Steep cost of long-term preemie care takes heavy toll on overburdened families
The story was originally published by the South Florida Sun Sentinel with support from our 2023 Data Fellowship.
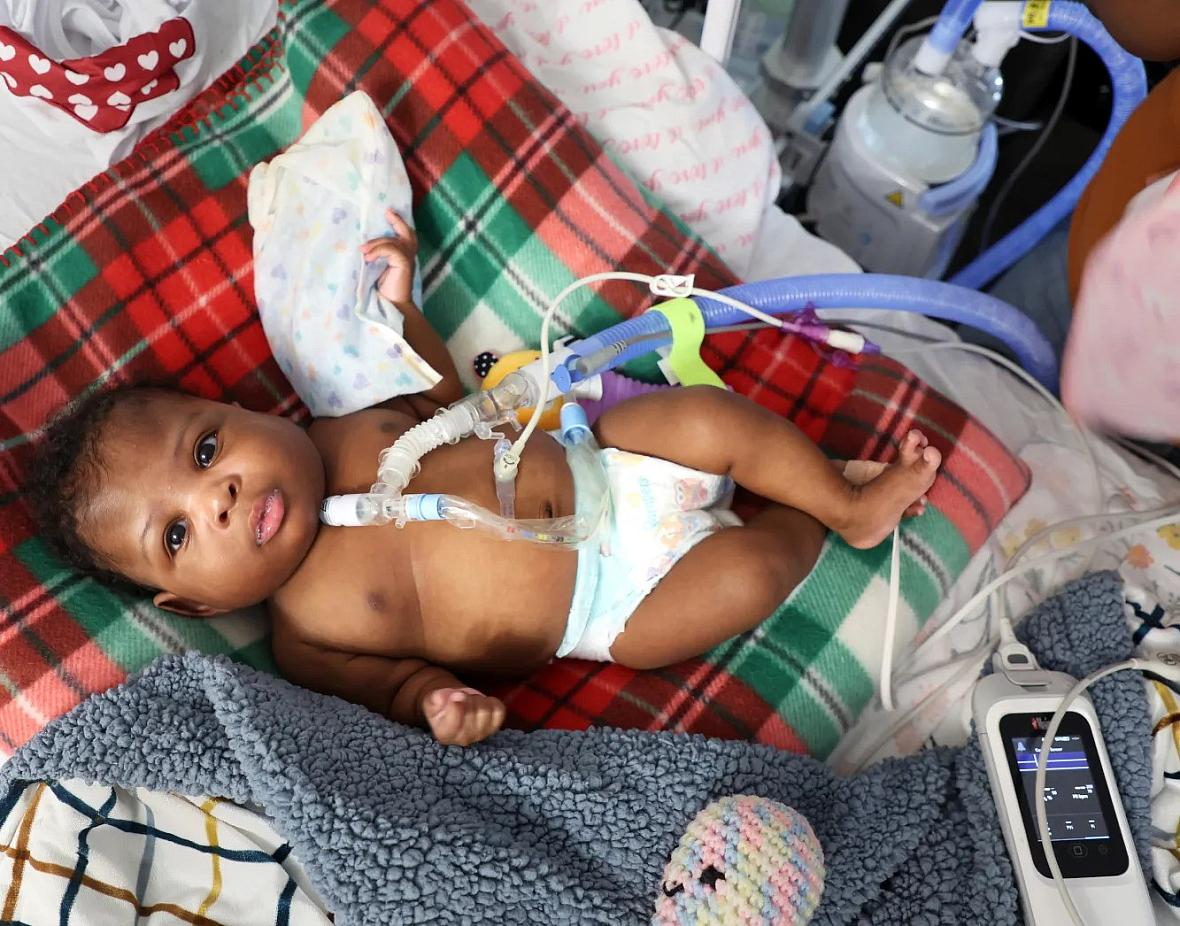
Darionna Williams in her crib at home in Fort Myers on Feb. 9, 2024, when she was 9 months old. Williams was born weighing 9.5 ounces. She is hooked up to a heart monitor and other life-saving machines. “I watch her to make sure she is breathing, and if she stops for three or more seconds, then this (monitor) will pick it up,” her mother, T’kyia White says.
(Carline Jean/South Florida Sun Sentinel)
Darionna Williams sits propped on pillows in her crib like a small doll, wearing a frilly red-and-white dress covered in hearts, a blankie clasped in her tiny hand.
Her hospital-grade crib sits in the middle of the chaotic living room. Tubes protrude from the infant’s throat, stomach and foot, a cord connecting her to a nearby monitor.
A colorful mobile playing a lullaby circles above Darionna’s head, a soothing but startling accompaniment to the beeps and whooshes of the machines that deliver oxygen into her lungs and formula into her intestine.
Eleven months after an emergency C-section brought Darionna into the world 15 weeks early, the baby’s tiny hand reaches for her mother’s finger. T’kyia White, Darionna’s mother, grabs onto her daughter’s thumb while carefully adjusting the tube in her baby’s tiny throat. She glances at a monitor tracking her daughter’s vitals, acknowledging how much her baby’s life hinges on a quick reaction.
