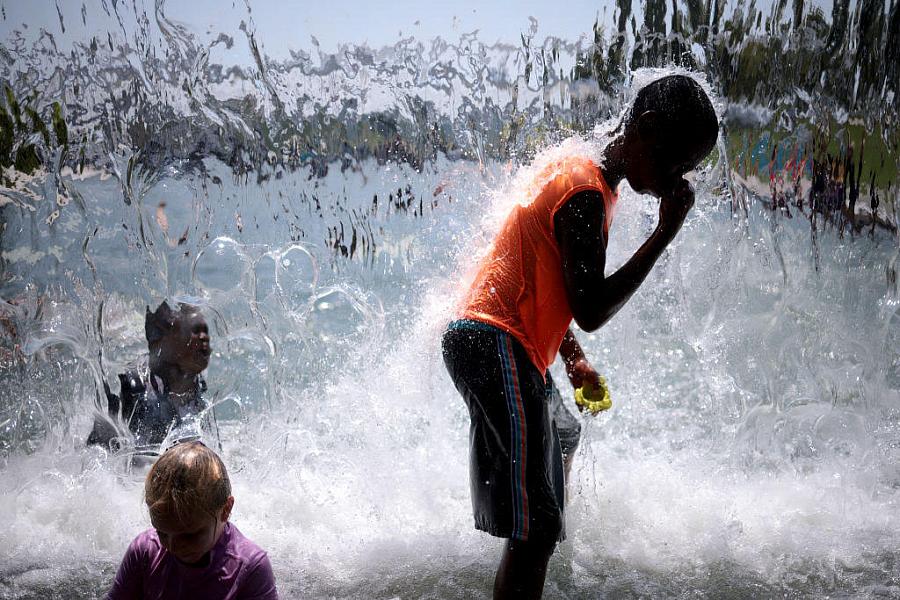
A lack of government support to prevent heat-related illness and death has left some Black communities taking a grassroots approach, reports Adam Mahoney at Capital B.
(Photo by Win McNamee/Getty Images)
Deaths of despair in people of color went overshadowed by white deaths
Deaths linked to suicide, drug overdoses and alcohol-related diseases — so called “deaths of despair” — have gotten lots of attention in white populations in recent years, even as rates among Black people almost tripled between 2015 and 2022, as Jennifer Porter Gore writes at Word in Black.
Princeton University economists Angus Deaton, a Nobel laureate, and Anne Case first sounded the alarm on deaths of despair nearly a decade ago, and at the time, the phenomena was thought to center on white individuals with no college education and reduced socioeconomic circumstances, Gore reports.
But a new analysis in JAMA Psychiatry, led by UCLA researchers, counters the racial elements of the narrative.
“The gap has closed, and it’s moving in the other direction,” author Joseph Friedman told Word in Black. “While the opioid crisis did raise drug overdose deaths among white Americans for a time, it was an anomaly.”
Friedman and Helen Hansen report that Black deaths of despair rose sharply starting in 2015, spurred by illegal drug use and alcohol-related deaths. The death rate for Black Americans surpassed whites’ rate when it hit nearly 104 per 100,000 people, compared to less than 103 per 100,000 for whites.
The same researchers reported in 2023 that Native American communities had the highest rates of deaths of despair.
“It’s important that these inequalities are shown and discussed, rather than hidden, so that we can mobilize resources to work to improve them,” Friedman said in a 2023 UCLA press release.
Friedman and Hansen found that the original 2015 work on deaths of despair didn’t fully incorporate racial inequities in access to education and health care, income and incarceration — all of which can exacerbate mental health and drug use. Thus, Gore writes, “the Princeton study distorted conclusions about who was most at risk of death of despair.”
Biden’s change to credit reports will benefit underserved populations
A new federal rule to keep medical debt off of credit reports should benefit women, African Americans and people with disabilities who disproportionately suffer credit hits from unpaid medical bills, reports Darreonna Davis at The 19th.
The proposed rule from the Consumer Financial Protection Bureau would prevent credit reporting companies from sharing past or new medical or dental debt information with lenders, and block lenders from using medical information for loan decisions.
According to the Bureau, 15 million Americans have medical debt — averaging more than $3,000 — on their credit reports. Those living in low-income communities and in the South are more likely to suffer credit dings from medical costs.
“Medical bills on credit reports too often are inaccurate and have little to no predictive value when it comes to repaying other loans,” the Bureau’s director Rohit Chopra said in a press release.
The rule is open for comments, and will take effect no earlier than 2025, reports Rob Wile at NBC News.
Despite previous efforts to reduce medical debt on credit reports, a Kaiser Family Foundation report earlier this year found that such debt persisted and was more common in people with disabilities, Black individuals, low- and middle-income adults, and people in rural areas and the South. Women also had slightly higher rates of debt than men, which could be related to women’s lower average incomes and childbirth costs.
