Challenges and cultural barriers faced by Asians and Latinos at the end of life
JoAnn Mar's report for KALW was produced as part of a larger project for the USC Annenberg Center for Health Journalism's 2018 California Fellowship. This story also ran in the Oakland Post.
Other stories in this series include:
Racial Disparities in End-of-Life Care— How Mistrust Keeps Many African Americans Away from Hospice
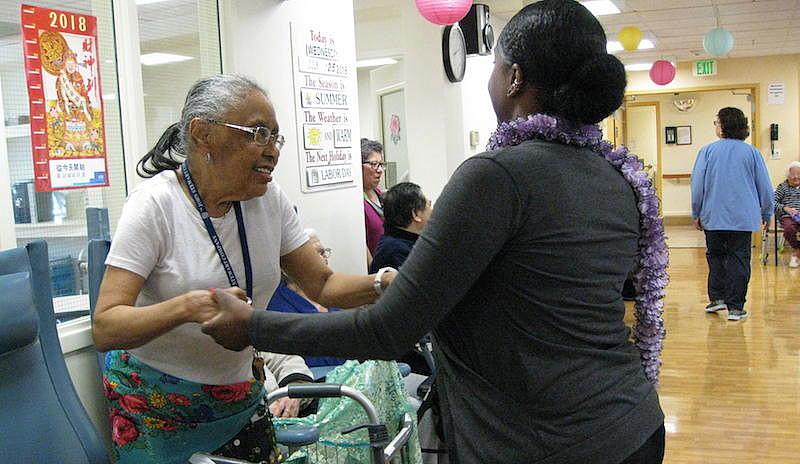
For Asians, Latinos, and other ethnic minorities, the end of life presents unique challenges. Language barriers and cultural traditions can often inhibit access to hospice, pain management, and comfort care.
Overcoming barriers and navigating cultural norms is not easy and requires health professionals and patients working together as equal partners.
The end of life is not easy for most Americans nearing death. The good news is that up to ninety percent of pain and suffering can be controlled. But the bad news is that over half of all dying Americans experience unwanted pain and suffering during their final days. And the numbers are even greater for people of color. African-Americans, Asians, and Latinos have less access to the pain medication and comfort care that hospice can provide at the end of life compared to whites.
Asians, Latinos, and other ethnic minorities whose second language is English face additional challenges. Language barriers and cultural traditions can inhibit awareness of and discussions about end-of-life options and are often compounded by poverty and lack of education.
The cultural taboo against openly discussing death
In many traditional Latino and Asian cultures, speaking openly about death is taboo, especially when a loved one is seriously ill. Among the Chinese, talking about death, especially with elders is considered disrespectful.
At a recent gathering, grief counselor Terri Daniel spoke with Chinese seniors residing at Mercy Housing, a low-income assisted-living community in San Francisco. The elders told Daniel they’ve spent a lot of time and thought setting up altars in honor of deceased ancestors and paying regular visits to the cemetery—but have not spent time making plans for their own deaths. Daniel asked how many of them have had end-of-life conversations with their children. Only six out of twenty-five seniors raised their hands. Fang Huang, resident services coordinator, said she and others at Mercy Housing have tried to encourage the elder residents to talk with their families and complete advance directives. When asked why they hadn't spoken with their families, one woman said they didn't want to discuss death with their children because they were afraid it would upset them. Another woman said, "My children are actually even more fearful than us."
Failure to plan for the end of life
Only one-third of Americans have completed an advance directive, a legal document that specifies a person's preferences for medical treatment in the event of a serious or terminal illness. Whites are more likely to have an advance directive than other racial and ethnic groups. Latinos and Asians are less likely than whites to discuss their end-of-life preferences or engage in advance care planning. Less than ten percent of Latinos have announced or written down their preferences about the kind of care they would want at the end of their lives.
These inequities have serious ramifications. Patients who engage in advance care planning (end-of-life conversations with family or health providers) are less likely to die in the hospital or to receive futile intensive care. Family members have fewer concerns and experience less emotional trauma if they have the opportunity to talk about their loved one's wishes. "Making sure that we talk to people and prepare people in advance for these serious illnesses—that's what we're trying to promote nation-wide," said Dr. Alexander Smith, one of the many concerned palliative care specialists in the Bay Area seeking to improve care at the end of life, "More importantly is understanding what their goals and values are. What type of life is worth living? What kind of trade-offs are they willing to make in order to have that type of life? These are the kinds of conversations that are very important and help family members prepare."
