Forward-thinking programs change our understanding of how to keep people healthy
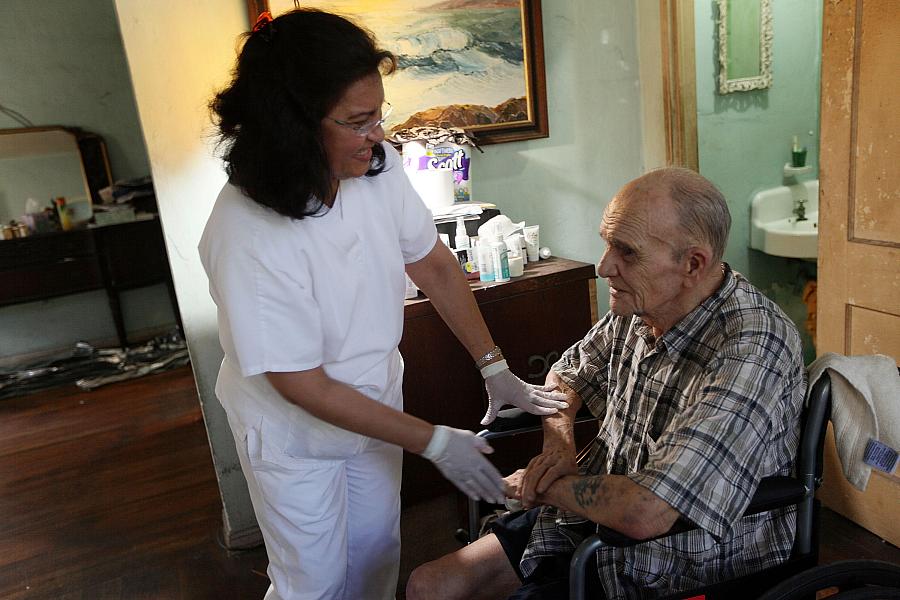
Joe Raedle/Getty Images
Several years ago, while working at a specialized program for geriatric patients in Massachusetts, I encountered an older woman who was struggling to deal with a severe mid-summer heat wave. She lived in a small apartment without air conditioning, and told me the heat was “sucking the life” out of her. She wasn’t sure she was going to make it, and her exam findings had me worried: Her lips were dry and cracked, and her skin appeared mottled. It was clear she was suffering from dehydration.
My immediate thought was that this patient required hospitalization. Even if I were to treat her with intravenous fluids in our clinic, I did not feel comfortable sending her back home to face the stifling heat.
But our case manager had a more creative idea. Rather than admitting this patient to the hospital — where she would be exposed to risks such as infections, blood clots, and deconditioning, not to mention the personal discomfort associated with hospitalization —the case manager suggested that we purchase and install a window air conditioner in her apartment. This approach would be particularly practical since the summer was just beginning and there would likely be at least a couple more Massachusetts heat waves before fall arrived. Our team decided to give this idea a try. By the end of the afternoon, an air conditioner had been installed in my patient’s apartment, and she appeared much better after receiving two liters of intravenous fluids in the clinic. At that point, we all felt comfortable discharging her home.
Unfortunately, the vignette I just described is the exception, not the rule, in the U.S. health care system. Too often, we rely on hospitals, emergency rooms, and nursing facilities because we are unable to address the underlying socioeconomic factors that drive poor health outcomes. Indeed, a famous analysis suggests that social circumstances and environmental exposures are responsible for 20 percent of health, twice the proportion attributable to traditional medical care. And, generally speaking, health care providers — doctors, nurses, pharmacists, and even community health workers — can do little to change these social and environmental factors because funding for medical and social services are kept separate.
So how was it that my clinic in Massachusetts was able to offer an air conditioner for my patient?
The reason is that I was practicing within a special geriatric program called the Program for All-Inclusive Care for the Elderly (PACE), which offers approved medical facilities considerable flexibility in caring for high risk older adults. To qualify for the program, patients must suffer from medical and functional problems — such as the inability to bathe or dress themselves— that would qualify them for placement in a nursing home. However, with the support of special resources offered through the PACE program — such as in-home support services, transportation to an adult day health center, social outings, meals, social work assistance, physical and occupational therapy, as well as traditional medical care — patients can remain in their home environment, living independently. Importantly, unlike traditional health plans, PACE programs may use their funding to pay for non-traditional services, like air-conditioners during summer heat waves. While there has yet to be a rigorous evaluation of the program, PACE patients not only have better health outcomes and are happier compared to similar control patients, but their emergency room and hospital utilization rates, as well as overall health care costs, are lower. Because of these encouraging numbers, the PACE program has now spread to 137 sites across 36 states.
The PACE model is only available to a small subset of the U.S. population, however, and many other groups— such as younger, chronically ill patients who suffer from homelessness, substance abuse, and behavioral health issues— could undoubtedly benefit from this more integrated and flexible approach.
This is why I was intrigued by a New England Journal of Medicine perspective article published earlier this month, which describes a strategy used in England that breaks down the wall between medical and social service spending and promotes many of the same benefits PACE patients experience. In England, patients with complex health needs, such as those with diabetes, lung disease, Parkinson’s, or advanced mental illness, receive what’s called a “personal health budget” that allows patients, in collaboration with their medical team and the approval of the British National Health Service, to spend money on the health-related services that are most important to them.
According to the article, many patients “choose to spend the largest part on home-based support services, choosing whom to employ and for what functions. But the budgets also cover such services as transport, psychological and physical therapies, nursing, podiatry, and leisure and equipment that address a health goal.” For example, one man with dementia used his funds to purchase a garden shed where he could garden within sight of his caregiver.
Personal health budget programs must be closely monitored, of course. The British news media have identified some instances in which these funds may have been used for potentially frivolous purposes. Nevertheless, the NEJM article reports that on the whole, evaluations of the program have shown it to be cost-effective and to improve quality of life for both patients and caregivers.
In our current political environment, it is not clear that a “personal health budget” program could withstand the partisan scrutiny in the U.S. While we are a doggedly individualistic society, we tend to oppose the expansion of programs that could be perceived as government “handouts.” Encouragingly, however, 13 states have received approval for demonstration projects in which health plans with responsibility for the overall expenditures of dually eligible patients would have the flexibility to use their funds to cover not just traditional medical services but also “home modifications, appliances, and cell phones as part of a case-management approach for populations with complex needs,” as the journal perspective notes.
From my perspective as a primary care clinician, I hope we can continue experimenting with models like the PACE program that empower those on the front lines, including patients themselves, to set spending priorities. So often, there are simple and inexpensive solutions to our patients’ greatest health challenges that could substitute for unnecessary, costly, and potentially harmful medical care.


