Safety Net: Without Health Insurance, Many Put Off Critical Treatment
Giana Magnoli reported this story for Noozhawk as a 2013 California Endowment Health Journalism Fellow.
The first part to the series can be found here:
Safety Net: Patchwork of Clinics Struggles to Keep Santa Barbara County Healthy
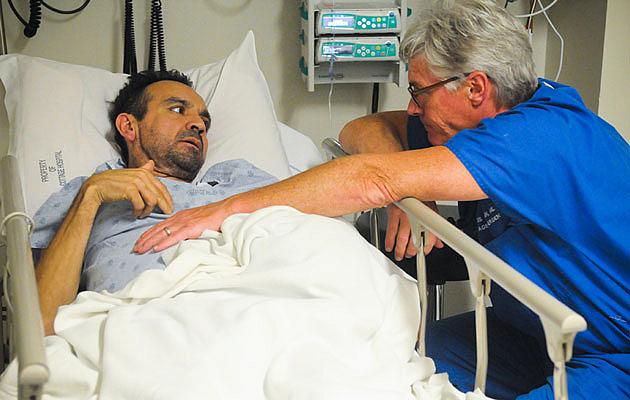
Dr. Chris Flynn listens to Alonso Camarena talk about the pain he’s experiencing during a recent visit to the Santa Barbara Cottage Hospital emergency room. Camarena, who does not have insurance, discovered he had cancer on his first visit to an emergency room two years ago. (Lara Cooper / Noozhawk photo)
“Can I tell you the whole story?” asked Alonso Camarena while lying in an emergency room bed at Santa Barbara Cottage Hospital.
Dr. Chris Flynn took a seat beside the man, who was covered by a thin hospital gown and blanket, and leaned in closer. Camarena was about to share a plight that is all too common for uninsured patients in Santa Barbara County. He had finally come to the ER that afternoon because he was in too much pain to ignore.
As Flynn examined his distended stomach, Camarena explained that he has worked at a Carpinteria motel for almost a decade, but doesn’t have health insurance because his employer doesn’t offer benefits. Primary care, even for basic check-ups, was out of the question for Camarena, who was wincing from the pressure of the doctor’s touch. About two years ago, the only other time Camarena came into the hospital, was when they found it.
A tumor.
Camarena had surgery that removed some of the mass, but not all of it. He had to return to work instead of focusing on his health.
When he came into the ER this time, Camarena was given pain killers and told to rest until he could be admitted to the hospital for treatment. Flynn pulled the curtain behind him as he left the room to look at some scans of Camarena in his office. A scan of the man’s abdomen showed a menacing black mass in the middle of his body.
At this point, Camarena’s liver is three times the organ’s normal size.
He has a rare form of cancer that can be caused by environmental exposure to compounds such as asbestos, said Flynn, who added that the case is typical of local uninsured patients. Many men and women over the age of 26 don’t qualify for any type of public insurance such as Medi-Cal, and can’t afford private health plans, so they forego it altogether.
Flynn, an experienced emergency medicine doctor, sees it all the time. About 5 percent of Cottage Hospital's 43,000 ER patients per year have no way to pay, and those numbers are even larger in the North County.
“They’re all taking a gamble,” Flynn said, looking over Camarena’s charts. “It’s all really good until it gets really bad.”
When he sees patients forsake medical care until an illness is so advanced that treatment may not help, he gets angry.
“It’s just wrong,” Flynn said of his latest patient. “He didn’t get the chance to fight this cancer when the odds were in his favor.”
Getting insurance coverage for these people is a big part of the federal health-care reform, which goes into effect Jan. 1. Preparing for the sweeping changes with the Patient Protection and Affordable Care Act, also known as Obamacare, is challenging, said Liz Snyder, deputy director of primary care for the Santa Barbara County Public Health Department.
“But we can’t lose sight of how incredible this is,” she added. “This is history. This is an incredible time.”
There are major components to the federal reforms: individual mandates for most taxpayers, making more people eligible for insurance coverage through Medi-Cal expansions and the state exchange, and changing the care model to focus more on preventative, ongoing care for patients.