“I watch her to make sure she is breathing, and if she stops for three or more seconds, then this (monitor) will pick it up,” White says.
In her Fort Myers apartment, White is alone in her struggle to care for her fragile daughter. However, across Florida many more parents spend their days and nights watching monitors, adjusting tubes and struggling to keep their premature babies alive. Preemie children, many with undeveloped organs, face incredible odds to survive and thrive, and often require years of monitoring and medical interventions that drain family and government finances.
Premature births in Florida — those earlier than 37 weeks gestation — rose 4% over the last decade, even as the state’s overall birth rate declined nearly 10% in the same time period, according to Florida Health Charts.
Florida doctors see a health crisis unfolding: Infant mortality rates in the state persist at levels higher than the national average, but equally as concerning is the rising number of premature births. More advanced technology allows doctors to perform life-saving measures on newborns the size of a shoe; premature babies tend to die within 28 days, leaving families grieving; fragile children are sent home from hospitals with breathing machines, feeding tubes and other medical devices to keep them alive.
An already burdened public health system is forced to absorb the soaring costs of long-term care.
“If more babies are born early and small, it’s a marker of the health of the pregnancy, and that means in Florida, mothers and infants are not headed in the right direction,” said Sarah Wood, a Harvard researcher who has studied infant health in Florida.

T’kyia White, 32, holds her daughter Darionna Williams in her Fort Myers home. Darionna weighed only 9.5 ounces when she was born, one of many Florida babies who are born premature and low birthweight.
Carline Jean/South Florida Sun Sentinel
Babies born too small or too soon are three times more likely to need specialized medical and developmental services before the age of 3, twice as likely to need additional intervention services throughout their school career, and twice as likely to have a lifelong health issue that affects their quality of life.
In addition, prematurity is one of the top causes of the death of infants before their first birthday.
With one in 10 babies in the state born premature, and one in nine babies born full term but underweight, the state’s future generations need better interventions to prevent birth outcomes from worsening.
Experts say many of these premature and low-weight births could be prevented if state spending and policies addressed them more comprehensively in three key areas:
- Insurance. Florida’s health system for low-income women is broken. It is one of only 10 states that has refused to expand Medicaid under the Affordable Care Act. Women in Florida are going into childbirth with unmanaged chronic health conditions, and while they bear some responsibility, a lack of insurance contributes. At the same time, Florida’s low Medicaid reimbursement rates deter maternal health providers from accepting patients with those plans. That has created long wait times for women at practices that do accept their Medicaid coverage.
- Providers. Too many women live in areas without maternal healthcare providers. Health experts say the state needs to invest in bolstering the maternal care workforce, and making more providers available to address risks for premature births for women in counties and ZIP codes where obstetric care is dwindling or nonexistent
- Education. Many women do not know where to find obstetric doctors, or even the educational materials to guide them through their pregnancies. Florida needs to increase education spending to help women overcome their hesitancy to get care, teach pregnant women signs of fetal distress and preterm labor, and encourage doctors not to dismiss or mistreat pregnant women, particularly Black women, when they complain of medical concerns.
“If we are saying it’s one thing or the other that is driving this, we are only going to take small steps,” said Dr. Stevenson Chery, medical director at BCOM Health, a government-funded health clinic in West Park in Broward County. “In order to address this problem and see progress, we are going to need to address the whole system.”
Maternal fetal specialists who treat high-risk pregnancies worry that the incidence of premature births will worsen with Florida’s new abortion restrictions. Since the U.S. Supreme Court overturned Roe v. Wade in 2022, Florida passed a 15-week abortion ban, and on May 1, a six-week ban will go into effect.
“Some of our leaders will make a big, big deal about decreasing mortality and right to life,” said Dr. Mark Hudak, a neonatologist and chairman of pediatrics at the University of Florida College of Medicine – Jacksonville. “But then when it comes to making sure that at the moment of birth the baby has the best chance to live … and if the baby has medical issues the appropriate resources are there … then that’s a different story.”
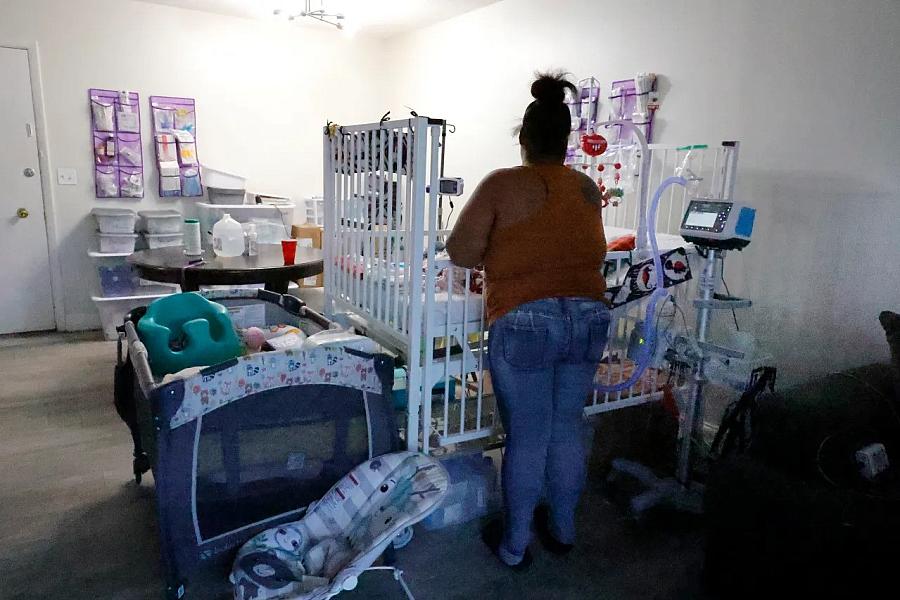
The living room at T’kyia White’s Fort Myers home is filled with equipment and supplies for her daughter Darionna Williams, who weighed only 13 grams at birth. She is hooked up to a heart monitor and other life-saving machines.
