
R. Jan Gurley
Physician-writer

Physician-writer
Dr. Jan Gurley, a board-certified internist physician, is the only Harvard Medical School graduate, ever, to have been awarded the coveted Shoney’s Ten-Step Pin for documented excellence in waitressing. Her health/science background covers the vast territory from sub-cell systems, to human studies, to the captivating science of seeing patients one-on-one. Her training includes basic science research (graduating magna cum laude from Harvard), then a residency at UCSF in Internal Medicine, as well as a Robert Wood Johnson Fellowship (Stanford/UCSF Joint Program) in epidemiology, public health and public policy, followed by work as an administrator of large divisions of the San Francisco DPH where she currently sees patients in a clinic for the homeless. Doc Gurley’s health writing has appeared in Salon, The San Francisco Chronicle, and the Chronicle Sunday magazine, along with regular pieces in BlogHer, KevinMD and as one of SFGate's City Brights. Jezebel has called her "indispensible." Her research has appeared in academic publications including the New England Journal of Medicine. You can read more about her at www.docgurley.com.

Reporters should be asking tough and urgent questions of the latest move to let GPT-4 into patients' electronic medical records.
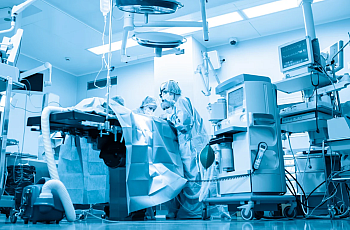
As we look to understand the public health response to COVID-19, Dr. Jan Gurley of the San Francisco Department of Public Health explains what it means when a state institutes Crisis Standards of Care, as Arizona has.

The U.S. faces an impending doctor shortage because not enough new ones are being trained to meet the needs of the U.S. population and a large portion of doctors are reaching retirement age. Will impending changes within the medical industry further exacerbate the problem?

The idea is that Electronic Health Records will reduce paperwork and administrative costs. But as more providers jump onboard, the negative impacts seem to be growing.
The data on the much-lauded Patient Centered Medical Home approach, a cornerstone of ACA, shows that it is expensive, onerously bureaucratic, a drain on health care resources, especially for primary care providers, and a distraction from health care delivery.
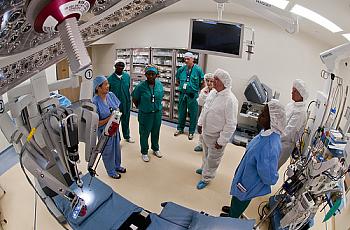
Underwhelming results demonstrate that after all the money and effort invested in bureaucracy, Patient Centered Medical Homes do not contribute to actual patient care.
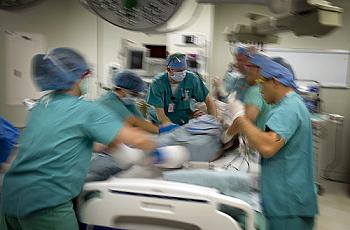
Patient-Centered Primary Care Medical Homes have been around for decades. The more you know about the intention behind them, the more you wonder, "How could that not be a good idea?" Based on the research, cost of implementation and effect on patient care, the answer I found may surprise you.

Hollywood stars, like Glee’s Cory Monteith, aren’t the only Americans struggling with addiction that kills. Monteith, who died of a heroin and alcohol overdose earlier this month, exemplifies the public health tragedy that is opioid overdose deaths in America.
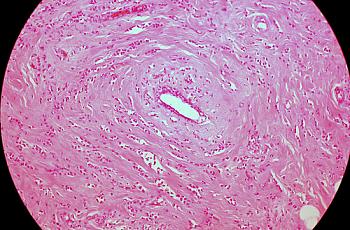
Although I believe we start with data and move forward, it is our narratives and our insights that guide us. Still, for me, this was ultimately a numbers game in the end: three tumors, two breasts, one very difficult decision.

There is nothing so horrifying as when your doctor is too nice to you. I knew I had cancer before they even told me because of the hushed voices, the pats on my shoulder, and the way, suddenly, no one cared how much time was being spent on my visit.