How COVID-19 prevention and treatment get lost in translation
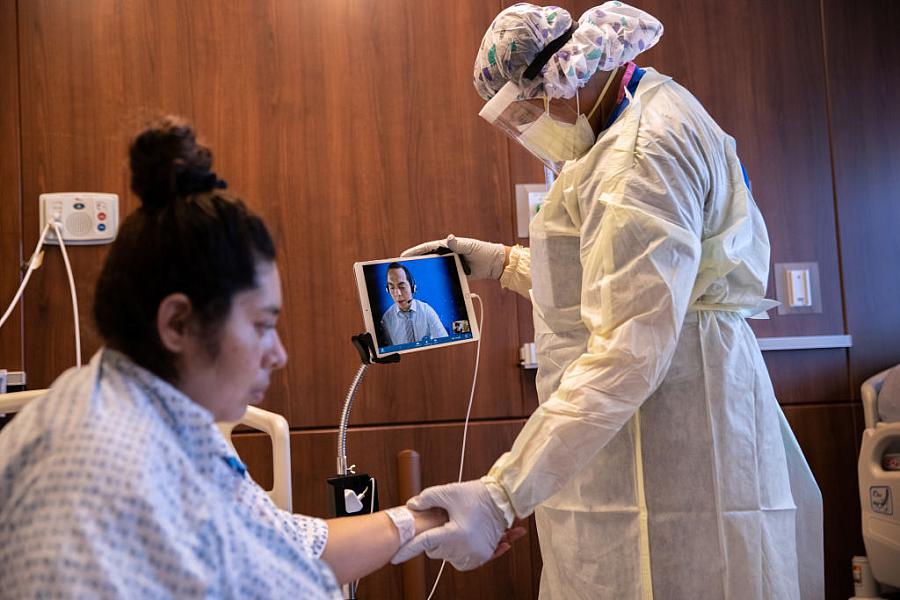
A hospital worker speaks through a remote Spanish translator while preparing a COVID-19 patient take her first steps after being removed from a ventilator at a hospital in Stamford, Connecticut.
(Photo by John Moore/Getty Images)
It should be obvious that effective health communication is essential to control the coronavirus. Everyone needs to know how to stay safe and protect others, when to get tested, and where to seek treatment if COVID-19 symptoms develop. But language barriers pose a significant problem for millions of people in this country who speak limited or no English.
While most hospitals and clinics are required by law to facilitate communication in the languages of all patients, translation and interpreter services are inconsistent at best, and too often nonexistent even in matters of life and death.
Soon after the coronavirus struck, advocacy organizations in my state, including the Washington State Coalition for Language Access, where I lead health work, and Latinos Promoting Good Health heard from people seeking advice on how to deal with language barriers to COVID-19 education, prevention and care. For example, in counties with many Spanish-speaking residents, hospitals and municipalities initially promoted free screening and testing programs in English only, and had no interpreters at test sites.
In western Washington, unbeknown to the family of a man hospitalized for COVID-19 who spoke only Spanish, doctors made plans to take him off a ventilator. When the man’s bilingual son finally learned what was happening, he got help from a disability rights group and requested a new treatment plan for his father, who survived.
And after several patients of indigenous heritage died of COVID-19 in an area hospital, cremation plans were made without bringing in interpreters who could speak Mixtec languages and consult with the families. This was especially troubling because cremation is contrary to their cultural practices. The families were hesitant to speak up due to their immigration status.
Some 65 million people in the United States — one in five — report speaking a language other than English at home, including 26 million people who say they have limited ability to speak English. These numbers, drawn from U.S. Census data, are widely considered to underestimate language challenges because the census notoriously undercounts immigrants and asks only about the ability to speak English, just one skill needed for communication in health care.
The official definition of limited English proficiency (LEP ) — limited ability to read, speak, write or understand English — better encompasses the skills needed for good communication about prevention and treatment. Even without language barriers, people with LEP face the pandemic at a disadvantage. They have higher rates of chronic illnesses and other risk factors, and they are much less likely be insured or have a regular source of care.
