'It's one of the silver livings': How COVID-19 pandemic could boost access to maternal health care
This story was produced as part of a larger project led by Marina Riker, a participant in the 2020 Data Fellowship.
Other stories in this series include:
Birth in the time of coronavirus
She already had a high-risk pregnancy. Then, COVID-19 struck.
Part 1: Birth on demand
Part 2: More than ‘a little snip’
Texas lawmakers aim to make maternal health a priority this year
Part 3: Filling the gap
Our women are dying': Texas lawmakers urged to extend Medicaid to a year after birth for new mothers

Marissa Mayberry, 28, talks as she sits on her bed and her husband Matthew, 28, listens at their home in Hondo, Texas on May 19, 2020. Marissa usually drives an hour each way to her midwife for prenatal care but has now been given the medical equipment, such as blood pressure cuffs, urine sticks and dopplers, to do it herself until the last few weeks of her pregnancy.
Josie Norris, The San Antonio Express-News / Staff Photographer
To keep our community informed of the most urgent coronavirus news, our critical updates are free to read. Ongoing coverage is available to subscribers. Subscribe now for full access and to support our work.
The afternoon sun shines through the window of Marissa Mayberry’s bedroom as she lies on the bed and lifts up her T-shirt to expose her pregnant belly.
Her husband, Matthew Mayberry, kneels next to her. He holds a fetal doppler, a machine used to listen to their baby’s heartbeat. He presses one hand to her belly to feel for the baby as he grasps the machine’s probe in the other, inching it across her skin.
“That’s a little knee,” Matthew says quietly.
“Yeah? Then maybe try right here,” Marissa replies, pointing to the lower part of her belly.
A rapid pounding thunders through the machine’s speaker: their baby’s heartbeat.
Marissa Mayberry, 28, unpacks her doppler at her home in Hondo. Marissa usually drives an hour each way to her midwife for prenatal care but has now been given the medical equipment, such as blood pressure cuffs, urine sticks and dopplers, to do it herself until the last few weeks of her pregnancy. Josie Norris /Staff Photographer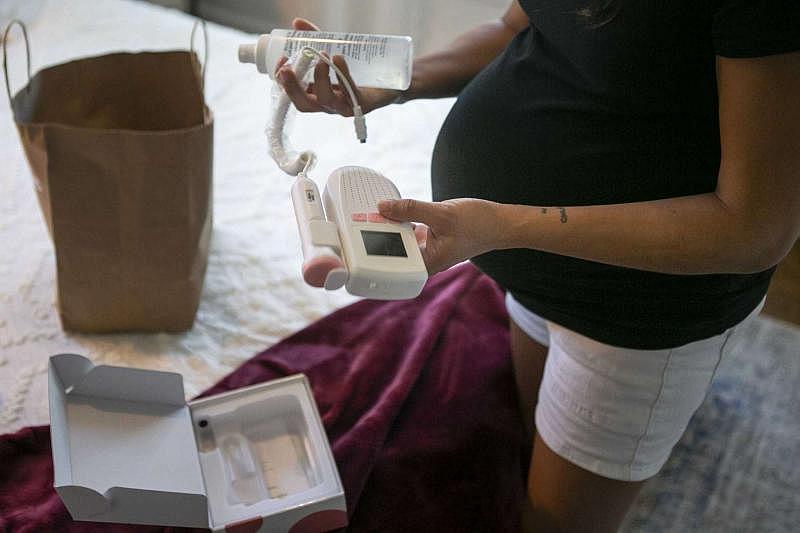
The Mayberrys, both 28, used to hear that sound only during prenatal checkups at their birth center in San Antonio, an 80-mile round trip from their home in Hondo. But in the early weeks of the coronavirus pandemic, Marissa’s midwife sent her home with the doppler machine, a blood pressure cuff and urine test strips that she could use to track her and her unborn baby’s health without coming into the office.
In the six weeks since then, prenatal care for Marissa has become a blend of at-home virtual visits with her midwife and in-office appointments every couple of weeks to undergo examinations and blood tests. It’s a system that Marissa hopes will continue after the pandemic passes — one that she says has made health care more accessible for her family and greatly increased her understanding of her own health.
