Black and Hispanic preemies more likely to be born at poorer performing hospitals
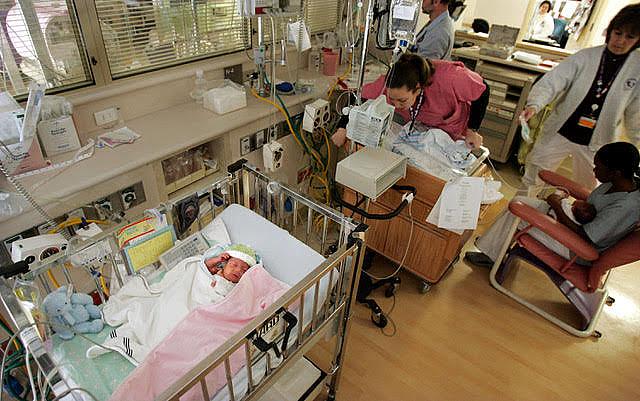
Photo: Mario Tama/Getty Images
Ten years ago, Dr. Elizabeth Howell took on a study to assess how black and white babies born with low birth weight fared across New York City. At the time, she found there were significant differences between the two groups: black babies with very low birth weight were several times more likely to die than white babies.
Howell and her colleagues estimated that, if black women delivered in the same hospitals as white women, then very low birth weight mortality rates for black babies would be reduced by 6.7 deaths per 1,000 for very low birth weight births, removing 34.5 percent of the disparity between the two groups.
But there has been positive change in care for premature babies since then. “There has been a substantial amount of improvement in neonatal care over the last decade,” said Howell, director of the Women's Research Health Institute at the Icahn School of Medicine at Mount Sinai. “In light of a significant focus on quality improvement, we wondered if those findings were still true.”
This time, Howell and her team chose to look at morbidity instead of mortality. Infant mortality is awful, but morbidities such as neurodevelopmental delays impact the entire trajectory of a child’s life. They also adjusted the study to look at very preterm infants, instead of very low birth weight ones — doing so allowed them remove babies who were just small for their gestational age but not premature. In addition, the researchers added Hispanic babies to their study.
They found surprisingly similar results: Where the babies were born mattered greatly. Race didn’t seem to matter in itself, but more black and Hispanic mothers were delivering at hospitals with worse rates of morbidity.
In the study’s sample of 7,177 very preterm infants born at 39 hospitals across New York City, 28 percent of the babies died or experienced serious complications. Compared to white infants, however, black preemies were almost twice as likely to die or have severe health issues, while the odds were about 50 percent higher for Hispanic babies. The research was published in JAMA Pediatrics this month.
Full-term babies gestate for 40 weeks, and those born before 37 weeks are considered preterm. Very preterm — the infants in this study — are born between 24 and 31 weeks. They can have a host of health problems, including breathing issues, vision and cognitive problems.
It’s still a puzzle why a mother would choose or end up at one hospital over another. In 2011, Howell tried to understand such decision-making. She looked at factors like a mother’s proximity to the hospital, and found that distance alone didn’t explain a decision.
“In fact, black women lived slightly closer to higher-performing hospitals,” Howell said. “It’s complex, and involves referral patterns and access.” She adds that Medicaid patients have a limited selection of physicians, and physicians often drive the conversation about where to deliver. “It could be familiarity, it could be someplace that is close to family support.”
And when it comes to hospitals, researchers still don’t know what drives the high amount of variation.
Howell hopes to find answers to both these questions in the future. She is doing qualitative research in hospitals, and also doing focus groups with moms to understand how they end up giving birth at a given hospital.
While this study was focused on New York City, many other studies have shown similar health disparities between hospitals. “From heart attack care to severe complications among moms, we see that black women go to hospitals with worse outcomes,” Howell said. “And if it’s true across the country, it’s going to be true in the NICU.”
Disparities in care at the beginning of life can set a course for a person’s whole existence, since events at the beginning have an outsized influence on the rest of a person’s life. “I think it’s so important to think about these disparities and the impact they have on trajectories,” Howell said.
**

