Searching for clarity in North Carolina’s infant mortality racial gap
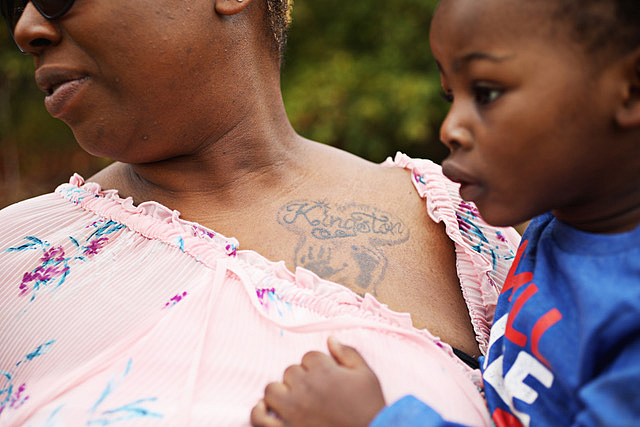
My project on racial disparities in infant mortality in North Carolina depended on women talking about their experiences. These stories helped to propel readers through data-heavy articles. I also knew that finding people was going to be the hardest part.
North Carolina has one of the highest infant mortality rates in the nation. As is the case in the rest of the country, African-American babies die at twice the rate of white babies.
As I reported these stories, I found that few people knew about this health disparity.
After the articles were published, I heard, and some of my sources heard, from women who thought patterns of infant deaths were only in their own families. One caller said, “I thought I was the only one.”
Before I attended the reporting fellowship week, I did a fair amount of groundwork in the search for African-American women to talk to me for the project. I contacted sources who had health-care program contacts, advocacy groups, and members of state-sponsored organizations that focus on maternal and infant health.
I did not have those women lined up for interviews before the fellowship week in California. While there, I realized I was getting a late start.
Upon returning from Los Angeles, I began to look for people in earnest. I contacted more health care organizations and advocacy groups. I was hoping to use some of my sources to vouch for me, explain the series and why I was asking people to participate.
Early on, this approach appeared to be working.
Through a source, I connected in August with a woman who had untreated diabetes before she became pregnant. I had planned for her to be the foundation of a policy story centered on Medicaid expansion. Unfortunately, she bowed out before our first interview. I never found anyone else appropriate to anchor that article, which I then had to restructure.
I searched Facebook, GoFundMe, death notices, and obituaries for leads. ProPublica sent me names of people from North Carolina who responded to a call-out on maternal mortality. We did our own call-outs in The News & Observer, but no African-American women responded.
Only one of the dozens of sources I asked to help connect me to potential participants resulted in an interview with a mother that I was able to include in the work. I found on my own the two women featured in the first article.
Having intermediaries make introductions would have been preferable, but I should not have counted on it.
I found one of the mothers when I attended a meeting of black doulas, where I was able to talk about what I was doing and why. In the course of my reporting, I also attended the meeting of grieving black mothers, and a black mothers’ breastfeeding group. While none of the mothers I met there participated in the series, I made some good connections, and hearing their stories informed my approach to interviews and my writing.
The data I used was readily available. North Carolina publishes infant mortality data each year, and the information is available online. A state task force produces an analysis of infant deaths each year. It includes causes of death and ages, and has mortality rates by county and region.
Though what the state produces is adequate, I should have looked sooner at the state’s death database, and gotten the newspaper’s database editor involved with the project sooner.
I gained some insights from looking at that raw data, which includes causes of death that don’t translate neatly into the state’s official reports.
The issue of unsafe housing and the impact on health was thrust into public view as I was finishing the final drafts. Carbon monoxide leaks at a public housing development were making people sick. Three infants died in the neighborhood in the space of weeks; two in public apartments and one at a neighboring boarding house.
Although two of those deaths were found not to be due to carbon monoxide poisoning, parents questioned whether the dilapidated condition of the apartments - rampant mold growth, leaking pipes, and poorly regulated temperatures - contributed to the deaths.
While it was too late to fully develop this angle, addresses in the database could have been used to map deaths and identify potential clusters.
While I knew finding people would be hard, I thought finding a place in the United States that had narrowed the racial infant mortality gap would be easy. Cities, counties and non-profits throughout the country are trying to do this.
Initially, I wanted to travel to an established Best Babies Zone to report on its projects and results.
Best Babies Zones use a “whole community” approach to improving overall health. I was looking for a community in a state somewhat comparable to North Carolina that had worked to achieve an infant mortality rate for African-American babies that was lower than North Carolina’s. That’s a small universe of possibilities, but Wake County, the capital county in North Carolina, inaugurated a Best Babies Zone last year, and I thought reporting on an established project would make for interesting parallels.
Early on, I hoped to go to a Best Babies Zone in New Orleans. I found in late summer that the project no longer existed.
I searched for another Best Babies Zone, but I did not find one that fit my criteria.
I shifted my focus to other community projects. I contacted a project in Washington, D.C. that I thought would be a good fit, but I was not able to finalize arrangements for a reporting visit.
My other options were doula and visiting nurse programs. I was contacting non-profits and considering options when the focus of my newsroom shifted to covering the pandemic.
