When pregnancy collides with a pandemic

The couple opted for a drive-thru baby shower in November to safely celebrate amid the pandemic.
(Photo by Anjel Alcaraz)
My husband and I always dreamed of having children. Last April I was thrilled to find out I was pregnant. But my excitement quickly turned into worry and sadness when I scheduled my first doctor appointment and was told my husband couldn’t come with me because of strict COVID-19 precautions. It was the beginning of the long, strange trip of pregnancy during the pandemic.
My husband joined that first appointment through a video call. He saw the first ultrasound, at about six weeks of gestation, on his mobile phone. He would not be allowed to accompany me to a single doctor appointment during my whole pregnancy.
I had been working remotely since California's stay-at-home order was issued in March. When I became pregnant, I was grateful to work at home and avoid direct contact with people who may be infected. But my hopes and plans for my pregnancy did not include a lockdown. I was ready to attend classes for pregnant women and first-time parents. I wanted to celebrate the good news with my family and friends. I was hoping to host a beautiful baby shower for our firstborn.
But the world around me became deadlier day by day, and the health care system became more chaotic. Los Angeles County, where I live, reported its first case of the coronavirus on March 9. By the end of May, the Department of Health had logged more than 46,000 cases of COVID-19 and 2,000 deaths. Hospitalizations were rising at an alarming rate. In the turmoil, my HMO’s systems and practices seemed to fall apart.
I was never assigned to a regular obstetric team, but sent from doctor to doctor in two different facilities. Once, I went to an appointment only to discover that the site had been turned into a coronavirus testing center. I was sent to a location eight miles away.
I tried not to let the growing crisis get to me, but it was impossible. I’m a reporter and I wrote about skyrocketing infections, deaths, job losses, closed businesses, evictions and the struggles of low-income students forced to learn online.
I interviewed people by phone, Zoom and email, and completely avoided close contact. It was good for my safety but increasingly bad for my emotional and mental health. I started to feel isolated, then anxious.
My husband and I got together with nobody except our mothers.
Our outings were walks in a park or along the beach, early in the morning or late in the evening to avoid crowds.
When I felt most desperate, I forced my mind to focus on my baby. That kept me strong and reminded me to stay the course to remain healthy.
A scary surprise
In my sixth month of pregnancy, I developed a rash and extremely itchy fingers and toes. I soaked my feet in oatmeal water and applied anti-itch lotions, but nothing helped for long.
Since I didn’t know who my designated obstetrician was supposed to be, I contacted one of the doctors on the list that appeared in my message options in my HMO’s patient portal. She ordered blood tests. I was diagnosed with gestational diabetes (GD). I had no idea what was that, but it sounded bad.
In GD, the blood-glucose level of a woman with no previous history of diabetes stays high — known as hyperglycemia — because she is unable to make and use all the insulin needed to support the demands of the pregnancy, as the American Diabetes Association explains. It usually shows up from 24 to 28 weeks of pregnancy and happens in about 18% of pregnant women.
The condition is treatable with a balanced diet low on carbohydrates and sugars, moderate exercise and the monitoring of blood sugar. If the condition is not controlled, it can lead to serious complications, including high blood pressure, or preeclampsia, which can cause damage to both the woman and fetus and lead to early birth. Poorly controlled GD can also cause an extra-large baby, which raises the risk of nerve damage and often forces a cesarean birth.
GD can develop in anyone, but the risks are higher for women who are over 25 years old, are overweight, have a family history of diabetes, or are Latina, African American, South or East Asian or Pacific Islander.
The diagnosis shocked me. The doctor — one I’d never met before or would ever see again — assured me that if I followed the recommended steps, the baby and I would be fine. Nevertheless, I felt I had failed my baby by not taking care of him. And following the recommended measures proved challenging without a regular provider to answer my questions.
I was required to pick up a kit at the pharmacy and start using it. It turned out to be a glucose monitor. I had never seen the apparatus before and I had no idea how it worked. Instructions in the kit were not clear, and my HMO would not give me an in-person appointment unless it was an emergency. Finally, a friend who had been diagnosed with GD during her pregnancy taught me how to use the kit through a video call.
