Maine has been hit hard by the opioid epidemic. What does that mean for its children?
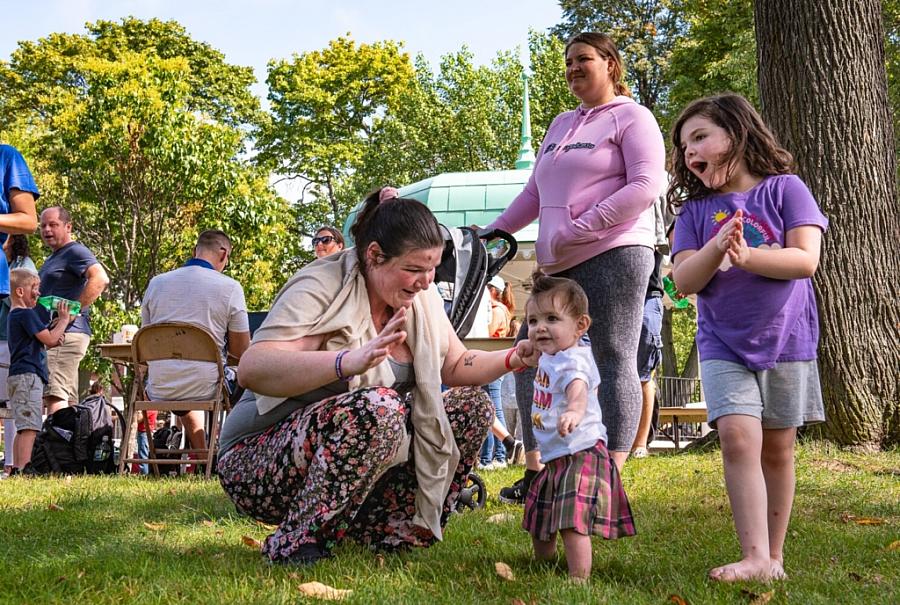
Kirsten Gaddas holds her daughter Oakley Shuman's hand as her other daughter, Sophia Shuman, right, dances to the music at a Rally for Recovery in Kennedy Park in Lewiston, Maine in September. The former drug user, who has been clean for nearly three years, says she owes her success to family, friends and the network of support groups for substance use disorder in the area.
The pandemic is a troubling reminder that the opioid crisis is far from over in Maine. Drug-related deaths rose by 33% in 2020, from 380 deaths in 2019 to 504 in 2020, and exceeded a previous record high set in 2017.
Nearly 85%, or 417 deaths in 2020, were caused by opioids, according to the Maine Office of the Attorney General’s annual “Maine Drug Death Report.” This year alone, there have been 399 fatal overdoses as of August 31, according to the OAG.
But as some state-led initiatives such as the Prescription Drug Monitoring Program, which tracks the prescribing and dispensing of controlled substances from physicians, veterinarians and pharmacies in Maine, have curbed the opiate doctor-to-patient pipeline over the past five years, illicit and nonprescription drugs have taken hold.
“The rise over 2019 was largely driven by a 33% rise in deaths due to the nonpharmaceutical drugs, primarily fentanyl, increasingly combined with the methamphetamine or cocaine,” wrote the drug report’s author, Dr. Marcella Sorg, a medical and forensic anthropologist from the University of Maine’s Margaret Chase Smith Policy Center.
Recovery advocates are also raising the alarm. At a panel discussion last month hosted by the Lewiston (Maine) Public Library, Jeremy Hiltz, a licensed alcohol and drug counselor and founder of Recovery Connections of Maine, warned that “we have a large problem coming up with methamphetamine.”
“It’s all over our community, it’s a cheaper option sometimes, it’s easy to struggle with,” Hiltz said, who is in long-term recovery himself.
The pervasiveness and severity of the opioid crisis are not measured solely in overdose deaths, however. Poverty levels, educational outcomes and child and family well-being, to mention just a few examples, are measures of both the causes and effects of substance use disorder.
Meanwhile, Maine’s child welfare system is still recovering from funding cuts under former Gov. Paul LePage and the challenges brought on by the pandemic. The Maine Department of Health and Human Services’ Office of Child and Family Services (OCFS) is chronically underfunded and understaffed.
Over the summer, Maine DHHS contracted a national firm to review OCFS practices after four children under the age of 4 died over the span of less than a month. Two were beaten or shaken to death. One died after accidentally ingesting fentanyl. The fourth appears to have died from a self-inflicted gunshot wound. The parents of three of the children have been charged in the death of their child. It appears at least one of the families had prior involvement with OCFS.
The Legislature also directed the Office of Program Evaluation and Government Accountability (OPEGA) to investigate OCFS, the third time in four years that that the OPEGA will look into children’s welfare.
This is not the first time the system has faced scrutiny. A series of high-profile child deaths in 2017 and 2018 led to some policy changes and additional funding to the OCFS. But federal data show that although the number of caseworkers increased in 2019, so did the number of reports of neglect or abuse. In 2019, the workload per caseworker remained about the same as in 2017.
What happens when these dual crises collide, and what’s needed to solve these issues? Is there a connection between the introduction and distribution of opioids into a community and indices of child well-being? Is Maine’s child welfare system equipped to effectively support families and children where substance use disorder is a risk factor? What solutions are out there?
These questions will guide my project, which will focus on these issues in Androscoggin, Franklin and Oxford counties, for the 2021 Data Fellowship. Major flashpoints such as fatal overdoses or child deaths often receive the most attention from both the media and policymakers. And it makes sense — they are clear indications something has gone wrong.
But many stories remain to be told. There are troves of data from the Maine Drug Data Hub, and as the investigations into OCFS continue, DHHS has already begun publishing data on child welfare outcomes. The data from these sources and others will guide my reporting and tell me where to look next to form a deeper, fuller picture. I anticipate closing my project by exploring policy solutions and other initiatives from within the state of Maine or models from other states.
My reporting will be guided by the data, but these stories would not be complete without the human voices of those impacted by these crises and those working toward solutions. I will seek out the voices of doctors, educators, families, state and local leaders, recovery coaches and people in recovery, caseworkers, and other experts to examine how the evolving opioid crisis has impacted family and child well-being, and what’s being done to tackle these complex issues.