Poverty and the tendency to delay seeking treatment
Luis Hernandez’ family did no planning around the end of life. Hernandez and his brother were raised by their single mother in the projects of Brooklyn, New York. "Death is not something we really talked about until it happened," said Hernandez. His mother had been complaining about pain for a long time, and he and his brother urged her to see a doctor. "My mom was always very scared of doctors and never wanting to go," said Hernandez, "No matter how many times me and my brother told her 'Go!' She said ‘I’m scared they’ll find something.’"
His mother waited too long. By the time she finally saw the doctor, she was diagnosed with stage four liver cancer. After emergency surgery, she got sicker and later died in the hospital. Because events moved so quickly, there was no time for Hernandez and his brother to talk with their mother and discuss hospice or alternatives to the aggressive medical interventions she received. "We're not rich white people," said Hernandez, "What time does she have when she has to work nine to six o'clock job? And even on weekends, she's working. Where do you find time to plan all of that out?"
Deportation threats may discourage end-of-life planning
In addition to poverty and lack of insurance, threats of deportation may cause undocumented immigrants to delay seeking medical help or plan for the end of life. Well-publicized cases of “hospital deportation” may further exacerbate fears among undocumented immigrants. “I’m concerned that the overall direction our country has taken, building the border wall, forced separation of families, will have serious consequences, in particular at the end of life,” said Dr. Smith, “It takes very little to prevent accessing services until it’s too late, until you’re really suffering, until you’re dying, until you’re hospitalized in the intensive care unit.”
Lack of health literacy as a barrier
In traditional Latino and Asian cultures, many families often treat illnesses using home remedies and for that reason, tend to delay seeing doctors and put off end-of-life planning. Many Chinese people will use traditional Chinese medicine first before seeing a doctor. Many Latinos and Asians also believe in fatalism—the idea that events such as serious illness or death are pre-determined by destiny—thus they tend to delay seeking treatment in the belief that medical intervention will not affect the outcome.
Misunderstandings around hospice
Hospice is a novel concept among many Asians and is often a misunderstood term among Latinos. Some Asians mistakenly believe that hospice is similar to nursing home care. Among Latinos, even medical professionals mistakenly translate "hospice" as "hospicio", which in Spanish, is a place for orphans, the destitute, or an asylum for the mentally ill. Compared to whites, fewer Latinos and Asians utilize hospice services and are more likely to die in the hospital.
Family members make end-of-life decisions for the patient
Family plays an important role in the end-of-life decision-making process in both Latino and Asian cultures. Personal autonomy is not highly valued among Chineseor Latinos--this runs counter to the individual-based paradigm prevalent in the American mainstream. Among Latino families, a male member, usually the oldest son or uncle, is responsible for making decisions on behalf of the dying family member. The expectation is that if the elected caregiver respects and loves the dying patient, they will insist the hospital "do everything" to keep the patient alive—this can mean another round of chemotherapy or multiple emergency room visits. The children of a Chinese parent will often advocate for aggressive, life-prolonging treatment out of a sense of filial duty.
Asian and Latino family members will often hide a poor prognosis from the dying relative. “Family may want to shield their loved one--‘Don’t tell mother that she has cancer. It's gonna make her depressed, she can't handle it psychologically',” said Dr. Smith, who has done extensive research on racial and ethnic disparities in end-of-life care. In Latin America, even physicians often do not disclose bad news or poor prognosis with their patients and are expected to keep up the patients' hope.
Failure to discuss end-of-life preferences can lead to poor outcomes
"In our own family, we don’t talk about death definitively," said Julie Thai about her family in Vietnam, "We don't talk about it at all because we just love our family members so much that we talk about them as if they're still alive." Thai's parents emigrated to the United States after the Vietnam war, but they kept in close contact with the rest of the family that remained in Vietnam. Thai and her mother were close to Thai's 85-year old grandfather, who told them he wanted a natural death and did not want to be resuscitated. But his family in Vietnam did not have any conversations with him as he was nearing death. Thai's aunt and her cousin took charge of making decisions on his behalf. "I think everybody assumed they would be in charge of his care, that they would do what they felt was right for him," said Thai, "It was never talked about and that's why his needs were not met at the end of life."
When Thai's grandfather was taken to the hospital for the last time, her aunt asked the hospital to do everything to keep him alive. Hospital staff kept feeding him beef broth, even though he was a vegan. "He was very upset, he was crying, he was pulling the IVs out, he was spitting up the food," said Thai, "He just didn't want anything they were giving him." Despite the attempts to save his life, her grandfather went into cardiac arrest and he died twenty-four hours later. "He was caused more pain by them imposing these heroic measures on him, as opposed to just letting him go, which is what he would have wanted," said Thai.