(Carline Jean/South Florida Sun Sentinel)
Why Florida mothers are having babies early
Doctors now know that preterm births and a mother’s health are closely related.
In Florida, women increasingly are entering pregnancy with unmanaged health conditions and no knowledge of medical risk factors for preterm labor and preterm birth. More state spending needs to focus on women’s healthcare, health experts say.
Florida designated about $150 million in the 2023-24 fiscal year for maternal and infant care programs, less than the $211 million allotted for cleanup of contaminated sites for redevelopment, or the $4 billion to address congestion on Florida’s highways and roads.
March of Dimes research points to Florida’s Medicaid policy as a factor in poor birth outcomes.
Florida is one of 10 states where the Affordable Care Act’s expansion of Medicaid for low-income adults has not been implemented by state lawmakers. That leaves a gap for women near poverty levels who can’t access insurance. A March of Dimes report shows about one in six women of childbearing age in Florida are uninsured as of 2021, making it more challenging to begin a healthy pregnancy.
“The state is spending money for programs for preterm babies, but not for prevention,” said Caroline Valencia, director of Maternal & Infant Health Initiatives for March of Dimes Florida. “Expanding Medicaid would give those people of childbearing age access to primary care. So before they think about getting pregnant, they could identify their health issues and get those under control.”
Although lower-income women in Florida can get Medicaid once pregnant, the delay to enroll and become approved presents a barrier to timely prenatal care.
One of every four mothers in Florida, or 24%, arrives at the hospital to give birth having inadequate prenatal care, higher than the national average of 15%, the March of Dimes report shows.
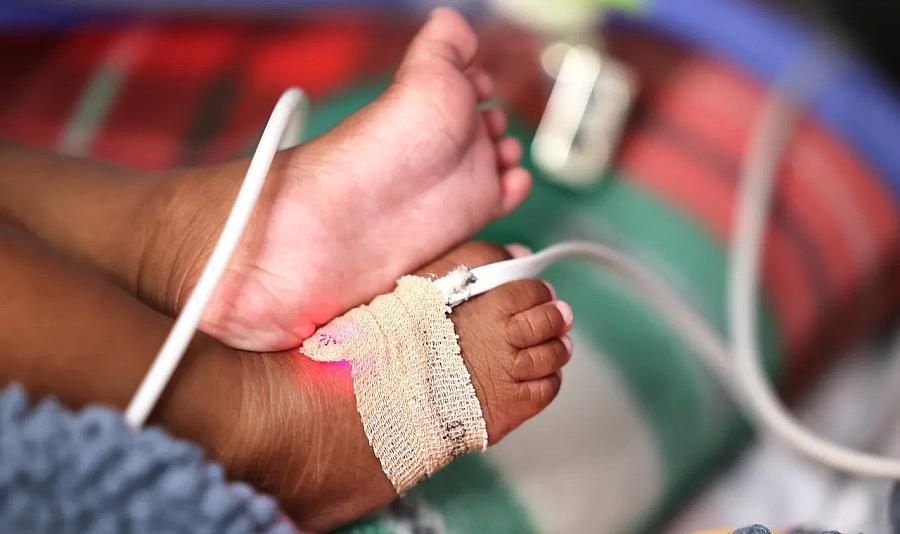
Tubes connected to machines for breathing and supplements for food keep Darionna Williams alive.
(Carline Jean/South Florida Sun Sentinel)
White, Darionna’s mother, was uninsured, overweight and experiencing blood clots when she went to the emergency department of HealthPark Medical Center in South Fort Myers with the flu in spring 2023. A doctor discovered she had preeclampsia, a life-threatening hypertensive disorder. An ultrasound revealed she had a dangerously low level of amniotic fluid. An immediate emergency C-section would be needed to save her baby’s life.
Baby Darionna weighed only 9.5 ounces at birth, not even a pound and barely the size of a shoe. She spent 249 days — more than half of her first year — in the neonatal intensive care unit at Golisano Children’s Hospital in Fort Myers. The life-saving surgeries and interventions performed at Lee Health, a public health system that operates the children’s hospital, kept the feisty newborn alive but came with a six-figure bill, mostly covered by the state-managed Medicaid program.
