Silicon Valley is riddled with inequality. What does that mean for health?
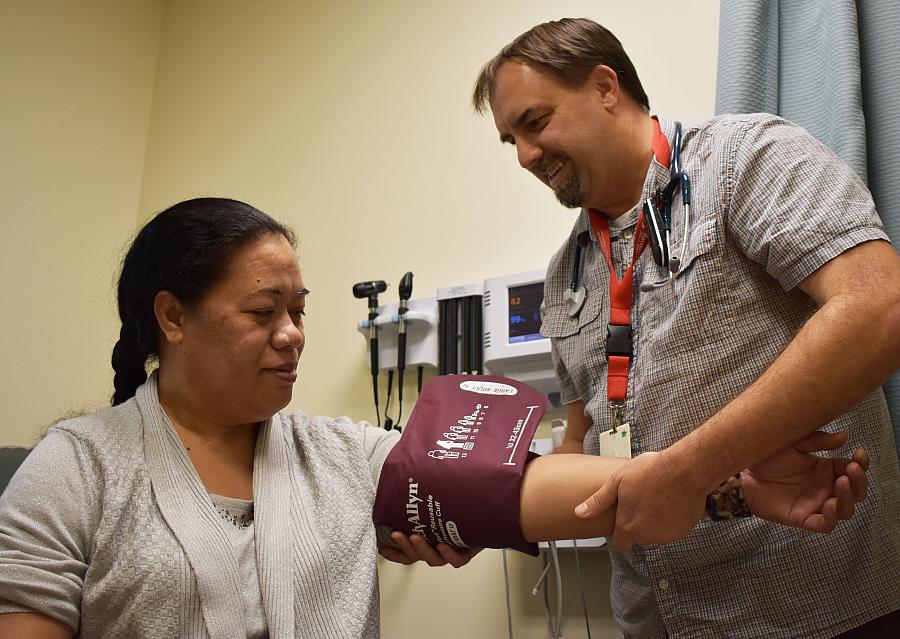
A patient at the Ravenswood Family Health Center in East Palo Alto has her blood pressure checked.
(Photo via The Almanac)
Picture Palo Alto, Atherton and Menlo Park — three of the nation's most expensive suburban towns, where school districts rank among the highest in the state, an extraordinary number of people drive Teslas, residents are predominantly Asian and Caucasian, and many residents gulp yet somehow manage to pay the median home price of several million dollars.
But go to areas that border these jurisdictions and a different, less idyllic picture emerges. East Palo Alto, North Fair Oaks (an unincorporated area of San Mateo County bordering Atherton), and Belle Haven (an isolated neighborhood of Menlo Park adjacent to East Palo Alto), have schools striving and failing to retain teachers and families, streets choked with commuters cutting through to tech jobs, and large numbers of families who struggle to pay rent. Residents are often forced to move into close quarters with extended family or live out of RVs or cars to make ends meet. The demographics of these areas are also different, due in part to a history of discriminatory housing practices. East Palo Alto and Belle Haven have larger African-American populations, and with North Fair Oaks, larger Hispanic populations, than elsewhere in southern San Mateo County.
There are substantial differences in life expectancy across these areas. In Belle Haven, the life expectancy is more than five years lower than the San Mateo County average, and in East Palo Alto and North Fair Oaks it is about four years lower, according to the United States Small-Area Life Expectancy Project.
Why is that? For my 2019 California Fellowship project, I aim to find out by sifting through public health data, conducting extensive outreach to community members, including in Spanish, talking to physicians and health experts, and drawing on my sources and the community knowledge I've gained over the last three years as a political reporter covering this area.
I have a few ideas about some of the factors that might shape these disparate life expectancy outcomes.
One is that the cost of living in the area is comparatively exorbitant, primarily due to housing costs. For households working at or even above minimum wage, the cost of housing leaves little left over to pay for health care and nutritious food. According to a recent report from the San Mateo County Office of Education, in the Ravenswood City School District, which serves East Palo Alto and Belle Haven, 58 percent of children experience housing insecurity or homelessness.
One town over, Atherton, with a median home value of $6.6 million or so, routinely wins superlatives as the “most expensive zip code in the U.S.” And while the lower-income neighborhoods I've discussed are considered more affordable, costs have risen dramatically over the last several years. According to the real estate site Trulia, median rent in Belle Haven is $3,700 a month, while the median home is $1.05 million as of January 2019. East Palo Alto is a city that has rent control, so some households may be less burdened by housing costs.
I'm also curious about how land use policy has shaped health in these areas by providing more affluent people proximity to benefits such as nearby grocery stores and parks, and leaving lower-income people closer to highways and the exhaust and particulate matter they bring. I also want to learn more about some relatively new research that suggests that simply living in an area with wealth inequality impacts health outcomes.
In addition, I plan to keep an eye out for innovative initiatives that can improve public health in these communities.
For instance, the Ravenswood Family Health Center has a partnership with the Primary School, a private school for low-income local children run by Dr. Priscilla Chan, spouse of Facebook CEO Mark Zuckerberg, to securely share student data between the health center and school, which has enabled early interventions for health problems like asthma. Another example: Over the past year or so, San Mateo County developed a coordinated entry system to provide more comprehensive support to people experiencing homelessness. Providers such as outreach staff at the local homelessness nonprofit LifeMoves, health care providers and law enforcement officers have begun to coordinate their approaches to meeting the needs of people experiencing homelessness in the county.
Guiding my reporting will be questions I'll collect from the community as I conduct interviews. I hope the stories that result will be a useful resource for my readers.