Because every obstetric appointment was with a different doctor, we always had to go through explanations of my history and condition. And I sensed that the doctors were in a hurry, perhaps to reduce the risk of spreading the virus. This left little to no room for me to ask my questions.
The situation was especially difficult since I couldn’t see family or friends who would have provided encouragement and support. My pregnancy, which was supposed to be a time of joy, was turning into a lonely, overwhelming experience.
But I was determined to do everything I could to deliver a healthy baby. Two friends who’d had GD provided very good advice. I bought a stationary bike online and exercised religiously. Once I learned to use the glucose monitor, I pricked my finger four times a day and maintained a controlled diet. I joined a Facebook group for women with GD, and it became an amazing source of support.
Most of the women in that group experienced similar feelings of failure when they were diagnosed. I also read inspiring stories of success. Women introduced their “sugar” babies to the group, reassuring the rest of us and motivating us to continue our diet and exercise regimens.
Celebrating in the new normal
In mid-November, a month before my due date, my husband and I opted for a drive-thru baby shower. We knew we had to be extremely careful. With Thanksgiving approaching, health authorities were bracing for another wave of infections and warning people to avoid large gatherings. We asked all our guests to wear face masks even though they would be inside their cars. We did, too.

We encouraged them to decorate their cars and line up a block away to drive by in a parade. We raffled small gifts and gave “aguinaldos,” a traditional Mexican gift bag. We filled it with candy, hand sanitizers and masks. We hired a “paletero,” an ice cream vendor with a cart, who handed out ice cream to guests passing by.
The baby shower lasted only an hour and a half, but it was delightful. We were learning how to enjoy life within the new limits.
On Nov. 30, I was not feeling well and decided to go to the hospital for a checkup. Once there, I was told my water broke and I was admitted for labor. My husband was allowed to accompany me, but he couldn't leave the room or he wouldn’t be permitted back.
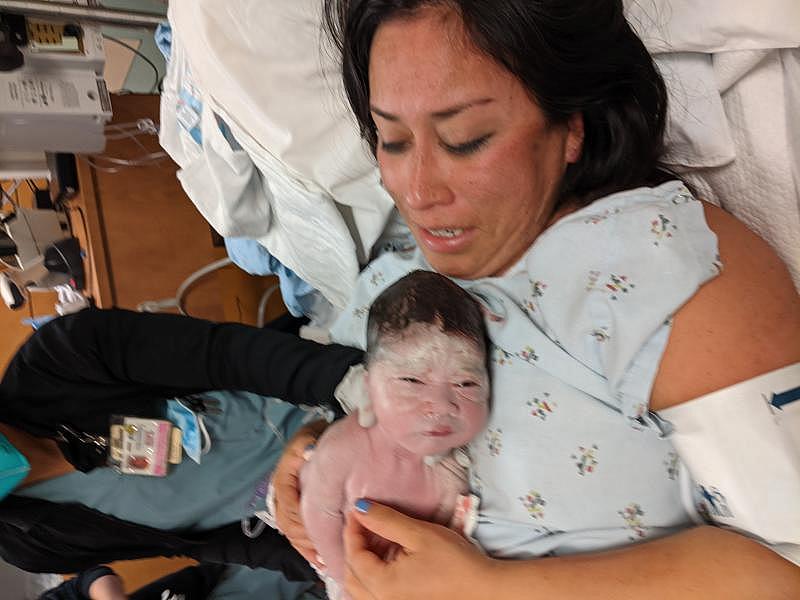
On Dec. 1 at 9:52 p.m. our baby, Andy, was born. A perfect, healthy little boy weighing 6 pounds, 4 ounces.
These days I’m in touch with friends who also had their babies during the pandemic. We swap stories and tips on how to manage parenthood during COVID-19 times. I have learned how to survive, connect with others, and even thrive in these strange circumstances. But my husband and I can't wait to get vaccinated and we're looking forward to seeing life get back to normal. We will finally be able to show our little one a world he can start to explore.