In Washington, where the nation’s first COVID-19 case was documented, an ominous pattern of disparities soon emerged. After the initial outbreak among predominantly white, elderly residents of a Seattle-area nursing home, cases increased among younger people of color. The University of Washington Medical Center, a system that provides language assistance to patients, found higher infection rates among LEP patients. Speakers of Spanish, Amharic and Khmer had infection rates roughly five times higher than English-only speakers.
Language access requirements and realities
Under federal law, recipients of federal funds — which includes virtually all hospitals and clinics — are required to provide meaningful language access to current and prospective patients and their families. These obligations are grounded in Title VI of the Civil Rights Act of 1964, which prohibits discrimination on the basis of race, color or national origin. The Affordable Care Act (ACA) strengthened language access requirements.
In June, as the pandemic was tearing through the country, the Trump administration finalized a rule that significantly weakened ACA language access provisions. Only a month earlier, the Department of Health and Human Services Office of Civil Rights issued a bulletin on “ensuring the rights of person with limited English proficiency in health care during COVID-19.” These seemingly contradictory orders have caused confusion, but Title VI obligations still stand. State nondiscrimination laws and hospital accreditation standards also require language access at health care facilities.
Yet language assistance in health care remains uneven across the country. A study in Health Affairs found that about one-fourth of hospitals in areas with high or moderate need for services such as interpretation, translation and multi-language signage do not offer them — nor do more than one-third of hospitals in areas with lower needs. While proper diagnosis and treatment depend on communication, language services are often portrayed as an add-on, not part of regular care, and referred to as an “unfunded mandate.” A partial stop-gap measure, the Coronavirus Language Access Act, was introduced in Congress in August.
Medicaid offers reimbursement for interpreter services, but a 2017 analysis found that only 15 states used it. Medicare doesn’t pay for these services, nor do most private insurers. These refusals defy fiscal logic.
Language barriers are associated with prolonged hospitals stays, serious medical mishaps, medication errors, and other disasters that are costly for patients, health care providers and insurers. Malpractice settlements show it can be far more expensive for hospitals not to provide adequate language services, especially when this failure results in catastrophic patient outcomes.
My state was hardly the only place where the pandemic magnified longstanding language problems. Often, translated health care information has been machine-generated, which has been shown to be not reliable. Across the country, information about COVID-19 was initially scarce and offered only in Spanish or a few other languages, despite the diversity of local populations. Many translations were web-based only, but the people who needed them didn’t necessarily have computers, smartphones or internet service.
Phone hotlines often had messages only in English or did not explain how to request interpreter services. Many programs seemed to be designed on assumptions that users would have the time and privacy to call during the workday and be able to stay on hold during lengthy waits. While English speakers could sometimes request call-backs, this option was rarely offered in other languages.
Translated information about COVID-19 and protective measures has become more widely available in many languages in recent months. But new problems have arisen.
Virtual care has become an essential part of medicine, but telehealth services often don’t have language access interfaces. And it can be almost impossible for people with limited English to get help for basic needs that have become so dire during the pandemic, such as food, housing, income assistance, unemployment benefits, child care, schooling and mental health.
Urgent stories abound
Reporting and analyses by journalists can call attention to very real harms caused by language barriers and help promote needed changes at the community level, where most care is delivered, and in state and federal policies.
There are powerful stories in the experiences of patients, families, and health workers; in data about language needs and services; and in the challenges of unearthing such data. In addition to hospitals, community clinics and public health departments, reporters should reach out to health and health care advocacy groups, immigrant organizations, and language services associations.
Journalists can also look at policies in the few states that have taken notable steps. Massachusetts requires and monitors competent interpreter services at hospitals. California requires coverage of interpreter services by commercial insurers. Some states have equity offices within their health agencies, and Hawaii and New York have created state-level language access programs with cross-agency coordination.
This kind of pandemic reporting can help spur the action so urgently needed to ensure that high-quality language services become a routine part of health care and a lifesaving strategy in the fight against COVID-19.
Joana Ramos is a health policy consultant and a founding member of the Washington State Coalition for Language Access.