“Since we know that Black adults and women are more at risk of having medical debt, then I would expect this policy would benefit those groups,” KFF vice president Cynthia Cox told The 19th.
Vice President Kamala Harris said the change would give affected individuals an average 20-point boost to their credit ratings and could help about 22,000 more mortgages be approved every year.
But the new rule would not address the true problem, added Eva Stahl, vice president of public policy at the nonprofit Undue Medical Debt, which is that “people don’t have access to affordable high quality health care.”
Black neighborhoods take summer heat safety into their own hands
As the summer heats up, a lack of government support to prevent heat-related illness and death has left some Black communities taking a grassroots approach, reports Adam Mahoney at Capital B.
This summer is expected to be hotter than usual, and heat-related mortality rates are highest in Black and Native American populations, according to the CDC.
While a handful of states have passed regulations that aim to protect citizens from heat, they tend to be ones with low Black populations. Florida and Texas, which have large and growing Black populations, have blocked ordinances to protect people from heat.
“It’s these discrepancies that are driving neighborhood groups to take control,” writes Mahoney. “Across the nation, Black neighborhood associations, community land co-ops, and nonprofit organizations have led heat preparation workshops, shared resources for water, fans, and transportation, and planned disaster networks that prioritize checking on elders and the most vulnerable during oppressive heat waves.”
Pew generates controversy in survey on Black Americans’ views on health care
About half of Black adults believe the U.S. health care system intentionally holds them back, and just over half believe medical researchers currently experiment on Black people without their knowledge or consent.
That’s one of the headline findings of a Pew Research survey on Black Americans’ views, reports Steven Ross Johnson at U.S. News & World Report.
The statistics illustrate the ongoing mistrust Black people feel towards the health care system, Johnson writes, creating a barrier to addressing health disparities in the nation.
But Pew has faced blowback for using the term “racial conspiracy theory” to describe Black people’s attitudes towards a variety of institutions. The researchers applied the term broadly, casting the belief that institutions have been deliberately used to harm Black people as a “conspiracy theory.”
“The problem here is that, historically, this has often been true,” writes Ja’han Jones at MSNBC, “from redlining to the Tuskegee syphilis study to gerrymandered voting districts that diminish Black voter power.”
DeAnna Hoskins, president of JustLeadershipUSA, called the terminology “shockingly offensive” in a statement. Saying “conspiracy theory,” she notes, implies that “other explanations are more probable.”
Study author Kiana Cox told Jones that she struggled with the negative connotations of “conspiracy theory” but ultimately decided it fit. Pew has since added an editor’s note stating the report is under revision and that the term was “not the best choice.”
The report did find that Black people had higher levels of trust in the health care system than in other institutions, such as prisons, courts, and the political system.
Efforts by health care systems during the pandemic, such as the use of mobile clinics and transportation assistance, helped improve the relationship between health care and marginalized communities, Dr. Georges Benjamin, executive director of the American Public Health Association, told U.S. News & World Report.
“Now that we know what works,” Benjamin said, referring to expanded access to health care, “we need to scale it up and we need to integrate them into our normal practice.”
From the Center for Health Journalism
July 10 is the deadline to apply for our Data Fellowship, which offers journalists an opportunity to transform their reporting by training them to “interview the data.” Fellows graduate from this hands-on training program, held Oct. 7–10, prepared to produce either a major investigative or explanatory health reporting project or a series of individual data-driven health stories that focus on issues important to their communities. Admitted Fellows receive a $2,000 stipend and five months of professional mentorship. Learn more here!
Webinar July 31, 10–11 a.m. PDT: Disappearing Options: Tracking the Story on Reproductive Health Care.
What do journalists need to know? Join our expert panel to discuss the latest developments, analyze their impacts on care, and uncover timely stories. Featuring Shefali Luthra of The 19th, Maya Manian of the American University Washington College of Law, and Eleanor Klibanoff of The Texas Tribune.
Free. Sign-up here!
What we’re reading
- “As pharmacies shutter, some Western states, Black and Latino communities are left behind,” by Tom Murphy and Kasturi Pananjady, AP News
- “Cancer researchers begin large long-term study of Black women,” by Roni Caryn Rabin, The New York Times
- “The short reach of long COVID care,” by Lygia Navarro, palabra. and WHYYs The Pulse
- “NIH wanted to make cancer research more diverse. The effort turned out to be a costly failure,” by John Wilkerson, STAT
- “This innovation could revolutionize kidney care of Black patients,” by Margo Snipe, Capital B
- “End of internet subsidy leaves millions facing telehealth disconnect,” by Sarah Jane Tribble, KFF Health News