Now that she is home, Darionna’s complex medical needs must be managed by her single mother, who calls her baby “my little fighter.”
To stay alive, Darionna needs four medications and specialized formula administered through a feeding tube. A tracheostomy tube to help her breathe needs regular cleaning, and she requires a foot monitor to gauge her heart rate and oxygen levels.
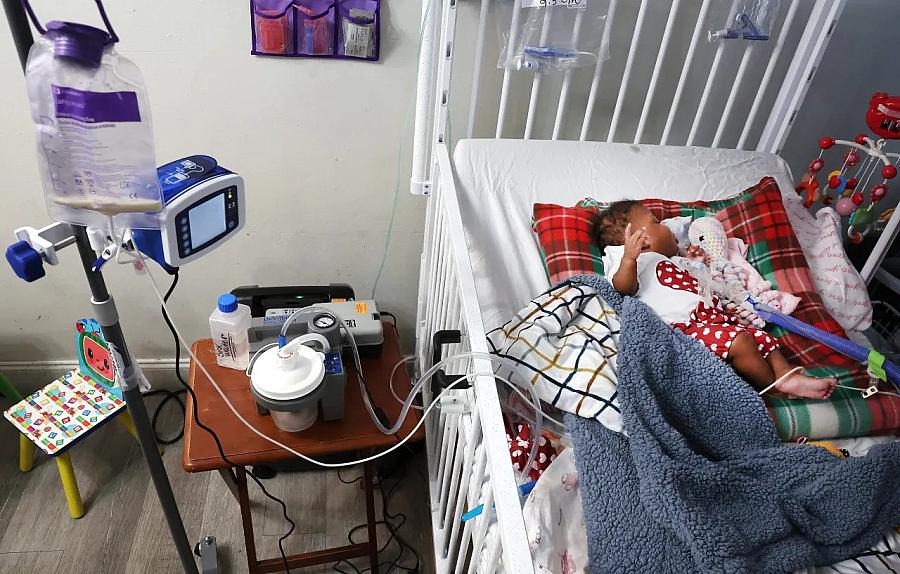
A gravity bag with baby formula is used to feed Darionna Williams. The baby is hooked up to a heart monitor and other life-saving machines. “I watch her to make sure she is breathing, and if she stops for three or more seconds, then this (monitor) will pick it up,” her mother T’kyia White says.
(Carline Jean/South Florida Sun Sentinel)
Darionna also needs to see specialists. A pulmonologist for her under-developed lungs. A cardiologist to ensure enough blood flows to her heart. A nephrologist for possible kidney disease. She will soon start physical therapy, speech therapy, occupational therapy. Appointments require transportation arranged through Darionna’s Medicaid plan, and travel requires hookups to portable monitors and oxygen tanks.
In White’s crowded apartment, storage bins filled with medications, syringes and medical supplies sit stacked against a wall. Behind the crib, a shoe organizer holds gauze packets, medical tape, alcohol wipes and spare parts for the trach tube.
“It’s a lot of work … it’s challenging but you get through it,” White says as she adjusts her daughter in the crib. “It’s tough, though.”
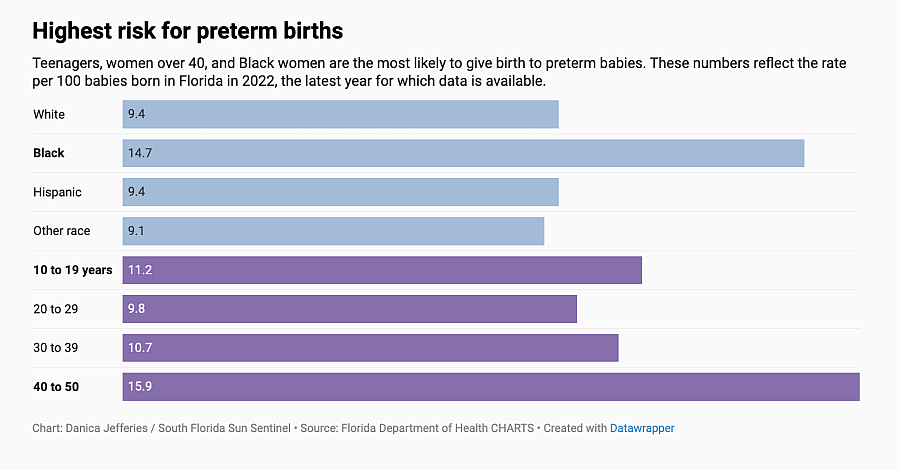
Black mothers are at higher risk
The causes of preterm births are varied, but one factor holds true throughout the nation: The preterm birth rate for babies born to Black women is higher — 1.6 times higher in Florida, for example — than non-Hispanic white women and Hispanic women. So too is the rate of low-weight births.
Some researchers say preterm labor among Black women is a result of the many physical, psychological and social stressors, including racism, that they experience on a daily basis.
Others insist Florida fails mothers by not graduating more Black OB-GYNs, by allowing maternal healthcare deserts without providers to exist in Black communities, and by not educating doctors on the need to be attuned to health conditions that put Black mothers-to-be and their babies at risk.
