How ‘surprise bills’ work, and why it’s time to get serious about them
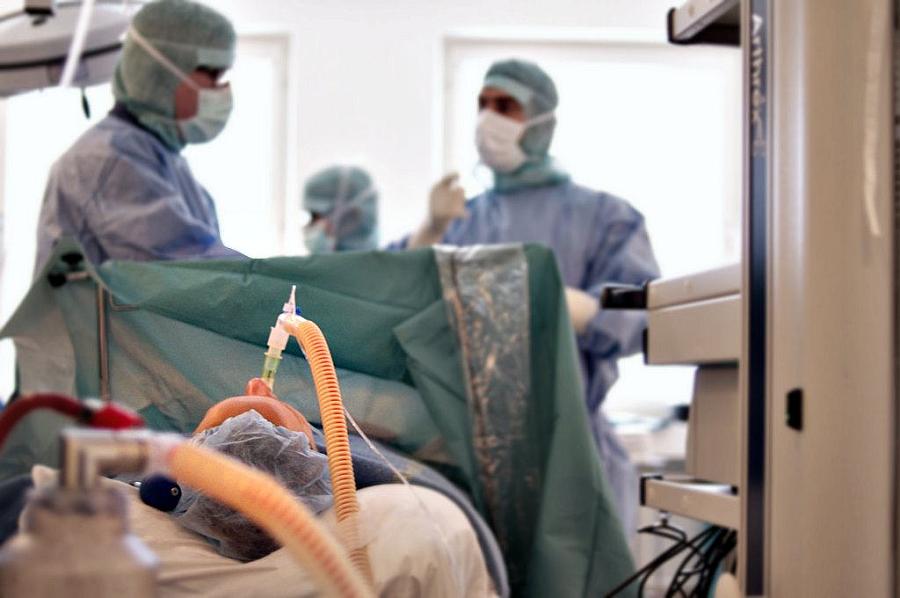
This is not the best time to be wondering about which of these providers isn't in your network.
You have a sharp, stabbing pain in your side. You rush to the emergency room of a hospital and are told you need an appendectomy. You know the hospital is in-network, and so you are confident that any expenses for your treatment will covered — right?
Wrong.
If you’ve gotten a “surprise bill” in the mail for medical expenses you thought were covered by your health plan, you are not alone. According to a recent Consumers Union survey, nearly one in four Californians with private insurance report having received a surprise bill. This can happen with a variety of specialists (surgeons, anesthesiologists, pathologist, radiologists, ER docs) and in a variety of settings, including hospitals, outpatient surgery centers, diagnostic laboratories, imaging centers.
Surprise medical bills occur when people receive an additional bill for the difference between the provider’s charges and what the insurer pays for in-network care. The practice is called “balance billing.” But how, you ask, could I have gotten a balance bill from an in-network hospital?
Here’s how: Although the hospital may be “in-network,” the surgeon and anesthesiologist working there may not be. There is no law requiring doctors to be in-network just because they provide services through an in-network facility. So, the hapless patient (you) is hardly in a position to verify who is “in” and “out” of network while lying on a surgical gurney. Then, after the surgery, you are presented with a bill from both the surgeon and the anesthesiologist for full charges. The “surprise” stems from the fact that you had no reasonable way to determine if the surgeon and anesthesiologist were out-of-network AND that their full charges might be up to 50 times higher than the negotiated rate the insurance company would normally pay for in-network care!
Preferred Provider Organizations or PPOs are structured to provide both in-network and out-of-network coverage, allowing individuals to have a greater choice of doctors and hospitals. It’s reasonable to expect that if someone consciously chooses an out-of-network provider, they should pay more for their care. The issue with surprise bills is, of course, whether individuals seeking urgent or emergency care are able to consciously choose out-of-network providers when they are in clinical distress and when they’ve chosen an in-network facility to seek care.
In contrast to PPO members, HMO members (and PPO members regulated by California’s Department of Managed Health Care) are already protected from surprise bills in two ways. First, if they go out-of-network for non-emergency care, they know they will pay the full bill on their own; that’s an essential feature of HMO coverage. And, if they require emergency care, they are protected from balance billing by state law, which was confirmed by a ruling from the California Supreme Court in 2009. The Court found that Section 1379 of the Knox-Keene Act of 1975 could be interpreted to prevent balance billing by physicians in emergency settings. As a result, HMO members in California, and most other states, do not receive surprise bills for emergency out-of-network services. They are fully protected.
So what can be done? Clearly, market solutions haven’t worked, unless you view price discrimination based on hidden prices a fair outcome of the market. I don’t, so I believe government action, either in the form of legislation or regulation is the only solution. And, because there is no existing law that can end this practice, new legislation is needed. AB 533, authored by Rob Bonta (D-Oakland) and currently before the legislature, would eliminate surprise bills and balance billing for out-of-network physicians providing services at an in-network hospital or facility for non-emergency care. The law would simplify decisions on the part of both PPO and HMO members; once they selected an in-network hospital or other facility (e.g., skilled nursing home, laboratory, outpatient surgery center), all physician services provided during that episode would be paid at least at a rate equal to Medicare reimbursement rates for all non-emergency services.
In an interview last year, I called balance billing for services by out-of-network providers at in-network facilities “… an abuse of the implicit trust that you have with your doctor and with your healthcare providers.” AB 533 would significantly curtail this practice by extending protection to all PPO and HMO members when they select an in-network facility for non-emergency services, by stopping doctors in those facilities, who may never come in personal contact with the member, from sending them a surprise bill. But additional legislation will be needed to prevent surprise bills for PPO members when they receive out-of-network emergency care.
Until then, it’s time for the legislature to take this important first step to protect California consumers from balance billing by passing AB 533. No more surprises — it’s time to do the right thing!
[Photo by Zdenko Zivkovic via Flickr.]

