For series on doctor shortages, reporter tackles a local health story as big as the U.S.
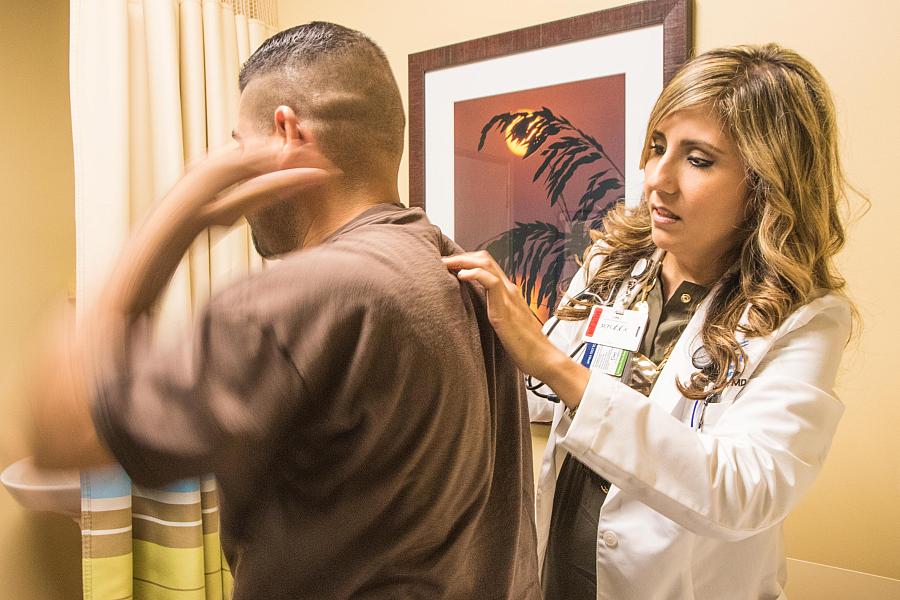
Dr. Olga Meave, who studied medicine in Guadalajara, Mexico before completing her residency in Bakersfield, sees a patient. Nearly half the San Joaquin Valley’s 5,000 doctors are international medical graduates, which leaves the region’s doctor pipeline vulnerable to changes in immigration policy. (Photo by Kerry Klein)
California’s San Joaquin Valley is facing a growing shortage of doctors. This region of roughly 3 million residents has 35 percent fewer physicians per capita than what the federal government recommends — a scarcity that can exacerbate medical problems and disproportionately affects disadvantaged populations.
It’s a trend that’s growing nationally — some groups estimate the entire country could be short of at least 40,000 doctors by the year 2030 — but areas like the Valley have been hit far harder than others. The Bay Area, for instance, counts twice as many primary care physicians per capita as the Valley’s most impacted counties.
When I began asking why the problem is so acute in this region, I expected the answer to be relatively simple, if also dissatisfying: As even the locals admit, the Valley just isn’t as desirable a place to live as bigger urban centers like San Francisco and Los Angeles. After all, as state Senate President Pro Tem Kevin De León once quipped about the Valley, “No one lives out there in the tumbleweeds.”
But the story is so much bigger than that. By the time I was finished, my reporting had covered not only the Valley’s marketing problem, but also federal and state laws dating back decades, executive orders, bills in Congress, visa programs, and more local, state-level and national trends than I could count. All of these have either influenced the growth of the region’s doctor shortage or promise to shape its future.
The problem itself is tangible and quantifiable. It was in investigating the root causes and consequences that I encountered challenges.
The first was finding knowledgeable sources. For a problem that can reach into any home and affect individuals so intimately, I was surprised at how difficult it was to find interview sources who could speak authoritatively about the subject. Professional medical organizations at the state and national level have been warning about the problem for years, and medical educators are certainly concerned about the doctor pipeline, but on the local scale, stakeholders have done little to organize themselves around the physician workforce issue. Local health advocates and nonprofits generally focus on public health rather than health policy, and providers themselves seem so overworked that they have little time to gather and advocate.
The second was the scope of the problem. The shortage is local, but so many of the forces that shape it either originate outside the Valley or impact a geographic area far beyond it. Plus, studies show that access to doctors is already lacking in regions like the Valley with substantial rural populations and high Medi-Cal enrollment — a confluence one source referred to as a “perfect storm.”
Moreover, complex problems — and a lack of organized stakeholders — mean there are no clear-cut solutions. In this convoluted web of laws, trends and demographic disadvantages, there could be no single solutions-based story — just incremental ones. Increasing local opportunities for graduate medical education could help the Valley retain doctors, but a Clinton-era federal law limits the growth of teaching hospitals. On paper, California pharmacists can now take on some responsibilities of primary care providers, but a law that would reimburse them for it is stuck in legislative purgatory. The very same pipeline that supplies doctors who fill in the Valley’s gaps in care — a path to citizenship for international medical graduates — is vulnerable to current changes in federal immigration policy.
Amid this swirl of policies and numbers, it was easy to forget that this wonky issue can impact people in direct and sobering ways. I knew my reporting would need more voices beyond health policy experts. With the support of a community engagement grant from the Center for Health Journalism, I experimented with two new strategies for deepening my reporting by engaging my audience.
For the first experiment, our station ran an on-air promo inviting listeners to call in with stories about doctor shortages from their own lives. It proved to be an overwhelming success: Over the course of the project, we received 34 messages, with stories ranging from long appointment wait times and long drives to harrowing trips to the emergency room and months of missed work while waiting for appointments with specialists.
These messages proved invaluable in humanizing the story for me. They led me to a woman who eventually became one of my main characters — a flute teacher on Medi-Cal who had to wait so long for a new appointment she ran out of vital medication — as well as a local specialist who appeared in two of my stories. Many others, whose voices may not have appeared in my stories themselves, did ultimately get an audience on a map we assembled of testimonials from across the Valley.
Our second community engagement strategy, a panel discussion I moderated about the shortage, was so popular that we had to turn people away. The event attracted community stakeholders I hadn’t previously met, and it drove home just how important this issue is for the community. The panelists themselves were so articulate and knowledgeable that I returned to them regularly throughout the project.
Just as there are no easy solutions to the Valley’s doctor shortage, there are no easy ways to tackle such a far-reaching subject. But when the issue resonates so deeply in the community, reporting on it requires time, creativity, and attention to ensure there’s no shortage of voices sharing their stories.

