Understand how life-and-death decisions could be made on front lines of COVID-19
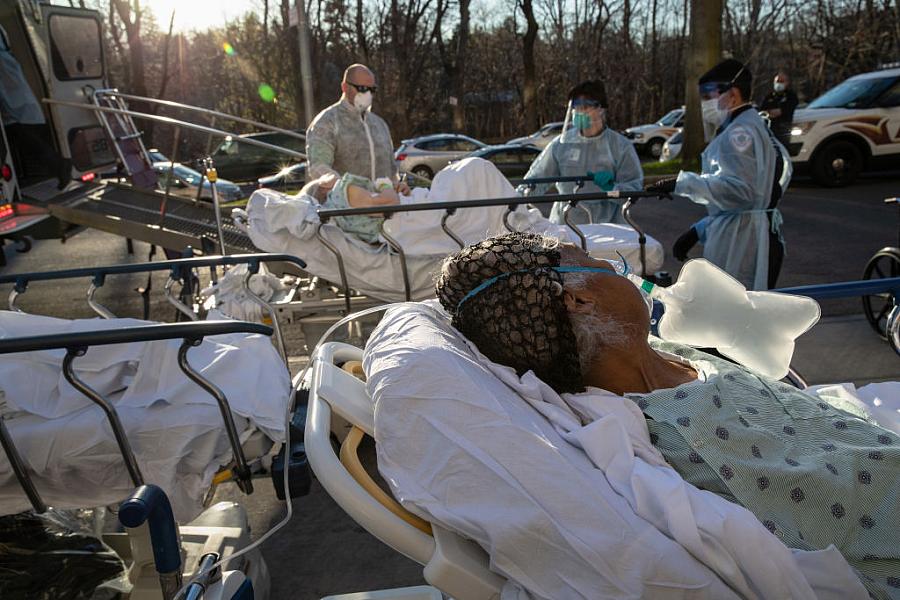
(Photo by John Moore/Getty Images)
As hospitals across the country have made preparations for a surge of COVID-19 patients, they’ve also had to plan for tough decisions on potentially scarce resources like ventilators.
These plans, driven by dire predictions of overstretched hospitals, mark a shift in medicine from an emphasis on each individual patient to those patients most likely to survive their time in the hospital, said Dr. Sunita Puri, the medical director for palliative care at the Keck Medical Center and Norris Cancer Center of USC and a member of Keck Hospital’s Ethics Committee.
“That’s a very, very big shift in the thinking of physicians and in the expectation the public might have of doctors and nurses during the time of shortages,” Puri said this week in a Center for Health Journalism “Covering Coronavirus” webinar. “…It’s uncomfortable for everyone involved.”
Puri described the logic behind these potential decisions, common misconceptions, and story ideas for journalists reporting on resource allocation and shortages.
Taking the decision away from frontline doctors
Even though there’s been a lot of discussion about care rationing and hospital surges, worst-case scenarios of deciding which patients get care haven’t happened in the country to date, Puri said.
Still, health systems are adopting clear policies that would address these dire scenarios, taking the decision making away from the physicians on the front lines and putting them in the hands of a triage officer or committee.
These committees, which are generally made up of people from a variety of disciplines, would look at how sick a patient is when they come in and what diseases they have been living with, Puri said. For example, they might look at whether the patient has diabetes, heart disease, or advanced cancer. (She pointed out that this would apply to all patients needing scarce resources, not just those with COVID-19).
They’d likely look at a patient’s Sequential Organ Failure Assessment (SOFA) score, which can help predict in-hospital survival, and their life expectancy. The decisions would not take into account social status, race or ethnicity. After weighing all the relevant factors, the committee would then assign a priority score.
“That doesn’t mean we say, ‘Sorry, there’s nothing we can do for you,” Puri said. “It means you may not be the highest priority for a ventilator, but we’ll still provide the best care for you.”
Covering the nuances
One of the biggest misconception Puri sees surrounds the use of the urgent measures taken to resuscitate a patient in a life-threatening cardiovascular emergency.
Contrary to popular medical dramas, the percentage of resuscitated people who survive as themselves is much lower than suggested by these shows.
When a COVID-19 patient’s heart stop because of low oxygen, the chances of bringing that patient back is “exceedingly low.” And, to perform resuscitation is very labor and resource intensive, involving a team of health care workers who are risking their own health in the process as virus particles are aerosolized.
If a hospital decides that they will not resuscitate patients with COVID-19, it’s because they want to make sure they protect the staff so they can continue to help as many patients possible, she said. That doesn’t mean they won’t treat patients with COVID using other approaches, she pointed out.
In some ways, the pandemic presents “a strange gift,” she said. People of all ages are forced to think about what they’d want for themselves if they got really sick.
Some questions everyone should consider include: What is the story of my life? What activities define my life and give it meaning? How much suffering would I be willing to go through? Who would I want to speak on my behalf if I couldn’t advocate for myself? Who would I not want to speak for me?
These conversations — ideally with a health care provider who knows you — can also address the fears of some people with disabilities who might worry they would be a low priority for scarce resources. It’s important to document the quality of one’s life at baseline.
Questions for journalists
Journalists interested in assessing the readiness of their local hospital should ask how many COVID-19 patients they’ve had, and how many needed to be in the intensive care units (ICUs). Has the hospital encountered any obstacles in their care, and, if so, what have they done? What are the day-to-day challenges? How many days are COVID-19 patients staying on a ventilator and how does that compare with broader patterns in the region?
Ask about the hospital’s response plan if resources do become scarce. What sorts of discussions have they had with other hospitals in the area that might be able to absorb patients if necessary? Does your local hospital feel prepared? Are care protocols coming from the government or the hospital system?
What are current supplies or personal protective equipment (PPE) like? Is there a plan in place to get more as numbers go up? Is this a concern?
If there’s not enough PPE, medical providers are more likely to get sick, leading to a shortage of doctors and nurses equip to take care of critically-ill patients.
Asked what types of stories we need more of right now, Puri said she’d also like to see more portraits of the people who have died of COVID-19, including front line health care workers. It would also be smart to look at hospital finances and how hospitals and clinics might rethink models to stay afloat financially during this crisis.
It’s also a good opportunity to look at health disparities that have made COVID-19 especially perilous for some minorities .
“It’s always in these situations where inequalities become exacerbated,” she said. “This is an opportunity to rethink the vast disparities we have in this country around health care and wellbeing.”
Puri stressed the need for nuanced storytelling about the life-and-death decisions this virus is forcing upon patients and doctors right now:
“Triage decisions are not about giving you everything or giving you nothing … it’s about using our resources to help the greatest number of people live, but to continue to treat with the best possible care everyone who is walking through the door,” she said. “That’s what I think is a little bit missing in the coverage now.”
**
Watch the full presentation here:

