We’re failing at vaccinating kids against HPV — and that could cost lives
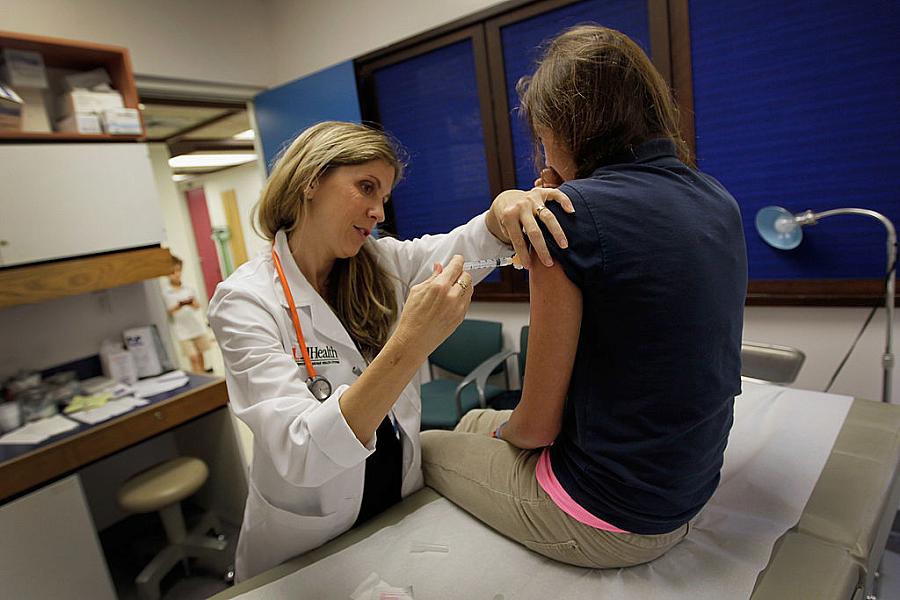
Pediatrician Judith L. Schaechter gives an HPV vaccination to a 13-year-old girl in her office at the Miller School of Medicine in Miami, Florida.
(Photo by Joe Raedle/Getty Images)
Only about one in six adolescents in the U.S. have been fully vaccinated against HPV, the human papillomavirus, by the time they turn 13, despite national recommendations that girls and boys be up to date on the shots at that age.
In that stark statistic lies a complicated story about a vaccine against a sexually transmitted virus that causes about 34,000 cancers a year in this country. It’s a story of official missteps, misinformation and confusion, and public anxiety about teen sex. Now, 13 years after the FDA approved the vaccine, HPV immunization rates fall so far short of public health goals that some medical experts have called it “an urgent public health problem requiring action.”
And it’s no mystery what action is needed.
“It’s time to think seriously about adding the HPV vaccine to school vaccine requirements,” said Jason L. Schwartz, assistant professor of health policy and management at the Yale School of Public Health.
With the measles vaccine consuming so much air time and public health attention this year, HPV seemed to fall off the radar. Then, in early July, British authorities announced they will begin offering the vaccine free to 12- and 13-year-old boys in all schools. Girls have received it in secondary schools for more than a decade, and now more than 80% of females aged 15 to 24 in the UK have been vaccinated. The decision to include boys brought new focus to vaccine policies and practices in this country.
Only Rhode Island, Virginia and Washington, D.C., require the HPV vaccine for school attendance, and the latter two jurisdictions have such broad exemptions and opt-out procedures that the policies “are requirements in name only,” Schwartz said.
Studies show that school entry requirements can dramatically boost adolescent vaccination rates. For example, in states that require teens to have meningococcal vaccination, coverage was 24 percentage points higher than in states without such a requirement, according to a 2016 study in Pediatrics. Rhode Island boasted one of the nation’s highest HPV immunization rates even before it began requiring the vaccine for seventh graders, in September 2015. Nevertheless, vaccination among boys increased significantly, compared with patterns in other states.
Cancers develop slowly so it will be years before anyone can measure the vaccine’s impact in preventing cases and saving lives, although experts around the world predict it will be significant. Nearly a decade of studies involving millions of people have shown the vaccine sharply reduces HPV infections, genital warts and pre-cancerous lesions. Researchers have found no serious health risks associated with the vaccine.
In short, it works and it’s safe. So why has it been slow to catch on?
“We’re still seeing the consequences of a very chaotic and contested rollout in 2006-2007,” Schwartz said.
The vaccine was initially approved for girls and young women, ages 9 to 26, as protection against one of the most common sexually transmitted infections — a virus linked to cervical cancer. Because people often contract the virus soon after they become sexually active, and the vaccine is most effective before infection occurs, the CDC urged vaccination at age 11 or 12. That recommendation, perhaps not surprisingly, generated fierce controversy.
Shortly after the vaccine came on the market, more than two dozen states considered requiring it for school entry. But critics pushed back, arguing that vaccination would encourage teenage promiscuity.
Over the years, public health officials broadened HPV vaccine recommendations to include boys and young men. Meanwhile, the health establishment repositioned the vaccine as protection against potentially deadly cancers. HPV is implicated in the vast majority of anal, penile, vaginal and throat cancers, in addition to cervical cancer.
Although the U.S. vaccination rate has increased steadily, it is not approaching the federal target of 80% coverage among adolescents by 2020. As of 2016, roughly 60% of 13- to 17-year-olds had begun the vaccine series, while 43.4% had completed it, Emory University researchers recently reported. But only 16% of adolescents were fully vaccinated by age 13, as recommended.
Research has shown that state laws requiring the vaccine or encouraging it through education are not associated with more, or more risky, adolescent sexual activity. But opposition to this vaccine has combined with the increasingly vocal and visible movement against vaccination in general to thwart new school HPV requirements. Last spring, the Connecticut General Assembly considered a bill to require the vaccine for ninth graders and for 12th graders who were not fully vaccinated by age 15.
Schwartz testified in support of the measure.
“That Connecticut requires 10 vaccines (against 14 diseases) for children and adolescents but does not currently require HPV vaccine can be misinterpreted as a suggestion that the vaccine is somehow less important than those others, a misunderstanding with potentially life-threatening consequences,” he wrote.
Vaccine opponents lobbied against the bill. It died in committee.
**