On average, one in 10 babies in Florida is born premature, but in some rural counties, particularly those with a relatively large Black population like Escambia in the northwestern corner of the state, it’s even as high as one in six who are born at less than 32 weeks of gestation.
“These high rates are concerning because preterm birth is a major risk factor for infant mortality,” said Hudak, the neonatologist at UF Health-Jacksonville.
Health researchers have found at least half of all preterm births are preventable. Mothers tend to give birth prematurely when they have risks like diabetes, kidney disease, hypertension and high stress levels. The risks also rise when they smoke or use drugs and alcohol while pregnant.
Shantay Davis suffered from hypertension when she became pregnant. Throughout her pregnancy, her blood pressure periodically skyrocketed. He doctor didn’t seem concerned. Then her amniotic fluid level dropped. She went to the Jackson Memorial Hospital emergency department to get checked.
“When I got to the hospital, the doctor said I don’t want you to have her yet. It’s too soon,” Johnson said. “But my blood pressure kept going up. It went up to 200, and 45 minutes after I got there I had an emergency C-section.”
The March of Dimes estimates about 75% of Florida counties have a high burden of women with chronic health conditions and a high rate of preterm birth.

Maya Sanchez and her daughter Lydia get a big hug from Dr. Chaas Gantt, founder of Palm Beach Regenerative Medicine at the Community Birth Wellness Festival & Midwife360 Family Reunion. The event at Dreher Park in West Palm Beach brought together families, midwives, doulas, and healthcare providers to celebrate family wellness, and featured workshops and demonstrations on natural childbirth, breastfeeding, postpartum care and holistic health. Outreach events such as this can help mothers and prospective mothers find the care and support they need when facing complicated pregnancies.
(Scott Luxor/Contributor)
When women with health issues arrive at a hospital having never seen a doctor, they may face life-threatening complications. About one of every four women who give birth prematurely are medically induced or require an emergency cesarean section to save their life, or their baby’s.
“We have to deliver these babies preterm just to decrease maternal mortality, which is still a big problem in the Black population,” explained Dr. Karen Young, director of the Newborn Intensive Care Unit at Holtz Children’s Hospital at the University of Miami/Jackson Memorial Medical Center.
No one knows for certain why the rate of preterm births is rising in the U.S. and Florida, but several trends may contribute: More people are having children later in life, and there has been an increase in people having multiple births, occasionally through in-vitro fertilization (IVF). Other contributing factors play a role, too, such as environment, chronic stress, anxiety, lack of emotional support, unstable housing and poor nutrition.
“I think it’s also education,” said Dr. Delisa Skeete Henry, an obstetrician practicing in South Florida. “Some doctors just don’t do a good job educating women on what they need to do to prevent preterm birth, nutrition, assessing their environment, and risk factors for delivering early.
“I’m sure it’s multifactorial. I don’t know that we can pinpoint one cause. It’s probably a combination of all of it.”
In addition to the little ones born preterm, some of the sickest babies are born full term but underweight, which can be less than 3 pounds, 5 ounces. At these weights, the tiny baby may have a harder time eating, gaining weight and fighting infections.
Mothers who smoke, eat poorly or become anemic during pregnancy often give birth to underweight babies that need specialized care in a NICU.
In 2022, the last year for which finalized data is available, 1 in 11 babies in Florida were low birthweight. And, between 2012 and 2022, the rate of infants born low birthweight in Florida increased nearly 6%, according to Florida Department of Health records.
“That’s concerning, “ said Wood, the Harvard researcher. “Those babies will need more resources and support to have good outcomes, and that may be challenging. The causes that put them in an environment to be born low birthweight are still there, so it becomes more challenging to get the resources they need.”
To bring those rates down, health experts want to see government leaders explore what drives poor birth outcomes within communities — and address them.

Dr. Stevenson Chery, medical director at BCOM Health, a government-funded health clinic in West Park in Broward County, speaks at a Black Maternal Health forum at the Dr. Martin Luther King, Jr. Community Center in Hollywood on April 6, 2024. The forum helped raise awareness about reducing maternal deaths among Black women, a group three times more likely to die from a pregnancy-related factor.
(Mike Stocker/South Florida Sun Sentinel)
Chery, the director of the Broward health clinic, treats a mostly Haitian population at the federally funded facility. He says every Black community has different contributors to poor birth outcomes. Applying a blanket solution in Florida to the rising rates of preterm and low birthweights won’t work.
“In Florida we just stay at the state level and make decisions and spend money where we think it should go to address the issues,” Chery said. “But you have to listen to the community. That’s the way to know the exact needs and wants that will address these problems.”
Medical interventions keep babies alive, but at a cost
When babies arrive early, specialists in Florida’s neonatal intensive care units work 24/7 to keep the small human beings alive, performing life-saving measures impossible just a decade ago.
With new interventions, doctors can save babies earlier in a woman’s pregnancy — as early as 22 weeks — resuscitating them at birth and placing small breathing tubes in their airways. Some experts think that has helped to keep the infant mortality rate down.
