The 'Skinny Fat’ Indian: Why South Asians Face a Higher Risk of Diabetes
The story was co-published with India Currents as part of the 2025 Ethnic Media Collaborative, Healing California.

Asian Indian women have the highest rates of gestational diabetes in the United States.
Pexels // Denys Mikhalevych
When Snigdha was diagnosed with diabetes in 2008, she felt betrayed and shocked.
"I was thin, did not have a sweet tooth, and had never been a foodie. I am lactose intolerant, so I didn’t even have ice cream! Nobody in my immediate family had diabetes. And yet here I was.”

Snigdha, a Bay Area resident, was six months pregnant with her first child in November 2008, when a routine glucose test revealed she had gestational diabetes.
Her Gestational Glucose Screening, measuring glucose levels six months into her pregnancy, came in at 163 mg/d, well into the diabetes range. She also failed the subsequent glucose tolerance test. Snigdha didn’t think she fit the profile of someone with diabetes. She was healthy, had a low BMI, and no immediate family history of the disease.
In South Asian families, diabetes is often seen as something that comes after weight gain, middle age, and clear warning signs. It’s often associated with older relatives who casually say, “I have a sugar problem.”
Snigdha’s diagnosis points to a larger truth that remains hidden — Asian Indian women have the highest rates of gestational diabetes in the United States.
“One, we don't secrete enough insulin, so we don't have the metabolic capacity,” said Dr. Venkat Narayan, executive director at the Emory Global Diabetes Research Center. “Second, our muscle mass is low, so we don't burn glucose readily. Third, we are easily prone to depositing fat in the liver.”
After we eat, blood sugar rises, and the pancreas releases insulin to help cells, especially in the liver and muscles, absorb glucose. But in type 2 diabetes, the cells become insulin-resistant, and over time, the pancreas can’t keep up, leading to rising blood sugar and eventually, diabetes.
During pregnancy, hormones from the placenta can interfere with the way insulin works. And if a mother has gestational diabetes, it can lead to medical complications like miscarriage, hypertension, as well as the baby having an increased risk of respiratory problems at birth, seizures, obesity, premature birth, and Type 2 diabetes later in life.
“If we don't know our numbers, don't know our health status,” the stress of pregnancy will easily reveal underlying factors like diabetes, says Dr. Alka Kanaya, an expert in type 2 diabetes, obesity, and cardiovascular disease at UCSF. For this reason, she strongly advocates that women have their health and key metrics evaluated before becoming pregnant.
“That woman is going to end up with gestational diabetes. That child is going to be that fetus living in a milieu of high glucose levels, already priming that child to have risk factors when they're born, so that they develop diabetes. It's a vicious cycle.”
Snigdha’s Gestational Diabetes Journey
In the wake of her diagnosis, Snigdha faced the reality of having to manage her condition while pregnant. She was given metformin, a medication to treat high blood sugar levels, and sent to a nutritionist.
“That's the first time counting the carbs came into my life,” Snigdha recalls. The nutritionist asked about her diet and lifestyle and offered suggestions.

Before this, “9 pm was dinner time,” said Snigdha. Not anymore. While eating an early dinner is a lifestyle change that has stayed with her since, altering her habits and taking medication were not enough to lower her glucose levels.
Snigdha had to get insulin shots to get her numbers under control.
With little body fat apart from her baby bump, she struggled to find a spot she could pinch for insulin injections. Snigdha’s sister-in-law, who had a similar health profile, also had gestational diabetes. “That made me feel a little less lonely.”
Snigdha welcomed a healthy baby, and within weeks of her son’s birth, her glucose levels returned to a safe range, and she stopped all medications. But that return to normalcy came with a warning from her OB/GYN. “From now on, you are at high risk for diabetes later, so you have to be tested regularly.”
Snigdha stayed slim and healthy, but seven years later, during her second pregnancy, early testing revealed gestational diabetes again.
The shock had faded, replaced by quiet acceptance. Snigdha followed the same treatment path through delivery.