Through the Medi-Cal expansion, CenCal Health, the local administrator of Medi-Cal, expects 30,000 more people to enroll during the first 18 months of the Affordable Care Act between Santa Barbara and San Luis Obispo counties. That’s a 30 percent increase, CenCal CEO Bob Freeman said.
Counties are taking the lead to get people signed up for Medi-Cal, since county agencies are the ones that determine whether someone is eligible, he said.
Expanding eligibility will apply to thousands of county residents, and even more will be eligible for subsidies on the state insurance exchange, Covered California.
The exchange has plans from private insurance companies for pre-determined prices, but the California Department of Insurance has no control over the rates, at least for now.
People who earn below $44,000, or $94,000 for a family of four, can receive subsidies for their insurance plans, but residents at every income level can buy a plan through the exchange.
For Santa Barbara, San Luis Obispo and Ventura counties, there are plans on the exchange from Anthem PPO, Blue Shield PPO, Kaiser Permanente HMO and Ventura County Health Plan HMO.
Realistically, however, only two options are available for most local residents since there are no Kaiser providers serving Santa Barbara County and only Ventura County employees can sign up for the county health plan HMO.
Covered California expects 95,000 people in the tri-counties to be eligible for subsidies and there will be five levels of coverage plans. Prices are based on a person’s age, income and family size.
Many newly eligible people could already be patients with the county clinics, but they may not be coming in regularly for preventative or ongoing care, said Dr. Takashi, Wada, director of the Public Health Department.
If people have insurance for the first time in 10 years, or ever, they could require a huge amount of care and referrals, which will severely tax the health-care system until it stabilizes, he said.
Patients of the county often need more complex care, as well, with five to 10 different health issues because of the effects of poverty and stressors associated with that.
“Down the road I think it will be a lot better, but that first year is going to be a huge challenge for the whole system,” Wada said.
The Public Health Department’s eight clinics serve 31,000 patients a year, with about 120,000 visits.
As of now, 25 percent to 35 percent of Public Health Department patients have no insurance, and that population includes a lot of working poor people, many of whom don’t get any coverage from their employers.
The highest concentration is in Carpinteria, where 35 percent of patients are uninsured, Snyder said.
More people — in fact, most — will be eligible for public or private insurance after the new laws are implemented, but some still won’t be covered.
Some patients are “paperwork challenged” or can’t find time to go to the doctor, said Dr. Charles Fenzi, chief medical officer for the Santa Barbara Neighborhood Clinics.
“We have a large number of folks who are currently not well treated for their mental health issues," he said. "That’s a huge problem in the city of Santa Barbara. People aren’t well enough controlled with meds to get in to see us or do paperwork, so for them, we want to provide case management.”
He added: “The same is true with folks who are working two jobs, live in one room, raising six kids and have diabetes. When do you take care of your diabetes? There’s no time.”
Outreach specialists are critical for these populations, and they offer rides to appointments, reminders about prescriptions, and help with disease management so people can continue to care for themselves and their families.
Undocumented people — who aren’t citizens or legal immigrants — are conspicuously left out of health-care reform altogether, and clinics and counties will not be reimbursed for providing care.
The Public Health Department receives more than $10 million in realignment funding to support the cost of caring for the uninsured and providing other health-care items that aren’t reimbursable.
However, the county will be losing 75 percent of that funding, making it one of the hardest hit in California.
“We always knew the governor was going to take back some of our funding,” Wada said.
Next year, the Public Health Department will be losing $2.3 million of realignment funding, and in 2014-2015, that number jumps up $7.3 million.
“The state’s reasoning is that since the Affordable Care Act is kicking in, they assume people will now be insured,” he said.
“We’re working with CenCal and our county Department of Social Services on ways to try convert the uninsured into the Medi-Cal system. We still may have to make some degree of cutbacks.”
This story originally ran on Noozhawk.com September 11, 2013
Photo Credit: Lara Cooper, Noozhawk staff