For families preparing to bring newborns into the world, the coronavirus has disrupted prenatal care and birthing plans, sometimes leading to canceled appointments and limited visitors in hospital delivery rooms. It also has brought fears that moms and babies could be separated at birth if one tests positive for the virus.
But the pandemic has also spurred another change: a shift toward telemedicine, which could remove barriers to care for women and their families.
“It’s one of the silver linings,” said Dr. Tony Ogburn, the chair of the University of Texas Rio Grande Valley’s obstetrics and gynecology department. “It has really facilitated the move to telemedicine, which has been sluggish at best.”
Over the last three decades, the maternal mortality rate in the U.S. has doubled, forcing physicians and women’s health advocates to examine ways to improve care for women before, during and after their pregnancies. Today, women in the U.S. are more likely to die from childbirth or pregnancy-related causes than other women in the developed world, according to the U.S. Centers for Disease Control and Prevention.
In Texas, women face a number of barriers that can complicate their health care, such as a lack of insurance and shortages of medical professionals in their communities. And, depending on where a mother lives, it might take more than an hour to reach a hospital or birth center.
According to the American College of Obstetricians and Gynecologists, less than half of women living in rural areas in the U.S. can drive to a hospital offering OB-GYN services within 30 minutes. The shortage is particularly acute in Texas: More than 150 counties home to more than 2 million Texans have no OB-GYN, a situation largely driven by rural hospital closures. Midwives in those counties are even harder to come by.
Matthew Mayberry uses a doppler on his wife Marissa Mayberry to hear the baby's heartbeat at their home in Hondo, Texas on May 19, 2020. Marissa usually drives an hour each way to her midwife for prenatal care but has now been given the medical equipment, such as blood pressure cuffs, urine sticks and dopplers, to do it herself until the last few weeks of her pregnancy. Josie Norris, The San Antonio Express-News / Staff Photographer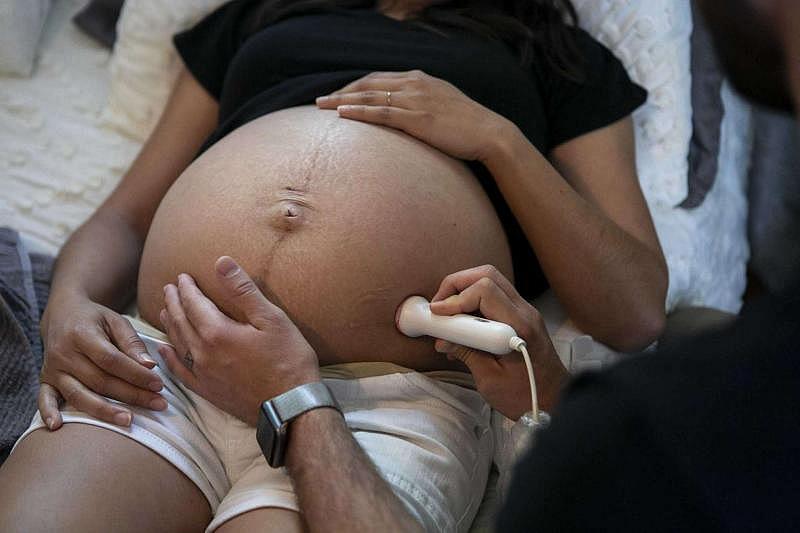
Women and health care providers hope that the shift to telemedicine could help fill those gaps.
“We really do hope that this breaks down barriers to care for our rural moms, and even some of our urban moms who work and have small children at home and it’s just really hard for them to get into the office for a visit if they have to sit in traffic for an hour,” said Heather Butscher, who works in Houston for the March of Dimes, a nonprofit dedicated to improving the health of moms and babies.
For years, many clinics and medical providers had been reluctant to make the switch, in large part because of fears that virtual health platforms wouldn’t comply with health privacy laws. Government-backed insurance programs such as Medicare and Medicaid also have limited the amount doctors earn from conducting virtual visits.
But when the coronavirus began to spread across the U.S. and health clinics were forced to reduce contact with patients, medical providers scrambled to find technological platforms that complied with the Health Insurance Portability and Accountability Act. At the same time, the federal and state governments waived reimbursement rules to allow medical providers to earn the same amount for visits over phone or video as those done in person.
