After Ebola, are U.S. hospitals prepared for the next deadly threat?
It’s been almost five months since the Ebola virus was first diagnosed in the U.S. While a handful of specialized hospitals worked together to treat patient zero and the nurses who contracted the disease while caring for him, health centers around the country spent thousands of dollars stocking up on protective supplies, providing extra training and sometimes even constructing new hospital units dedicated to exotic or highly infectious diseases.
The threat of an Ebola outbreak in the U.S. was always small and is even smaller now. But are hospitals around the country better off for the preparations they undertook, or will the investment fall to the wayside, forgotten until the next scary disease outbreak?
In an interview about hospital preparedness, Dr. Stuart Cohen, director of Hospital Infection Control at the University of California, Davis Health System, told me that Ebola was just the latest in a long line of strange or alarming diseases like SARS, MERS or H1N1 that have gradually pushed U.S. hospitals toward higher standards of infection control and treatment. From the piece:
People are making infrastructure changes and really getting focused on what’s necessary to manage complicated patients,” said Cohen in a phone interview with The Huffington Post. “I do think there will be [disease outbreaks] after this, so that preparation won’t be a one-time wonder.
But it's just as easy to be skeptical that anything has changed, in part because very little reporting is done after a crisis is over. I want to investigate what changes are actually being made in US hospitals following the Ebola outbreak, and what effects those changes could have on future threats. I hope to dig into the issue with a report on the network of hospitals, designated by the U.S. Department of Health and Human Services as Ebola treatment centers.
I also plan to explore infectious disease preparedness on an individual level. For many serious viruses, this means getting vaccinated -- usually in childhood. Decades ago, parents were desperate for vaccines that would protect their children against dreaded diseases like polio. Now, as the recent measles outbreak and the ongoing reluctance to vaccinate pre-teens against HPV has shown, parents need a lot more convincing. As California communities continue to experience the consequences of vaccination rates, how will this complicate hospital preparedness for highly infectious diseases that many doctors may have never seen in person.
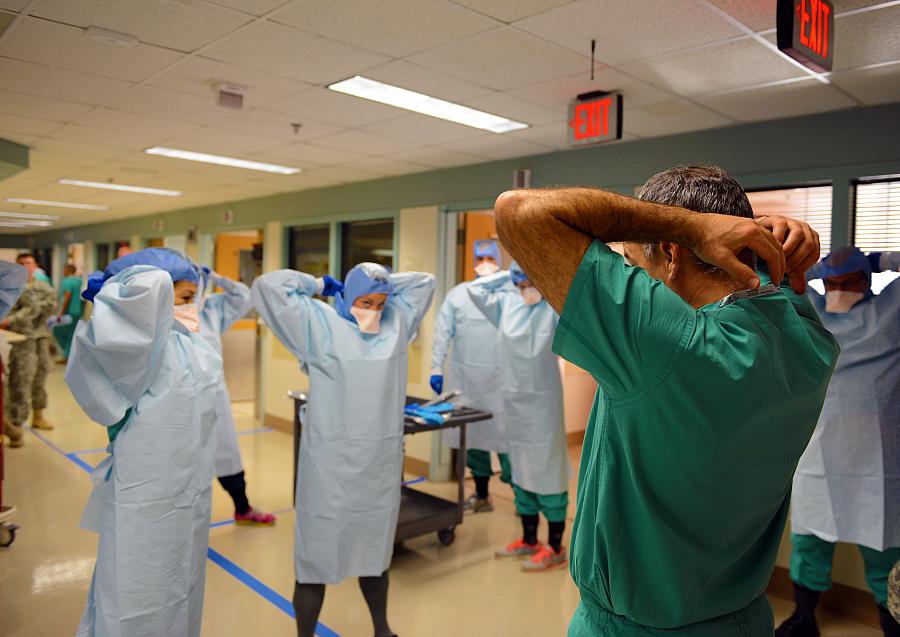
Photo via Flickr: armymedicine