Overcoming cultural barriers and taboos
Trained medical professionals and social workers can make a critical difference in reaching out to ethnic patients and their families and helping them prepare for the end of life. Professional translators are essential to assist medical staff and families and help them overcome language barriers and facilitate conversations with patients. “You should always have a professional interpreter for any serious conversation,” said Dr. Alexander Smith, “You may think your Spanish is pretty good because you took it in college, but that does not rise to the level of professional translation.” All too often, says Smith, so-called “ad-hoc interpreters” are used in place of professionals and this may lead to inaccurate translations. “For example, a family member may have their own agenda, trying to protect their loved one from a serious diagnosis, and they may not translate everything completely,” said Smith, “Nurses, though they may speak the language, may not know how to translate the medical terminology into the other language.”
Educational outreach and good communication also require special training in cultural humility—an awareness of the patient's values, beliefs, and traditions and a willingness to listen closely to the patient. Cultural humility can also mean becoming a student of the patient, forgoing the role of expert, and allowing him to become a full partner in his care. “You have to let the family lead," said hospice social worker Karen McCabe, "Instead of us taking the lead, ‘oh, well we know all about this, we’ll be right over, we’ll tell you what to do.’”
McCabe works at Hospice of Santa Cruz County, which provides home hospice services to patients nearing the end of their lives. Santa Cruz County has a large number of farmworkers and one-third of the population is Latino. Twenty years ago, Latinos made up only three percent of all hospice patients in Santa Cruz. Today, the number of Latinos in hospice has increased to eight percent, thanks to community outreach efforts by the Hospice of Santa Cruz.
McCabe says working with the family and overcoming their fear of hospice is key to providing the patient with good end-of-life care. For example, when explaining hospice, McCabe says she avoids confusing terminology like “hospicio” and instead tells families that hospice means getting all the care they want at home. “I explain that we’re going to be bringing nurses into your home and we’re going to be sending the medicines into your house and we need somebody in your family to be in charge of care and we’re going to teach them what to do," he explains.
On Lok, the gold standard for end-of-life care
On Lok Senior Health Services was created in 1971 in San Francisco Chinatown by a group of Chinese elders who wanted an alternative to nursing homes. The founders believed that traditional models of care were not adequately meeting the needs of the elderly. Today, the majority of On Lok’s seniors are low-income Chinese and Latinos living in three Bay Area counties.
On Lok provides low-income frail seniors with comprehensive services that allow them to stay at home. These services include home visits and clinical care, meal deliveries, transportation, and adult day care.
"Even though it's taboo, I usually say 'I'm your doctor and this is my job and I need to know what you want or what you don't want'," said Dr. Alana Shpal, a primary care physician at On Lok in San Francisco. "And I also bring up that if we don't discuss this now, it'll put their family in a harder place later on and that often helps because they see their family struggling to make a decision and they don't want to be a burden." She added, "I remind them that telling me is a gift they’re giving their family members."
Shpal, who mostly works with Spanish speaking patients, says conversing with them can often be challenging, especially if cultural norms prohibit patient autonomy and discussing death. But thanks to the efforts of Shpal and other staff members, almost all of On Lok's participants have completed advance directives. "It's a crusade of mine, to have everyone document their end-of-life preferences," she says.
On Lok currently serves over 1,500 frail elders, and at the end of life, provides seniors with comfort care similar to hospice. On Lok's innovative program has now been replicated in thirty states.
Hope for the future
Julie Thai and her mother are still recovering from the shock of her grandfather's painful and protracted death. Thai is encouraging her parents to plan for the end of their lives and complete their advance directives, to avoid repeating the mistakes of her grandfather. She recently asked her mother about how she wants to die. "She's pretty comfortable talking about it," said Thai, "She says 'Just let me go.'"
Following the death of her grandfather, Thai graduated from medical school. She’s now a doctor in Flint, Michigan, specializing in family medicine and geriatrics and is trained to help seniors plan for the end of their lives. By having open, honest conversations, Thai hopes to honor her patients’ wishes. In particular, she wants to reach out to patients bound by culture who can’t talk openly about death. Efforts like Thai’s could have a big impact by reducing racial disparities in end-of-life care.
[This story was originally published by KALW.]