The result: Within weeks, health providers were providing all sorts of medical care virtually — including prenatal visits — a shift that could’ve taken months to unfold otherwise.
“People were so reluctant to do it,” Butscher said. “But now, we’ve been forced into it.”
Confronting the digital divide
Medical clinics across San Antonio have embraced the move. Dr. Patrick Ramsey, a maternal-fetal medicine specialist at UT Health San Antonio, said its clinics ramped up to provide care over the phone or through Zoom when in-person exams aren’t necessary.
He and other physicians are able to write prescriptions for blood pressure monitors and blood sugar test kits so expectant moms can check their levels at home. By measuring themselves, Ramsey said, some of his patients have been more active in taking control of their health, rather than relying solely on their doctors.
“It has increased health literacy,” Ramsey said. “The downside is the disparities part. It’s a great platform to use to make access better, but we’re disparately increasing access. And unfortunately, the patients who probably need access the most might not be able to get it.”
In South Texas, women of color and those who have lower incomes are more likely to live with pre-existing conditions that are driven by poverty — such as diabetes, obesity and high blood pressure — and can turn dangerous during pregnancy.
At the same time, low-income women may lack access to technology needed to participate in telemedicine. Ramsey said providing telemedicine to everyone will mean finding creative ways to give families access to that technology, even if it means setting up Wi-Fi hubs at community health clinics.
It could also mean providing those visits by phone, rather than video calls, he said. Nearly 1 in 4 Bexar County households don’t have a desktop or laptop, and nearly 17 percent don’t have internet access, according to 2018 census estimates.
But for patients who do have access to that technology, it’s now much easier to get care.
“It’s a big game-changer,” Ramsey said. “(For example), my patient who lives two hours away from San Antonio with a 2-week old baby — she would have to put her in the car, get the car seat and then have to worry about COVID-19 coming into the clinic. She can do it all from home.”
‘More empowered’
In late March, as the number of San Antonians infected with COVID-19 was doubling every three days, Alisa Voss Godfrey, owner of the San Antonio Birth Center, said she realized that the safest way to protect her clients and their newborns was to limit their physical presence in the birth center.
“They said telehealth, and they said coronavirus, and they said this is happening,” Godfrey said. “I got out my American Express, and I bought about $6,000 in extra supplies and equipment.”
At an average cost of $102 per client, Godfrey ordered doppler machines, blood pressure cuffs, urine analysis strips and tape measures to send home with the expectant mothers in her care. In Texas, licensed midwives such as Godfrey care for only women considered low-risk: those who don’t have pre-existing or medical conditions that could complicate their pregnancies.
Marissa Mayberry, 28, poses at her home in Hondo, Texas on May 19, 2020. Marissa usually drives an hour each way to her midwife for prenatal care but has now been given the medical equipment to do it herself until the last few weeks of her pregnancy. Josie Norris, The San Antonio Express-News / Staff Photographer
Godfrey has found that by taking their own measurements, women have become more aware of their health and what’s normal — and not normal — for them.
“They are actually more empowered, so why would we not want people to be more empowered?” she said. “That’s exactly what we stand for.”
That has been Mayberry’s experience. Prenatal visits over Zoom also meant she didn’t have to take off work, find child care for her 3-year-old son and drive an hour each way to the birth center. And, with visitors limited in the center, her husband was able to be by her side at every visit.
Last week, it took her and her husband only 49 seconds to find their baby’s heartbeat with the doppler — significantly faster than the first few times they tried.
“We’ve had a lot of fun learning,” Mayberry said. “Like when my baby is moving, I’m like ‘Oh, that makes sense because the back is over here,’ and it’s almost like we can catch the heartbeat immediately now because of how well they’ve trained us to learn the position.”
She said the last few weeks have allowed her to feel more connected to her husband and their unborn baby, whom she is due to deliver at the San Antonio Birth Center in early June. But because she could go into labor any day now, her time with telemedicine is now on pause.
Until the birth, she must head to the birth center for her weekly checkups — in person.
Marina Starleaf Riker is an investigative reporter for the San Antonio Express-News with extensive experience covering affordable housing, inequality and disaster recovery. To read more from Marina, become a subscriber. marina.riker@express-news.net | Twitter: @MarinaStarleaf
[This story was originally published by San Antonio Express-News].

