How a surgeon helped solve the problem of far too few black organ donors
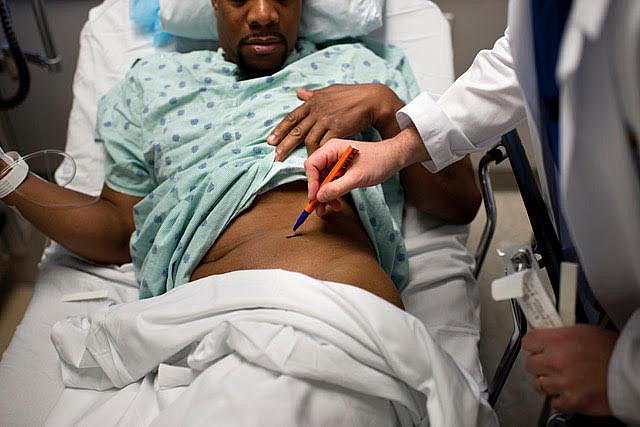
Doctors at Johns Hopkins prepare to transplant a kidney from a living donor into a recipient. (Photo: Brendan Smialowski/AFP/GettyImages)
It was 1978 when Howard University professor and transplant surgeon Clive Callender got a call from the South-Eastern Organ Procurement Foundation, saying they had some data to share. What happened since then is a testament to the power of community outreach to diminish health disparities.
The foundation was the nation’s oldest organ procurement organization, and a predecessor of the United Network for Organ Sharing (UNOS), which coordinates donations across the country today. Howard University Hospital is the nation’s only teaching hospital on the campus of a historically black university.
“Their data demonstrated that 70 percent of the patients on dialysis were black, and yet less than 10 percent of those who donated for transplantation were black,” Callender recalled recently. “They recognized the discordant nature of the data and wondered what could be done about it.”
Callender didn’t have an answer to the problem of too few black donors, but he obtained a $500 federal grant to do some research. Working with a colleague, they brought together 40 individuals from Washington, D.C.’s African-American community for two-hour sessions to talk about organ donation. Initially, only two participants said they’d be willing to sign an organ donation card.
Though organs can be transplanted between races, donors and recipients must have some genetic similarities. Some blood and tissue types are more prevalent among specific ethnicities than others. To make sure matches can be found for everyone, it’s essential that all be present in the donor pool, in numbers proportionate to their representation in the population, Callender said.
Through in-depth conversations, Callender and his partner identified five barriers to organ donation. First, participants were unaware of the great need for organ donation within their own community. And many feared that organ donation would go against their religious beliefs.
There was also a deep distrust of health care providers, rooted in awareness of the 1932 Tuskegee Syphilis Experiment, in which 600 black men from Alabama went untreated for the disease just so they could be studied.
They worried too that if they signed an organ donation card hospitals would allow them to die so their organs could be harvested. And they were convinced doctors only wanted their organs so they could be transplanted into white people.
Knowledge in hand, the researchers sought to address these concerns through education. They shared that a disproportionate number of African-Americans need transplants due to high rates diabetes and hypertension in the black community. And that organ donation is supported by major religions.
Callender and his colleague stressed that more African-Americans hold positions of authority in health care than in the days of Tuskegee. And that hospitals broach the subject of organ donation with family members only after a potential donor has died. They also noted that at Howard University Hospital, where most of the patients are African-Americans, a majority of organ donors are white.
“What was remarkable was that after we discussed this, all 40 who participated signed onto organ donation,” Callender said. “This said to us that the way to overcome this disparity it to go to these communities and educate and empower them.”
Callender crafted a program to increase minority organ donation in Washington, D.C., using what they’d learned in the focus groups. They honed messages specific to the community, and recruited black transplant recipients and people on waiting lists as spokespeople. The percentage of potential donors among black D.C. residents increased from 10 percent in 1978 to 51 percent by 1993.
In the mid-1980s, Dow Chemical provided funding to roll out similar programs in 22 American cities with the highest African-American populations.
In 1991, Callender published his results in the New England Journal of Medicine, and founded the Minority Organ Tissue Transplant Education Program (MOTTEP). And he expanded its mission to include all ethnic and racial minorities.
MOTTEP initiatives are currently underway in about 25 American cities. In Detroit, MOTTEP Director Remonia Chapman, with help from Gift of Life Michigan, has developed a network of volunteers, block clubs, neighborhood groups and churches, increasing minority organ donation pool from 10 percent to 25 percent over two decades. She was recently named “Michiganian of the Year” by The Detroit News in recognition of her efforts.
Nationally, the organ donation rate of African-Americans surpassed that of whites in 2010. In 2017, there were 38.1 organ donors per million African-Americans, compared with 34.29 per million Caucasians.
But disparities persist.
Of 114,600 people waiting for organ transplants as of April 2018, 30 percent were African-Americans, though the group represents just 13 percent of the American population.
Despite the increase in donors, blacks still are disproportionately represented on organ transplant lists due to high rates of diabetes and hypertension, which can lead to organ failure. Social determinants of health, such as poverty and institutional racism, are believed to contribute to the disparity, but genetics are also a factor, Callender said.
For example, African-Americans are genetically predisposed to focal segmental glomerulosclerosis (FSGS), a common cause of nephrotic syndrome in pediatric and adult patients. Most children with FSGS don’t respond to therapy and progress to end-stage renal disease.
And the heterogeneity of African Americans, or mix of races in their ancestry, can make it more difficult to find a suitable donor — especially in the case of bone marrow transplants, which require a near-perfect genetic match.
More donations are needed from every race, Callender added. Hispanics, the nation’s largest minority, had a donation rate of 27.5 per million in 2017. And just 15.1 per million Asian-Americans are organ donors.
“It doesn’t matter if people are black, white, green or purple — we need donors from all ethnic groups.”