Yet when these extremely premature infants, often referred to as “micro-preemies,” need a high level of care, that must happen at a hospital with a neonatal intensive care unit equipped with the newest technology and staffed with specialists. The Florida Department of Health in its State Health Improvement Plan has set a goal to increase the percentage of very low birthweight infants born in a hospital with a Level 3 neonatal intensive care unit from 78% in 2020 to 86% by 2026.
However, 38 of Florida’s 67 counties don’t have a single neonatal intensive care unit. Although one in 10 babies in Florida is born premature, only 16 counties in Florida have a Level 3 NICU and even fewer, six, have a Level 4 NICU that provides the highest level of specialized care.

Babies weighing just ounces may spend their earliest and most precarious moments being transported and fighting to live without their parents by their side, in a hospital’s NICU an hour or more away.
Even when a transfer is successful to a hospital with a NICU, about 40% of all babies will die from preterm-related causes, a percentage higher in Florida than the national average of 36%.
Keeping babies alive in the NICU often requires millions of dollars annually in intensive-care costs from taxpayer funds. In Florida, 44% of births are babies on Medicaid, meaning the cost of care comes from state and federal money.
Nationally, one preterm baby averages $71,158 in neonatal intensive care costs, and the average NICU admission is 14 days, according to the Health Care Cost Institute’s review of 2017-2021 commercial claims data. In cases where infants require prolonged stays or multiple surgeries, the cost can soar to hundreds of thousands of dollars. Families with private insurance typically incur the out-of-pocket costs.
After discharge, potential lifelong disabilities can be costly, too.
Babies born prematurely can have short-term health issues like difficulty fighting off infection as well as breathing and feeding issues because their lungs and stomachs aren’t fully developed. They may also have long-term issues such as risk for lung infections, digestive issues, disabilities such as cerebral palsy, vision and hearing problems, and developmental and intellectual delays.
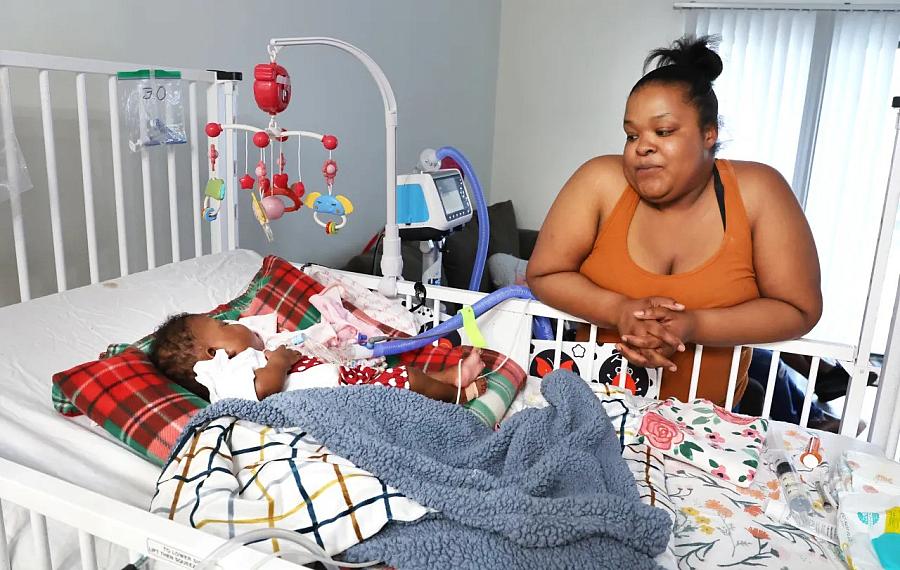
T’kyia White with her daughter Darionna Williams at their Fort Myers home. “It’s a lot of work … it’s challenging but you get through it,” White says. “It’s tough, though.”
(Carline Jean/South Florida Sun Sentinel)
Caring for a premature baby requires a parent like White to go to months if not years of follow-up appointments, learn how to operate medical equipment, and navigate a complex maze of public services — if and when they are available.
The responsibilities can be particularly difficult to navigate in Florida for low-income parents who may lack transportation to travel to appointments, don’t have a grasp of the English language, live in rural areas, or can’t afford to miss work to visit doctors.
“Even though it’s a long NICU stay, of course, the parents always want their babies to go home,” said Dr. Beatriz De Jongh, associate medical director of the NICU at Golisano Children’s Hospital in Fort Myers. “That’s what they’re thinking and hoping for. But when they go home, there is a lot of follow-up. Oftentimes, it is a full-time job for parents.”
Readmission rates to hospitals are high for preterm babies. De Jongh said odds are likely 11-month-old Darionna will be readmitted to Golisano in her first years of life. “If she got sick or she has a cold, she has a high likelihood she’ll have to be readmitted.”
Whether families are able to access resources such as home-visiting programs or financial aid can make a difference in their babies’ long-term prognosis.
“So many of the issues we are trying to think about are not just the first month of life when it’s life or death, but afterward, too,” said Wood, the Harvard researcher. “The resources in the home or community may make the difference in the health outcomes.”
