Racial disparities in study reveal the dangers of using formulas to ration care
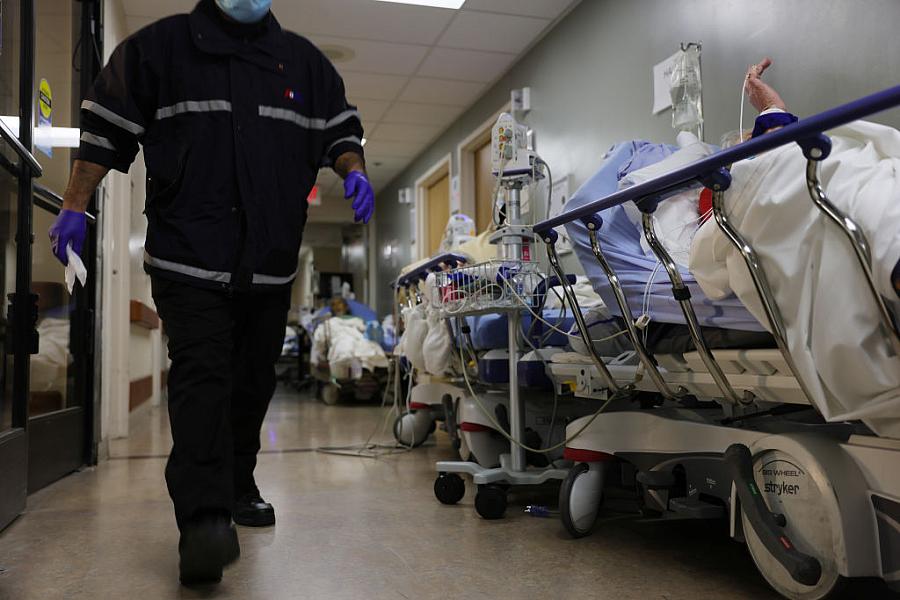
(Photo by Mario Tama/Getty Images)
There are many reasons why African Americans have died at disproportionate rates during the COVID-19. But some of the reasons why people of color might get worse health care during a pandemic are more subtle and insidious than we might think.
For example, racial disparities found within a recent study from the Yale New Haven Health System suggest that a widely used tool for allocating resources among incoming patients tended to disadvantage African American COVID patients.
“The U.S. health care system and health care systems globally have been moving increasingly towards adopting algorithms and predictive scores to help to allocate resources in effective ways,” said Dr. Benjamin Tolchin, director of the health system’s Center for Clinical Ethics and one of the authors of the study. “Our findings emphasize the importance of testing those algorithms and predictive scores empirically for potentially inequitable outcomes that are not intended by the folks developing them, but may have very serious consequences for their use.”
During the first wave of the COVID-19 pandemic, the Yale health system turned to a scoring system that helps doctors calculate a patient’s odds of survival. The idea was that the score could help the health system triage care and scarce resources during a COVID-19 surge.
A high organ failure assessment score (known as a SOFA score in the lingo) assumes a higher likelihood of death, and the need to direct resources to patients with a better chance of survival.
Although the Yale health system never reached that crisis point, researchers there decided to use the electronic medical records of their COVID patients to study their SOFA scores. The goal was to see whether the triage scores among patients of color might lead doctors to divert resources from the populations most in need.
The team’s findings confirmed their fears: Black patients were more likely to arrive at the hospital with a higher SOFA score than white patients. Surprisingly, there was no significant difference between the SOFA scores of Hispanic patients and non-Hispanic white patients.
That’s important, Tolchin said, because essentially all crisis standards shift resources to patients who need those resources but have lower, less ill scores — including those currently in use in Alaska and Idaho. “The concern is that if Black patients are at great risk of having an elevated SOFA score compared to white patients, they’re at risk of being denied life-saving medical resources compared to white patients when admitted to the hospital with COVID.”
The study’s data didn’t answer the question of why Black COVID patients were coming to the health system more acutely ill, but Tolchin and his team hypothesized that factors such as a distrust of the medical system, an expectation of lower quality care, and less ready access to health care and insurance could all be at play.
Interestingly, the team didn’t see any significant disparities between Medicaid patients and those with private insurance, further suggesting that the higher intake scores seen in Black patients had more to do with issues specific to their race, rather than economic status.
During the multiple waves of pandemic surges, health systems around the country put in place plans and procedures in case doctors were forced to ration care if hospitalizations overwhelmed available ICU beds and key equipment, such as ventilators and dialysis machines. Early on, many health systems looked to the dire situation that overtook Lombardy, Italy, a town with a robust health care system that was nonetheless devastated by a crush of ill patients.
Meanwhile, the nation’s ongoing reckoning with systemic racism collided with the pandemic last year, intensifying a trend of deeper reporting into how some of the algorithms baked into key decisions at hospitals may create or worsen health disparities.
The problems aren’t limited to triage scores. For instance, a recent article by reporter Roni Caryn Rabin for The New York Times explored how a common measure for measuring kidney function provides different assessments for Black patients, possibly making them seem less sick than they actually are. And an article last year from the late, revered science writer Sharon Begley at STAT examined whether racial bias skews a popular algorithm used to “guide patient care on everything from who receives heart surgery to who needs kidney care and who should try to give birth vaginally.” In 2019, reporter Starre Vartan of Scientific American wrote about a study published in Science that found that a health care risk-prediction algorithm used by hospitals and insurance companies to determine which patients require more “high-risk care management” demonstrated racial bias.
While Tolchin is heartened by the increase in reporting on the algorithms and tools behind crisis standards of care and other major health care decisions, he argued that not enough attention is being paid to the reasons why health systems end up needing to triage patients and the steps that should be taken to avoid this in the future.
“Those are questions that are not going to be addressed by a crisis standard of care, but rather our health insurance system, our tax code, universal health care, and the presence of marginalized populations in the health care workforce,” he said. “Those are the measures we should really think about in addressing the disparity that we’re seeing here.”
**

