How are homebound residents getting vaccinated in your coverage area?
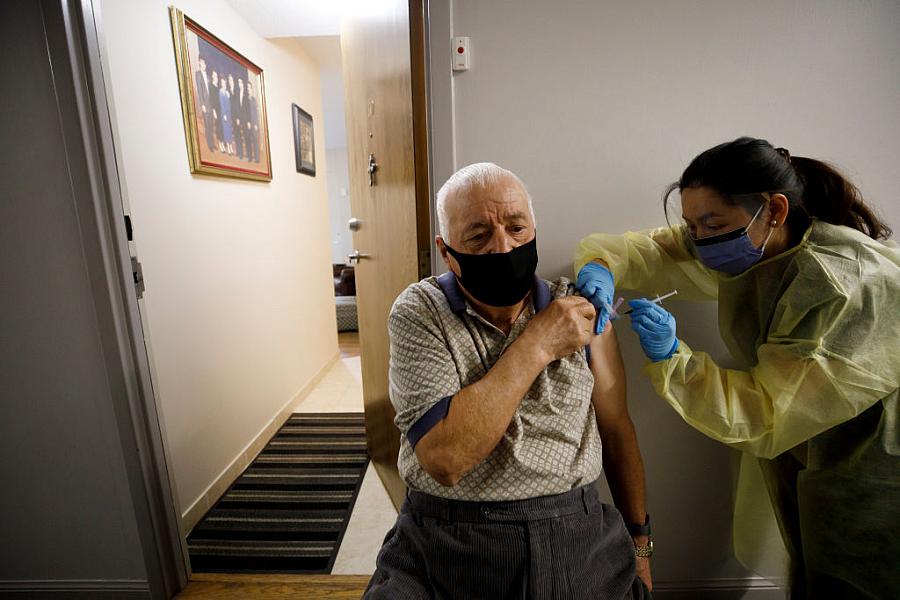
(Photo by Cole Burston/Getty Images)
As part of its “You Asked, We Answered” series, the Center for Health Journalism has been asking journalists what questions they have about reporting on COVID-19. This week's question: “How will the vaccine be distributed to homebound? I’ve asked all local officials and they have no answers.”
Early in the pandemic, veteran health reporter Judith Graham noticed the lack of attention being paid to homebound Americans. There wasn’t much data on how hard they were being hit by COVID-19, or what types of services they got if they contracted the virus.
So when vaccine distribution began late last year, she wondered how the shots would be delivered to the millions of people in this country who are homebound. On Twitter, family members of these individuals were asking the same questions.
“It’s one thing to say, ‘Everybody should get the vaccine,’” said Graham, who writes a column on aging for Kaiser Health News. “It’s another one to think about, realistically, how are we going to get vaccines to older adults who are cognitively impaired, physically impaired, living at home, don’t have internet access, etc. and so forth?’”
She quickly realized there wasn’t a coordinated plan — but rather a patchwork of local efforts — to immunizing this population against the coronavirus. As she reported, communities’ strategies have included sending geriatricians, visiting nurses or fire department paramedics into people’s homes to vaccinate them.
“This was an overlooked population until very recently, and a lot of places still don’t have plans to reach them,” she said. Still, she added, “I expect these efforts are going to accelerate in many places.”
As the United States races to get residents immunized to quell the pandemic ahead of rapidly spreading variants, states and localities have been left to come up with their own vaccine priority groups and distribution methods. In the process, some people, like the homebound, have been neglected.
Journalists covering this story have had to contend with issues like a lack of data and explicit plans from government officials.
“Honestly that’s been a big source of frustration for me,” said Cindy Krischer Goodman, health reporter for the South Florida Sun Sentinel. “Homebound seniors write to me, and I haven’t been able to find clear answers for them. There is no statewide registration or distribution system.”
One way to protect homebound people from COVID-19 is to vaccinate their caretakers, said Dr. Eric Toner, a senior scholar with the Johns Hopkins University Center for Health Security.
Some of these caretakers are family members and thus not classified as frontline health care workers. States should prioritize them for the vaccine, Toner said. Another solution: mobile vans set up in communities for homebound Americans who can leave their homes.
Going into people’s residences one by one to vaccinate them will be a slow and logistically challenging process, Toner noted. The Pfizer and Moderna vaccines, which have been the most widely available so far, have cold storage requirements and only last for a few hours after being thawed.
The Johnson & Johnson (now resuming) and AstraZeneca (pending approval) immunizations don’t have the same temperature restrictions and would be easier to get to homebound people, Toner said. Some localities have been using the Johnson & Johnson vaccine for those stuck at home because it is only one shot, compared to two injections for Pfizer and Moderna.
“Now places are beginning to think about how they want to do this — in part in response to outcries from the families of people who are homebound,” Toner said. “That’s driving state and local health departments to figure it out.
“It’s important. It’s a hard thing to do. But these are people who are especially vulnerable should they get infected.”
As Graham has reported, many homebound individuals have multiple medical conditions — such as heart disease, cancer and lung disease — that leave them particularly susceptible to COVID-19.
She suggests journalists pursue this story by checking with local visiting nurses and home health care agencies to see if they’re vaccinating people who can’t leave their residences. There is no national advocacy organization specifically dedicated to homebound Americans, she noted.
Beyond that, local fire departments, area agencies on aging, medical societies or hospitals might have answers or be working on solutions for the issue, she said.
There has been progress since Graham wrote her initial story in February. For instance, New York City recently started a program where the fire department deploys nurses to vaccinate homebound residents with the Johnson & Johnson shot.
“There’s more attention being paid to this group, and there are new efforts springing up every day,” Graham said, adding: “It’s still highly fragmented and not sufficiently broad in scope.”
The splintered nature of these undertakings — and quickly evolving distribution strategies — means there are a lot of local and regional stories waiting to be told right now.
**