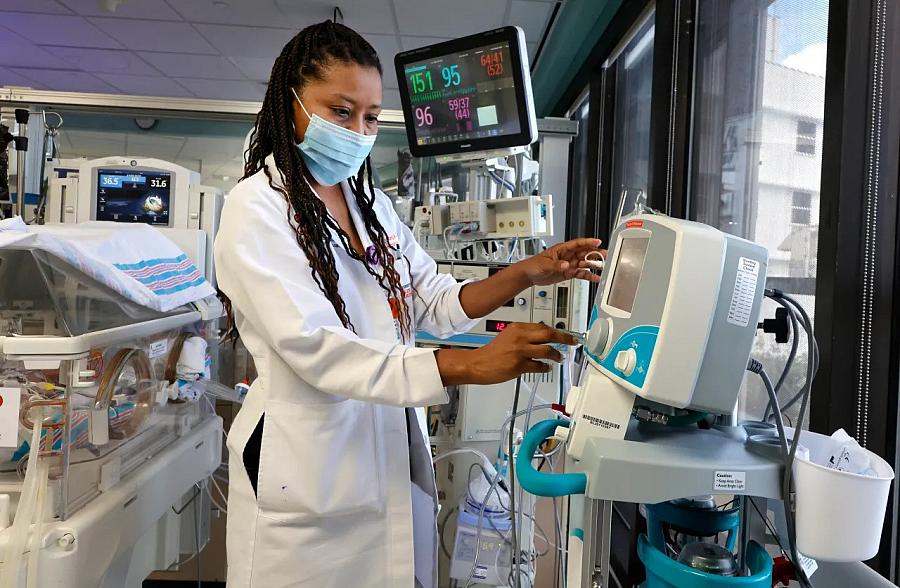
Dr. Karen Young, director of the Newborn Intensive Care Unit at Holtz Children’s Hospital at Jackson Memorial Medical Center in Miami, monitors a NICU patient.
(Carline Jean/South Florida Sun Sentinel)
Young, at Holtz Children’s Hospital at Jackson Memorial Medical Center in Miami, cares for these fragile babies, some transported from birthing centers or nearby hospitals without a specialized intensive care unit. One baby has been in Jackson’s NICU for almost a year, although the average stay is three to six months.
The doctor worries about the future for these small human beings, particularly those born before 25 weeks.
“The good news is neonatology has advanced significantly and we can save more babies. However, what we don’t know, because we haven’t studied them enough, is what are the long-term consequences of being born early?” Young said. “For example, will they be prone to obesity in adulthood or have an increased risk of Alzheimer’s? We don’t know yet if being born early programs all these other things.”
On her shift in the NICU, Young moves among tiny bassinets and peers into one in particular where a baby boy in a blue knit cap has tubes protruding from his throat, stomach and foot. His head is the size of an apple. His hands are the size of a pecan. His diaper is the size of a cocktail napkin.
He weighs 400 grams, not even a pound.
The tube in his tiny throat draws oxygen from a ventilator, supplying air to breathe. The one in his stomach gives him nutrients to grow, and the one from his head monitors for brain bleeds that often occur when a baby arrives before organs fully form. Born at 24 weeks, each day brings new threats to his life.

Dr. Karen Young, director of the Newborn Intensive Care Unit at Holtz Children’s Hospital at Jackson Memorial Medical Center in Miami, inside the NICU bay. “The good news is neonatology has advanced significantly and we can save more babies. However, what we don’t know, because we haven’t studied them enough, is what are the long-term consequences of being born early?” Young says.
(Carline Jean/South Florida Sun Sentinel)
A lot of development happens in late stages of pregnancy: The kidneys and lungs mature; the bones harden; vision and hearing improves.
Young and her team of cardiologists, pulmonologists and pediatric specialists rotate between the baby in the blue cap and as many as a hundred others fighting a battle to stay alive. The same battles happen in the 41 other NICUs in Florida continuously at capacity.
“This is the future if we don’t address this problem,” she said. “We will have children with health issues for years to come.”
The toll of a premature birth
A premature birth easily can keep families at near-poverty levels and dealing with stressful emotional conflicts like divorce and mental health breakdowns.
In Miramar, Yoanka Garcia and her family are teetering on eviction from the home they rent. Garcia has spent the last year taking her daughter Liberty Belle to medical appointments and surgeries, all while overseeing a household with three older children.

Liberty Belle Mazzarese was born weighing only 1 pound, 4 ounces.
(Yoanka Garcia/courtesy)
After Garcia went into labor at only 24 weeks, doctors delivered Liberty Belle via emergency C-section. She arrived weighing only 1 pound 4 ounces and spent 135 tumultuous days — a third of her first year — in the NICU before she was discharged.
At home, Liberty Belle sits in her mother’s lap, clapping to a tune that signals her favorite TV show is about to begin. Garcia lets out a sigh as she begins to describe the last year.
Financially, the Garcia family barely scraped by. They no longer have a car that runs, unable to afford repairs. Garcia said she is fighting with her daughter’s Medicaid health plan over the NICU bill for $93,000. She arranges transportation with Liberty Belle’s insurance but still takes buses or Uber with Liberty Belle to get diapers and special formula and to some of her appointments.
