Juan Solis lives a life in the shadows, his health destroyed by valley fever
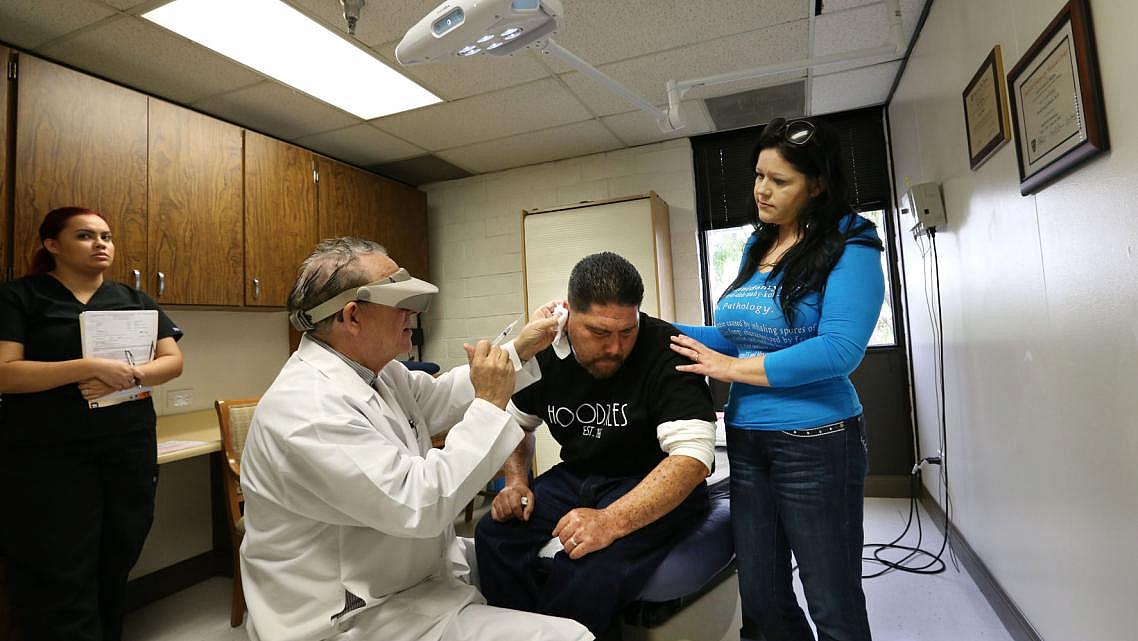
Dr. David Elbaum helps his patient, Juan Solis, who contracted cocci meningitis in 2008, his wife Julie is with him during the dermatologists visit in Bakersfield. Kenya Davalos, medical assistant helps Dr. Elbaum.
(Photo: Casey Christie/The Bakersfield Californian)
Click HERE for Spanish version.
When Juan Solis shuffles out of his dark bedroom, he’s careful not to get too close to the windows.
He makes sure he only walks his dogs at night.
If he must go out during the day, he lathers on sunscreen, makes sure his legs and arms are covered, even during the peak of summer in Bakersfield’s blistering heat. And he never forgets his sunhat.
Juan has extreme light sensitivity, caused by valley fever. He contracted the respiratory disease in 2008, but he was misdiagnosed for so long that he developed complications. The coccidioidal fungus that causes valley fever spread to his bloodstream, causing cocci meningitis, a lethal illness. It kills about 95 percent of patients in the first two years if left untreated, and a 30 percent fatality rate with treatment. The only drug that worked to help control his symptoms was Voriconazole, or VFend, an antifungal drug. There are two problems, though. The drug can cost more than $900 a month. And it has severe side effects, including an outbreak of cancerous lesions on Juan’s skin.
“We can’t do anything except keep taking these pills that are in turn killing you, but it comes down to this: do you want to die really fast or die slower with these pills? You get to pick,” Juan’s wife, Julie, said.
Juan chose to die a little slower. Julie has been hoping for a cure. Valley fever, which is endemic to much of the southwest United States and contracted by the simple act of breathing, has no effective treatment, no vaccine, no antifungal medication that comes without side effects. The extreme light sensitivity experienced by Juan, which in turn has led to his skin cancer, is a very severe side effect for a valley fever patient, and yet, with so few options, Juan knows he likely will be taking those drugs for the rest of his life.
***
Juan had a fever that would not abate, but nobody knew why.
Extreme fatigue took its toll, so Juan stopped going to his job designing trusses for residential homes. His bosses told him to stay home and to come back when his health was in order.
He lost 50 pounds in about two months. But none of the doctors he saw could give him a diagnosis that explained what he was feeling. One recommended going to the dentist for a root canal. Another one suggested an optometrist, wondering if the pressure Juan felt in his head was from eye strain. When Julie asked her own doctor about Juan’s symptoms, she was told he probably had pneumonia.
Meanwhile, the cocci fungus was disseminating into Juan’s bloodstream. Juan’s fever was rising so high he became delirious. He would stumble down the hallway to his easy chair in the mornings and lay there until his wife and kids came home in the afternoons.
Marisol, Juan’s then-6-year-old daughter, would come home and see her once-energetic father, who had coached her softball team, resting in his recliner, pale, sick.
“Is daddy dead yet?” Marisol would ask.
For six months, nobody thought to diagnose Juan with valley fever.
Then Julie found her husband passed out and slumped over in his chair. It was Father’s Day.
When they got him to San Joaquin Community Hospital (now called Adventist Health Bakersfield), the doctor drew a vial of spinal fluid, diagnosed Juan with coccidioidal meningitis and said he probably wouldn’t make it through the night.
That’s a night Juan’s kids and wife still refer to as “the end.” It’s the night Juan was supposed to die.
He pulled through, but the disease progressed to the point where Diflucan, the standard antifungal used to treat valley fever, would not work.
“The majority of people don’t get it in the spinal column, and unfortunately, we don’t have a cure or medication,” said Claudia Jonah, health officer at the Kern County Department of Public Health Services. “Just a small percentage of patients get something that severe, but they have it for the rest of their lives.”
Juan’s doctor prescribed Voriconazole, a drug that saved Juan’s life but has been robbing him of his health.
Figuring out a drug’s value when it becomes unaffordable
The costs were staggering, both financially and emotionally. Julie and Juan’s insurance initially didn’t cover the full cost of the drugs, and they were paying $900 for Juan’s 800 mg daily dose of Voriconazole. They drained $10,000 they had in a certified deposit and sold ATVs, a boat, furniture and, eventually, their home to make bills.
Juan, unable to return to work, signed up for social security benefits and got on Medi-Cal, the state insurance plan.
“Obama’s my homie,” Juan says. Without the Affordable Care Act, he would not be able to afford his medication, which now costs than less than $100 a month.
The medication keeps valley fever at bay, but Juan now faces a new challenge: skin cancer.

Juan and Julie Solis take their dog Gigi on a walk around their neighborhood.
Juan’s dermatologist warned him to avoid the sun.
That’s tough for a guy who used to coach his three kids’ volleyball, softball and baseball teams. He doesn’t like to project himself as a sick man. At a recent valley fever fundraiser, he leaned back in his chair, ate pizza and laughed and played with his 4-month-old nephew. You wouldn’t know he was sick.
But that’s not always the case, his 15-year-old daughter, Daisy, said.
“Some days, he’s off. When he won’t get out of bed, I think about those days and I wonder if he’ll make it,” Daisy said.
Her family hasn’t had a real conversation about that possibility, though, she said.
When it does come up, Juan tells his kids the same thing his doctor tells him: “as long as you keep taking these pills, you’re good.”
This theory was put to the test last spring. There was a problem with Juan’s social security benefits. It took two months to work out the confusion, and money was getting thin. Juan started splitting his pills in half.
“Maybe it’s dormant?” Juan said he thought at the time.
It took about three weeks of splitting pills before Juan relapsed and was back in an emergency room. That visit cost $27,000.
Julie had heard of West Nile virus, which in 2008 infected two people in Kern County. She had never heard of valley fever, which that year infected more than 1,100 and left six dead — her husband nearly became the seventh.
Why were doctors misdiagnosing valley fever? she wondered. And why hasn’t there been a broad public awareness campaign?
She calls it a “dirty little secret.”
Juan, soft-spoken, is a little more understanding.
“I don’t blame it on the doctors because they didn’t know,” he said of his misdiagnosis.
But Julie knows that if her husband had been diagnosed sooner, he wouldn’t be in the situation he’s in. His daughter, Marisol, tested positive for valley fever shortly after Juan got sick. Her symptoms subsided after being treated for one year with an antifungal drug.
***
Burning off lesions
When the electric needle hit Juan’s skin, it smoldered. A plume of smoke lingered in the air. He shut his eyes and gripped his wife’s hand. It was all Julie could do to keep from crying.
A little orange flame from the needle flickered across Juan’s ear, turning his skin black.
These doctor’s visits, which range in cost from $100 to $150, have become routine, along with visits to the neurologist, infectious disease specialist and general practitioner.
But the dermatologist Juan visited on this particular day — the day before Thanksgiving — is his favorite. David Elbaum burns and scrapes the lesions off Juan’s face and body.
That day, a spot of squamous cell carcinoma that looked like a wart on his ear was bothering him. It kept him from sleeping on his right side. The lesion on his upper cheek bothered Julie because of how close it was to his eye. Elbaum zapped that one with liquid nitrogen.
It’s all a result of the medication, which was never developed for valley fever but has been used off-label for years to treat the disease. Clinical trials indicated just 2 percent of patients would develop photosensitivity, but those trials were conducted in controlled settings. In the real world, experts in Kern County say it could be as high as 30 percent.
Vfend’s side effects have distinguishing features, such as the freckles that develop up and down the arms of patients like Juan, or the chronic ulcer on the lower lip he sees on every valley fever patient who takes the medication. Juan had lip reconstruction a few years ago to get rid of his.
“This is the first drug I’ve ever seen do this. Some drugs cause photosensitivity, but because this is a lifesaving one, we can’t stop it,” Elbaum said. “People on Vfend in Bakersfield are on it for life. This disease is in their brains, their bones.”
As Juan recovered after his procedure, Elbaum answered a question Julie never thought to ask: if there’s a breakthrough in research and an effective medication comes to market, will Juan’s skin cancer subside? Will Julie get her husband back?
Elbaum was direct.
“He’s so far past it,” he said. “If he immediately did get cured, he’s had so much sun damage, it will not go away because of medication.”
Walking out of the office, Julie wiped tears away, still in a state of shock.
“I really thought that if they found a cure, the skin cancer would subside,” she said.
Juan tried to console her. Tried to convince her that it would be better than nothing. They could still make the valley fever go dormant, he told her. They could make it go to sleep. Maybe then, he would have just one disease to battle instead of two.
“It’s just my life now,” Juan said.
***
CLARIFICATION: An earlier version of this story stated that valley fever kills about 95 percent of patients in the first two years. That is true only if valley fever is left untreated. With treatment, the fatality rate drops to 30 percent.
***
SIDEBAR: 3D imaging could answer fundamental questions about valley fever
For more stories in this series, click here.