Snigdha’s food diary during her second pregnancy.
Courtesy of Snigdha
“Two days after he's born, my blood sugar falls within range,” remembers Snigdha, and she went off all diabetes medications again.
She continued to follow a healthy lifestyle over the next few years, but then in 2020, three years after her second child was born, Snigdha’s fasting glucose numbers — a test taken when your glucose should be at its lowest — started to rise.
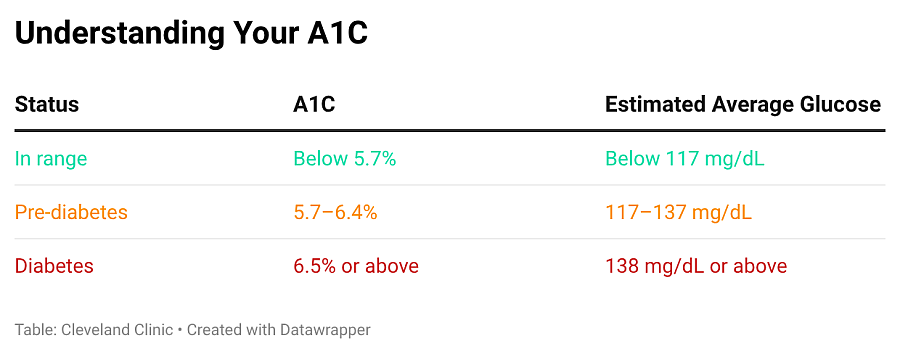
She was only 44, and her BMI was only 23, but her glucose level at 111 mg/dL put her squarely in the pre-diabetic range. Her HbA1C level was also rising — 6.1 in 2022 and 6.6 in 2024.
Snigdha’s path to diabetes followed a pattern predicted by research: people who experience gestational diabetes are more than 11 times as likely to develop diabetes within nine years after delivery compared to those who do not.
The Skinny ‘Fat’ Indian
Dr. Deepika Reddy, an endocrinologist at the University of Utah, explains that a diabetes diagnosis is often linked to excess body fat, particularly visceral fat around the organs, which triggers inflammation and contributes to insulin resistance. But BMI doesn’t always accurately capture this risk in certain populations like South Asians.

The “thin Indian with a pot belly” is a visible sign of a growing epidemic of obesity and type 2 diabetes, particularly among Asian Indians. Research from an NIH study shows that Indians tend to develop diabetes at a younger age and at lower BMI levels than white Caucasians.
People who appear lean may still have a higher body fat percentage. This “skinny-fat” body type may develop before birth due to changes in gene regulation. Low levels of vitamin B12 and folate in the mother, along with high blood sugar during pregnancy, are likely major causes.
At Emory University, Dr. Narayan has researched diabetes since 1992. “When you think of diabetes and why South Asians or Indians are at higher risk for diabetes, there are two axes that we should pay attention to — one is the biological axis, and the other is the lifestyle and environmental axis.”
In 2015, his team hypothesized that Type 2 Diabetes may not be a single disease but could represent Type 2a, an insulin-resistant type of diabetes, and Type 2b, an insulin-deficient type of diabetes.
If someone is not secreting enough insulin, even a small addition of fat can be excessive. “You don't have the ability to compensate,” explained Dr. Narayan. “You can now be insulin resistant, giving rise to the ‘skinny fat Indian’ phenotype.”
An Inflection Point
Snigdha’s PCP has not put her on any medications yet, asking her to give diet and lifestyle a try as well as an app to count her carbohydrate intake.
“I am not good with that,” admits Snigdha. A busy media professional raising two kids, she doesn’t have time to make a quinoa salad for herself and a separate meal for her family.

A typical breakfast for Snigdha.
Courtesy of Snigdha
However, cutting carbs has been a game-changer for her. “I started making minute changes. Now breakfast is usually one slice of bread, and with, say, cucumbers, an egg.”

Snigdha acknowledges, “I probably should (have) dedicated time for actual exercise.” Finding time is a common challenge, but one that doctors say can make a meaningful difference.
“It has to start with moving more,” says Dr. Kanaya. “By exercising, you get the muscles to be insulin sensitive — that’s how you decrease insulin resistance.”
Snigdha knows that an inflection point may be on the horizon and is committed to working on her lifestyle by eating right and monitoring her blood sugar levels.
Diabetes can lead to serious complications such as heart disease, strokes, kidney damage, nerve problems, dementia, and vision loss if it is not properly managed.
A Call For More Research
More than 800 million people worldwide have diabetes, and about a quarter are Indians, says Dr. Narayan. “Our knowledge is borrowed from other populations. When you look at the amount of research that comes out of Indian populations, whether in India or in the diaspora, it's about 1 to 2%. So there is a huge mismatch between the knowledge and our application of that knowledge.
“I think unless we invest more in the research at the biological level as to why South Asians are more prone, I don't think we're going to solve the problem.”
At UCSF, Dr. Kanaya is working to develop better risk prediction models for South Asians through the MASALA Study. “It's so important for people to be in research studies. We have very little data on South Asians because they don't participate. So if you hear about a study, please join.”