“I’m so overwhelmed with everything,” she said. “I don’t have any family nearby. I am trying to get back on my feet. We are most likely going to be evicted because we can’t make ends meet.”

Christopher and Yoanka Garcia with their baby Liberty Belle are serenaded by the NICU staff at Joe DiMaggio Children’s Hospital in Hollywood as they prepare to leave in December 2022. Liberty Belle was born 16 weeks early, weighing only 1 pound, 4 ounces, and spent four months in the NICU at the hospital.
(Mike Stocker/South Florida Sun Sentinel file)
Liberty Belle came home from the hospital in a frilly red Christmas dress, with a breathing tube in her nose and an oxygen tank. Each week for the last year, she returned to Joe DiMaggio Children’s Hospital in Hollywood where she had fought to make it through her first months of life. She saw a cardiologist, a pulmonologist and a pediatrician. Earlier this year, she had surgery on her eyes, a common complication with premature babies.
“There was a point where we were going every two weeks to the eye doctor. We were also going to the rehab center and they were measuring her head. She almost had to wear a helmet because she started to get a flat back, but then she learned how to sit up and that was it,” Garcia said.
“Now we do physical therapy and occupational therapy,” Garcia said. “We were going to three or four appointments a week. Now we go every Wednesday.”

Liberty Belle Mazzarese, now 1, weighed 1 pound, 4 ounces, when she was born. She was released to go to her Miramar home after 135 days in the NICU.
(Carline Jean/South Florida Sun Sentinel)
The refrain repeats itself all across Florida as mothers like Garcia navigate the complex and costly care their babies need.
At Golisano Children’s Hospital in Fort Myers, where Darionna was born, case workers help parents navigate complicated forms and requirements to get the medical and financial support to transition home.
“As much as we try to make them knowledgeable and make connections for them, we need parents to be independent and take the steps and stay on top of the resources,” case worker Chelsea Vanness said.
In rural counties in Florida, resources like at-home rehabilitative services are less available and drive times to specialists are longer, making it nearly impossible for families without a car to attend all the appointments. Language presents a barrier too. Also, daycare can be particularly challenging when a premature baby’s immune system is fragile.
Case workers say a big threat to a baby released from the NICU often is the mother’s mental health. Numerous studies reveal mothers of premature infants experience higher rates of postpartum depression than mothers of full-term infants.
“Babies who are born preterm, those parents have a high risk of depression, high risk that they will separate from partners because of added stress at home,” said Dr. Young at Jackson in Miami. “And in terms of earnings, this is a baby who may need added care at home, and for some parents they don’t have the resources to get another person to come in and help. That means they can’t work. These become significant problems.”

Yoanka Garcia, 37, of Miramar with her 1-year-old daughter, Liberty Belle Mazzarese.
(Carline Jean/South Florida Sun Sentinel)
Florida has extended Medicaid coverage for mothers after giving birth from 60 days to a year. Young says that policy shift is important because it allows women a greater chance to remain healthy between pregnancies.
However, it’s just the first step.
“In Florida, there’s a shortage of psychologists, especially who will accept Medicaid,” said Elizabeth Simonton, co-founder of ICU Baby. “If a mom doesn’t feel well mentally, it’s not a matter what resources are available for her baby because she is not going to access them.”
After her own personal experience with a premature infant, Simonton started ICU Baby to give emotional, financial and informational support to NICU families in Miami. Often, her volunteers translate medical information for parents who speak languages other than English.
“We have seen how hard it is for parents to manage complex medical care,” she said.
When these tiny babies grow, so can their special needs.
It has been 14 years since Kaleb Moore was born, a 1-pound, 10-ounce bundle with only one kidney and undeveloped lungs. His parents Marcus and Rosie Moore spent the first six months of their baby’s life praying for Kaleb’s survival in the NICU at Advent Health in Orlando.
“We were seeing the grief of other parents whose baby had died,” Marcus Moore said. “Kaleb had a 5% chance of survival.”
Today, Kaleb is an eighth-grader who has a learning disability and spends half his school day in a classroom for students with special needs. At school, he receives supplemental reading help from a specialist.
Life with Kaleb has been overwhelming at times for the Moores. Long after their worries about simply keeping him alive faded, the Moores faced new concerns. There were emergency trips to the hospital for lung infections or to reinsert the feeding tube he had pulled out. There were struggles to afford the high cost of special formula, and trips to see specialists for various therapies.
Marcus Moore said the high level of care Kaleb needed tested their marriage and put the family on the verge of bankruptcy. “The tension is always there,” he said.
“I ended up leaving my job to take care of Kaleb. We didn’t pay our mortgage for quite a while. We almost lost our house … from 2009 to 2014 … those years were tough.”
Moore and his wife have formed The Gift of Life 27 charity to help other parents of premature infants. They solicit donations and deliver care packages to parents of babies in Central Florida NICUs. As the rate of premature births in Florida rises, Moore delivers preemie hats and other items to NICUs that are continuously full of babies.
“The need is only going to get greater,” he said.


